Have a language expert improve your writing
Run a free plagiarism check in 10 minutes, generate accurate citations for free.
- Knowledge Base
Methodology
- What Is a Focus Group? | Step-by-Step Guide & Examples

What is a Focus Group | Step-by-Step Guide & Examples
Published on December 10, 2021 by Tegan George . Revised on June 22, 2023.
A focus group is a research method that brings together a small group of people to answer questions in a moderated setting. The group is chosen due to predefined demographic traits, and the questions are designed to shed light on a topic of interest.

Table of contents
What is a focus group, step 1: choose your topic of interest, step 2: define your research scope and hypotheses, step 3: determine your focus group questions, step 4: select a moderator or co-moderator, step 5: recruit your participants, step 6: set up your focus group, step 7: host your focus group, step 8: analyze your data and report your results, advantages and disadvantages of focus groups, other interesting articles, frequently asked questions about focus groups.
Focus groups are a type of qualitative research . Observations of the group’s dynamic, their answers to focus group questions, and even their body language can guide future research on consumer decisions, products and services, or controversial topics.
Focus groups are often used in marketing, library science, social science, and user research disciplines. They can provide more nuanced and natural feedback than individual interviews and are easier to organize than experiments or large-scale surveys .
Here's why students love Scribbr's proofreading services
Discover proofreading & editing
Focus groups are primarily considered a confirmatory research technique . In other words, their discussion-heavy setting is most useful for confirming or refuting preexisting beliefs. For this reason, they are great for conducting explanatory research , where you explore why something occurs when limited information is available.
A focus group may be a good choice for you if:
- You’re interested in real-time, unfiltered responses on a given topic or in the dynamics of a discussion between participants
- Your questions are rooted in feelings or perceptions , and cannot easily be answered with “yes” or “no”
- You’re confident that a relatively small number of responses will answer your question
- You’re seeking directional information that will help you uncover new questions or future research ideas
- Structured interviews : The questions are predetermined in both topic and order.
- Semi-structured interviews : A few questions are predetermined, but other questions aren’t planned.
- Unstructured interviews : None of the questions are predetermined.
Differences between types of interviews
Make sure to choose the type of interview that suits your research best. This table shows the most important differences between the four types.
| Structured interview | Semi-structured interview | Unstructured interview | Focus group | |
|---|---|---|---|---|
| Fixed questions | ||||
| Fixed order of questions | ||||
| Fixed number of questions | ||||
| Option to ask additional questions |
Topics favorable to focus groups
As a rule of thumb, research topics related to thoughts, beliefs, and feelings work well in focus groups. If you are seeking direction, explanation, or in-depth dialogue, a focus group could be a good fit.
However, if your questions are dichotomous or if you need to reach a large audience quickly, a survey may be a better option. If your question hinges upon behavior but you are worried about influencing responses, consider an observational study .
- If you want to determine whether the student body would regularly consume vegan food, a survey would be a great way to gauge student preferences.
However, food is much more than just consumption and nourishment and can have emotional, cultural, and other implications on individuals.
- If you’re interested in something less concrete, such as students’ perceptions of vegan food or the interplay between their choices at the dining hall and their feelings of homesickness or loneliness, perhaps a focus group would be best.
Once you have determined that a focus group is the right choice for your topic, you can start thinking about what you expect the group discussion to yield.
Perhaps literature already exists on your subject or a sufficiently similar topic that you can use as a starting point. If the topic isn’t well studied, use your instincts to determine what you think is most worthy of study.
Setting your scope will help you formulate intriguing hypotheses , set clear questions, and recruit the right participants.
- Are you interested in a particular sector of the population, such as vegans or non-vegans?
- Are you interested in including vegetarians in your analysis?
- Perhaps not all students eat at the dining hall. Will your study exclude those who don’t?
- Are you only interested in students who have strong opinions on the subject?
A benefit of focus groups is that your hypotheses can be open-ended. You can be open to a wide variety of opinions, which can lead to unexpected conclusions.
The questions that you ask your focus group are crucially important to your analysis. Take your time formulating them, paying special attention to phrasing. Be careful to avoid leading questions , which can affect your responses.
Overall, your focus group questions should be:
- Open-ended and flexible
- Impossible to answer with “yes” or “no” (questions that start with “why” or “how” are often best)
- Unambiguous, getting straight to the point while still stimulating discussion
- Unbiased and neutral
If you are discussing a controversial topic, be careful that your questions do not cause social desirability bias . Here, your respondents may lie about their true beliefs to mask any socially unacceptable or unpopular opinions. This and other demand characteristics can hurt your analysis and lead to several types of reseach bias in your results, particularly if your participants react in a different way once knowing they’re being observed. These include self-selection bias , the Hawthorne effect , the Pygmalion effect , and recall bias .
- Engagement questions make your participants feel comfortable and at ease: “What is your favorite food at the dining hall?”
- Exploration questions drill down to the focus of your analysis: “What pros and cons of offering vegan options do you see?”
- Exit questions pick up on anything you may have previously missed in your discussion: “Is there anything you’d like to mention about vegan options in the dining hall that we haven’t discussed?”
Prevent plagiarism. Run a free check.
It is important to have more than one moderator in the room. If you would like to take the lead asking questions, select a co-moderator who can coordinate the technology, take notes, and observe the behavior of the participants.
If your hypotheses have behavioral aspects, consider asking someone else to be lead moderator so that you are free to take a more observational role.
Depending on your topic, there are a few types of moderator roles that you can choose from.
- The most common is the dual-moderator , introduced above.
- Another common option is the dueling-moderator style . Here, you and your co-moderator take opposing sides on an issue to allow participants to see different perspectives and respond accordingly.
Depending on your research topic, there are a few sampling methods you can choose from to help you recruit and select participants.
- Voluntary response sampling , such as posting a flyer on campus and finding participants based on responses
- Convenience sampling of those who are most readily accessible to you, such as fellow students at your university
- Stratified sampling of a particular age, race, ethnicity, gender identity, or other characteristic of interest to you
- Judgment sampling of a specific set of participants that you already know you want to include
Beware of sampling bias and selection bias , which can occur when some members of the population are more likely to be included than others.
Number of participants
In most cases, one focus group will not be sufficient to answer your research question. It is likely that you will need to schedule three to four groups. A good rule of thumb is to stop when you’ve reached a saturation point (i.e., when you aren’t receiving new responses to your questions).
Most focus groups have 6–10 participants. It’s a good idea to over-recruit just in case someone doesn’t show up. As a rule of thumb, you shouldn’t have fewer than 6 or more than 12 participants, in order to get the most reliable results.
Lastly, it’s preferable for your participants not to know you or each other, as this can bias your results.
A focus group is not just a group of people coming together to discuss their opinions. While well-run focus groups have an enjoyable and relaxed atmosphere, they are backed up by rigorous methods to provide robust observations.
Confirm a time and date
Be sure to confirm a time and date with your participants well in advance. Focus groups usually meet for 45–90 minutes, but some can last longer. However, beware of the possibility of wandering attention spans. If you really think your session needs to last longer than 90 minutes, schedule a few breaks.
Confirm whether it will take place in person or online
You will also need to decide whether the group will meet in person or online. If you are hosting it in person, be sure to pick an appropriate location.
- An uncomfortable or awkward location may affect the mood or level of participation of your group members.
- Online sessions are convenient, as participants can join from home, but they can also lessen the connection between participants.
As a general rule, make sure you are in a noise-free environment that minimizes distractions and interruptions to your participants.
Consent and ethical considerations
It’s important to take into account ethical considerations and informed consent when conducting your research. Informed consent means that participants possess all the information they need to decide whether they want to participate in the research before it starts. This includes information about benefits, risks, funding, and institutional approval.
Participants should also sign a release form that states that they are comfortable with being audio- or video-recorded. While verbal consent may be sufficient, it is best to ask participants to sign a form.
A disadvantage of focus groups is that they are too small to provide true anonymity to participants. Make sure that your participants know this prior to participating.
There are a few things you can do to commit to keeping information private. You can secure confidentiality by removing all identifying information from your report or offer to pseudonymize the data later. Data pseudonymization entails replacing any identifying information about participants with pseudonymous or false identifiers.
Preparation prior to participation
If there is something you would like participants to read, study, or prepare beforehand, be sure to let them know well in advance. It’s also a good idea to call them the day before to ensure they will still be participating.
Consider conducting a tech check prior to the arrival of your participants, and note any environmental or external factors that could affect the mood of the group that day. Be sure that you are organized and ready, as a stressful atmosphere can be distracting and counterproductive.
Starting the focus group
Welcome individuals to the focus group by introducing the topic, yourself, and your co-moderator, and go over any ground rules or suggestions for a successful discussion. It’s important to make your participants feel at ease and forthcoming with their responses.
Consider starting out with an icebreaker, which will allow participants to relax and settle into the space a bit. Your icebreaker can be related to your study topic or not; it’s just an exercise to get participants talking.
Leading the discussion
Once you start asking your questions, try to keep response times equal between participants. Take note of the most and least talkative members of the group, as well as any participants with particularly strong or dominant personalities.
You can ask less talkative members questions directly to encourage them to participate or ask participants questions by name to even the playing field. Feel free to ask participants to elaborate on their answers or to give an example.
As a moderator, strive to remain neutral . Refrain from reacting to responses, and be aware of your body language (e.g., nodding, raising eyebrows) and the possibility for observer bias . Active listening skills, such as parroting back answers or asking for clarification, are good methods to encourage participation and signal that you’re listening.
Many focus groups offer a monetary incentive for participants. Depending on your research budget, this is a nice way to show appreciation for their time and commitment. To keep everyone feeling fresh, consider offering snacks or drinks as well.
After concluding your focus group, you and your co-moderator should debrief, recording initial impressions of the discussion as well as any highlights, issues, or immediate conclusions you’ve drawn.
The next step is to transcribe and clean your data . Assign each participant a number or pseudonym for organizational purposes. Transcribe the recordings and conduct content analysis to look for themes or categories of responses. The categories you choose can then form the basis for reporting your results.
Just like other research methods, focus groups come with advantages and disadvantages.
- They are fairly straightforward to organize and results have strong face validity .
- They are usually inexpensive, even if you compensate participant.
- A focus group is much less time-consuming than a survey or experiment , and you get immediate results.
- Focus group results are often more comprehensible and intuitive than raw data.
Disadvantages
- It can be difficult to assemble a truly representative sample. Focus groups are generally not considered externally valid due to their small sample sizes.
- Due to the small sample size, you cannot ensure the anonymity of respondents, which may influence their desire to speak freely.
- Depth of analysis can be a concern, as it can be challenging to get honest opinions on controversial topics.
- There is a lot of room for error in the data analysis and high potential for observer dependency in drawing conclusions. You have to be careful not to cherry-pick responses to fit a prior conclusion.
If you want to know more about statistics , methodology , or research bias , make sure to check out some of our other articles with explanations and examples.
- Student’s t -distribution
- Normal distribution
- Null and Alternative Hypotheses
- Chi square tests
- Confidence interval
- Quartiles & Quantiles
- Cluster sampling
- Stratified sampling
- Data cleansing
- Reproducibility vs Replicability
- Peer review
- Prospective cohort study
Research bias
- Implicit bias
- Cognitive bias
- Placebo effect
- Hawthorne effect
- Hindsight bias
- Affect heuristic
- Social desirability bias
A focus group is a research method that brings together a small group of people to answer questions in a moderated setting. The group is chosen due to predefined demographic traits, and the questions are designed to shed light on a topic of interest. It is one of 4 types of interviews .
As a rule of thumb, questions related to thoughts, beliefs, and feelings work well in focus groups. Take your time formulating strong questions, paying special attention to phrasing. Be careful to avoid leading questions , which can bias your responses.
There are various approaches to qualitative data analysis , but they all share five steps in common:
- Prepare and organize your data.
- Review and explore your data.
- Develop a data coding system.
- Assign codes to the data.
- Identify recurring themes.
The specifics of each step depend on the focus of the analysis. Some common approaches include textual analysis , thematic analysis , and discourse analysis .
Every dataset requires different techniques to clean dirty data , but you need to address these issues in a systematic way. You focus on finding and resolving data points that don’t agree or fit with the rest of your dataset.
These data might be missing values, outliers, duplicate values, incorrectly formatted, or irrelevant. You’ll start with screening and diagnosing your data. Then, you’ll often standardize and accept or remove data to make your dataset consistent and valid.
The four most common types of interviews are:
- Structured interviews : The questions are predetermined in both topic and order.
- Focus group interviews : The questions are presented to a group instead of one individual.
It’s impossible to completely avoid observer bias in studies where data collection is done or recorded manually, but you can take steps to reduce this type of bias in your research .
Scope of research is determined at the beginning of your research process , prior to the data collection stage. Sometimes called “scope of study,” your scope delineates what will and will not be covered in your project. It helps you focus your work and your time, ensuring that you’ll be able to achieve your goals and outcomes.
Defining a scope can be very useful in any research project, from a research proposal to a thesis or dissertation . A scope is needed for all types of research: quantitative , qualitative , and mixed methods .
To define your scope of research, consider the following:
- Budget constraints or any specifics of grant funding
- Your proposed timeline and duration
- Specifics about your population of study, your proposed sample size , and the research methodology you’ll pursue
- Any inclusion and exclusion criteria
- Any anticipated control , extraneous , or confounding variables that could bias your research if not accounted for properly.
Cite this Scribbr article
If you want to cite this source, you can copy and paste the citation or click the “Cite this Scribbr article” button to automatically add the citation to our free Citation Generator.
George, T. (2023, June 22). What is a Focus Group | Step-by-Step Guide & Examples. Scribbr. Retrieved September 18, 2024, from https://www.scribbr.com/methodology/focus-group/
Is this article helpful?
Tegan George
Other students also liked, what is qualitative research | methods & examples, explanatory research | definition, guide, & examples, data collection | definition, methods & examples, get unlimited documents corrected.
✔ Free APA citation check included ✔ Unlimited document corrections ✔ Specialized in correcting academic texts
Instant insights, infinite possibilities
7 focus group examples for your next qualitative research project
Last updated
9 March 2023
Reviewed by
Jean Kaluza
Short on time? Get an AI generated summary of this article instead
Qualitative research is a fact-finding method for exploring and understanding people's beliefs, attitudes, experiences, and behaviors.
It involves collecting and analyzing data for insights into complex phenomena and social issues.
Researchers take this detailed data and analyze it using techniques such as content analysis, thematic analysis, or grounded theory to identify patterns and themes in the data.
Qualitative research can inform policies, design interventions, or improve services.
Analyze focus group sessions
Dovetail streamlines focus group research to help you understand the responses and find patterns faster
- What is a focus group?
A focus group is a qualitative fact-finding method involving a small group of five to 10 people discussing a specific topic or issue. A moderator leads the group, poses open-ended questions, and encourages participant discussion and interaction.
A focus group aims to gain insights into participants' opinions, attitudes, beliefs, and behaviors about the discussed topic.
Marketing research, product development, and social sciences use focus groups to understand consumer behavior, attitudes, and preferences. They can also explore social issues, gather feedback on new ideas, or evaluate the effectiveness of a program or intervention.
You can conduct in-person or online focus groups and record and transcribe the sessions for analysis. You use thematic or content analysis to analyze the data and identify patterns in the participants' responses.
- Why do researchers use focus groups?
Researchers use focus groups for various reasons, primarily to gain qualitative insights and opinions from people with similar characteristics.
Here are other reasons for focus groups:
Understand consumer behavior
Focus groups are ideal in marketing research for gathering insights into consumer preferences and behavior. Researchers can better understand what motivates their target audience, needs, wants, and what drives their purchasing decisions.
Gather feedback on new ideas
Focus groups can gather feedback on new products, services, or ideas. Researchers can present a new concept to a focus group and ask for their opinions to see how well they receive the idea. They can also learn what changes might be necessary and the potential market.
Evaluate the effectiveness of programs or interventions
Focus groups can help evaluate the effectiveness of a program or intervention. Researchers can ask participants to share their experiences and opinions to gain insights into their experience with the program. They can determine what aspects of the program work well, what could be improved, and its impact on participants.
Explore social issues
Focus groups can help explore social issues, such as attitudes toward a particular topic or the impact of a social program. Bringing together a diverse group of people can help researchers gain a more nuanced understanding of the issue and identify potential solutions or interventions.
Focus groups are a helpful tool for gaining qualitative insights and opinions from people with shared attributes. You can use these groups in different settings, and they’re handy for exploring complex issues that require in-depth understanding.
When should you use a focus group?
Here are some situations where a focus group might be appropriate:
If you’re launching a new product or service and want to gather feedback on your concept, features, and branding
To better understand your target audience's behavior, attitudes, and partiality by helping you identify patterns and trends in their decision-making
When you want to evaluate the effectiveness of a program or intervention by understanding the participant's experiences and opinions
If you want to develop effective marketing strategies with insights into what resonates with your target audience
When you want to explore social issues, such as the impact of a social program, and gain a deeper understanding of the issue at hand
Focus groups are less useful for situations where you need quantitative data or a representative sample of the broader population. It's essential to carefully plan your focus group, including selecting willing participants, choosing a moderator, and developing a discussion guide to achieve your research goals.
- 7 examples of focus groups
Researchers can use focus groups in different settings to gather feedback and opinions on products, services, or topics. Here are some examples of focus groups:
1. Product testing
Marketers can use a focus group to test a new product. For example, a company plans to launch a new line of skincare products and wants to get feedback from potential customers before the launch. The company organizes focus groups with participants who match their target market demographic and supplies a moderator with a discussion guide.
The moderator asks the focus group participants to try the products and provide feedback on the product's packaging, scent, texture, effectiveness, and overall appeal.
They question participants about their current skincare routine, what products they use, and what they look for in skincare products.
The company changes the product packaging, ingredients, and pricing based on feedback. This ensures the product meets the needs and preferences of the target market.
Now, the company can launch the new skincare line with confidence that its target market will love the product.
2. Advertising campaigns
Focus groups can test the success of advertising campaigns. Participants provide feedback on the ad's messaging, visuals, and tone, helping a company refine the campaign before launch.
For example, a brand organizes a focus group with participants who match their target demographic before launching their new advertising campaign.
If the focus group participants find the ad's message too complicated or unclear, the company can simplify the message based on feedback. This makes the ad more attractive and digestible for its target audience.
3. Political campaigns
Political participants can use focus groups to gather information about:
What issues are most important to voters
How voters feel about the candidate and their message
How the candidate can improve their message and campaign strategy
For example, a political campaign might convene a focus group of voters from a particular demographic, such as suburban women or young adults.
The leader might ask the focus group questions about their feelings and attitudes towards the candidate, the issues they care about most, and how they perceive the candidate's stance.
4. Market research
Marketers can use focus groups to gather information about consumers' likes and dislikes about a particular product or service. They can use this information to guide product development, marketing, and advertising strategies.
For example, a company forms a focus group to gather feedback on a new product concept, such as a new type of food packaging.
The moderator asks the focus group questions about their perceptions of the product, the likelihood of purchasing it, and any suggestions they have for improving it.
5. Product development
Focus groups can gather qualitative data from potential users or customers to understand their needs, preferences, and experiences with the product.
Companies can use focus groups at different stages, from the initial concept development to the testing and refinement of prototypes.
For example, a business gathers a focus group to provide feedback on a new music streaming service app, and participants answer questions about:
Their experiences with their current music streaming experiences
Preferences for layout
Impressions of the new streaming service
Product development teams can use this feedback to ensure the product meets the needs and expectations of the target market.
6. Healthcare
Healthcare focus groups can gather feedback and insights from patients, healthcare providers, and other stakeholders.
Healthcare providers can use focus groups to gather qualitative data on various topics, including patient experiences, healthcare delivery, policies, and products.
For example, a provider uses a focus group to gather feedback on a new healthcare policy related to access to care. Participants answer questions about their experiences accessing healthcare, opinions on the policy, and any suggestions for improvements.
7. Education
Educators can use focus groups to get insights into student experiences and preferences to improve the quality of education and student engagement.
Focus groups can also collect feedback from teachers and parents on issues such as teaching methods, parental involvement, and student performance.
Decision-makers can use this feedback to improve curriculum development, teaching methods, school policies, and educational products to meet the needs of students and educators.
- The pros and cons of focus groups
Focus groups are a popular research method to gather feedback and opinions from small, diverse groups. While focus groups can provide valuable insights, they also have drawbacks.
Provides in-depth insights
Focus groups allow in-depth discussions and more comprehensive insights into a topic. Participants can provide detailed feedback and share their opinions, attitudes, and experiences.
Encourages group dynamics
Focus groups encourage participants to interact and discuss the topic with each other, generating new ideas and insights. Participants can build on each other's thoughts and ideas, leading to a more extensive and nuanced discussion.
Cost-effective
Conducting a focus group can be less expensive than other research methods, such as one-on-one interviews or surveys . It can be more cost-effective to gather a group in one location rather than travel to different locations to conduct individual interviews.
Can be used to test ideas
Focus groups can test new ideas, products, or services before they launch. It allows companies to gather feedback from potential customers, enabling more informed decisions.
Flexibility
Researchers can adapt focus groups to various topics and settings, from academic research to market research.
The moderator can conduct focus groups quickly, making them a valuable tool for gathering data in a short amount of time.
Small sample size
Focus groups usually involve a small number of participants. The opinions of a focus group may not represent the broader population.
Potential bias
Group dynamics can influence the opinions and attitudes of a focus group, so they may not reflect the opinions of individual participants.
Limited scope
Focus groups may only provide insights into a specific topic or product instead of broader insights into consumer behavior or attitudes.
Time-consuming
Conducting a focus group can be time-consuming, as it requires organizing and scheduling participants, setting up a location, and analyzing the data.
Interpretation
The interpretation of focus group data can be subjective and dependent on the researcher's perspective and biases.
Researchers should use focus groups and other research methods to ensure comprehensive and accurate findings.
- How do you run a focus group?
Here are some steps to follow when running a focus group:
Before planning your focus group, define your research objectives and determine what you hope to achieve through the focus group.
Determine your target audience by categorizing them with common characteristics to provide the necessary insights.
Identify potential participants that fit your target audience, offer an incentive to encourage participation, and recruit them for the focus group.
Select a skilled moderator to facilitate the discussion and keep it focused. The moderator should understand qualitative research techniques and have good interpersonal skills.
Develop a discussion guide outlining the questions for the focus group. The questions should elicit insights and opinions from participants on the research objectives.
Hold the focus group in a comfortable, quiet location. Introduce the moderator and explain the purpose of the focus group. The moderator should guide the discussion, asking questions from the discussion guide and encouraging participation from everyone.
Record the discussion using audio or video recording equipment. Consider taking notes during the discussion to capture critical points.
Transcribe the audio or video recording and analyze the data to identify patterns and themes.
Use the data to draw conclusions and make recommendations based on the research objectives. Use techniques such as content analysis , thematic analysis , or grounded theory to identify patterns and themes in the data.
Prepare a report summarizing the findings of the focus group and provide recommendations based on the research objectives.
Follow these steps to conduct a successful focus group, uncover valuable insights, and achieve your research objectives.
- Five sample focus group questions
Here are some sample focus group questions that you could use in different research contexts avoiding leading questions and emphasizing open-ended questions:
1. Exploring a new product or service:
What are your first impressions of this product/service?
What do you like/dislike about the product/service?
How does this product/service compare to similar products/services?
What improvements could we make to the product/service?
2. Understanding consumer behavior:
What factors influence your decision to purchase a product/service?
How do you typically research products/services before making a purchase?
How do you feel about the pricing of products/services?
How do you use technology when shopping for products/services?
3. Evaluating the effectiveness of a program or intervention:
What do you think are the strengths of the program/intervention?
What challenges have you faced in participating in the program/intervention?
How has the program/intervention impacted your life?
What changes would you recommend to improve the program/intervention?
4. Developing marketing strategies:
What messages do you think would resonate with your target audience?
What channels do you think are most effective for reaching your target audience?
What motivates your target audience to make a purchase?
How do you think your target audience perceives your brand?
5. Exploring social issues:
What are your attitudes toward [topic]?
How has [topic] impacted your life or those you know?
What are some potential solutions to address [topic]?
What are some barriers to addressing [topic]?
These are just a few examples of questions that you could use in focus groups. Carefully design questions relevant to the research objectives that elicit meaningful participant insights.
Should you be using a customer insights hub?
Do you want to discover previous research faster?
Do you share your research findings with others?
Do you analyze research data?
Start for free today, add your research, and get to key insights faster
Editor’s picks
Last updated: 18 April 2023
Last updated: 27 February 2023
Last updated: 22 August 2024
Last updated: 5 February 2023
Last updated: 16 August 2024
Last updated: 9 March 2023
Last updated: 30 April 2024
Last updated: 12 December 2023
Last updated: 11 March 2024
Last updated: 4 July 2024
Last updated: 6 March 2024
Last updated: 5 March 2024
Last updated: 13 May 2024
Latest articles
Related topics, .css-je19u9{-webkit-align-items:flex-end;-webkit-box-align:flex-end;-ms-flex-align:flex-end;align-items:flex-end;display:-webkit-box;display:-webkit-flex;display:-ms-flexbox;display:flex;-webkit-flex-direction:row;-ms-flex-direction:row;flex-direction:row;-webkit-box-flex-wrap:wrap;-webkit-flex-wrap:wrap;-ms-flex-wrap:wrap;flex-wrap:wrap;-webkit-box-pack:center;-ms-flex-pack:center;-webkit-justify-content:center;justify-content:center;row-gap:0;text-align:center;max-width:671px;}@media (max-width: 1079px){.css-je19u9{max-width:400px;}.css-je19u9>span{white-space:pre;}}@media (max-width: 799px){.css-je19u9{max-width:400px;}.css-je19u9>span{white-space:pre;}} decide what to .css-1kiodld{max-height:56px;display:-webkit-box;display:-webkit-flex;display:-ms-flexbox;display:flex;-webkit-align-items:center;-webkit-box-align:center;-ms-flex-align:center;align-items:center;}@media (max-width: 1079px){.css-1kiodld{display:none;}} build next, decide what to build next, log in or sign up.
Get started for free
- Privacy Policy

Home » Focus Groups – Steps, Examples and Guide
Focus Groups – Steps, Examples and Guide
Table of Contents

Focus Group
Definition:
A focus group is a qualitative research method used to gather in-depth insights and opinions from a group of individuals about a particular product, service, concept, or idea.
The focus group typically consists of 6-10 participants who are selected based on shared characteristics such as demographics, interests, or experiences. The discussion is moderated by a trained facilitator who asks open-ended questions to encourage participants to share their thoughts, feelings, and attitudes towards the topic.
Focus groups are an effective way to gather detailed information about consumer behavior, attitudes, and perceptions, and can provide valuable insights to inform decision-making in a range of fields including marketing, product development, and public policy.
Types of Focus Group
The following are some types or methods of Focus Groups:
Traditional Focus Group
This is the most common type of focus group, where a small group of people is brought together to discuss a particular topic. The discussion is typically led by a skilled facilitator who asks open-ended questions to encourage participants to share their thoughts and opinions.
Mini Focus Group
A mini-focus group involves a smaller group of participants, typically 3 to 5 people. This type of focus group is useful when the topic being discussed is particularly sensitive or when the participants are difficult to recruit.
Dual Moderator Focus Group
In a dual-moderator focus group, two facilitators are used to manage the discussion. This can help to ensure that the discussion stays on track and that all participants have an opportunity to share their opinions.
Teleconference or Online Focus Group
Teleconferences or online focus groups are conducted using video conferencing technology or online discussion forums. This allows participants to join the discussion from anywhere in the world, making it easier to recruit participants and reducing the cost of conducting the focus group.
Client-led Focus Group
In a client-led focus group, the client who is commissioning the research takes an active role in the discussion. This type of focus group is useful when the client has specific questions they want to ask or when they want to gain a deeper understanding of their customers.
The following Table can explain Focus Group types more clearly
| Type of Focus Group | Number of Participants | Duration | Types of Questions | Geographical Area | Analysis Type |
|---|---|---|---|---|---|
| Traditional | 6-12 | 1-2 hours | Open-ended | Local | Thematic Analysis |
| Mini | 3-5 | 1-2 hours | Closed-ended | Local | Content Analysis |
| Dual Moderator | 6-12 | 1-2 hours | Combination of open- and closed-ended | Regional | Discourse Analysis |
| Teleconference/Online | 6-12 | 1-2 hours | Open-ended | National/International | Conversation Analysis |
| Client-Led | 6-12 | 1-2 hours | Combination of open- and closed-ended | Local/Regional | Thematic Analy |
How To Conduct a Focus Group
To conduct a focus group, follow these general steps:
Define the Research Question
Identify the key research question or objective that you want to explore through the focus group. Develop a discussion guide that outlines the topics and questions you want to cover during the session.
Recruit Participants
Identify the target audience for the focus group and recruit participants who meet the eligibility criteria. You can use various recruitment methods such as social media, online panels, or referrals from existing customers.
Select a Venue
Choose a location that is convenient for the participants and has the necessary facilities such as audio-visual equipment, seating, and refreshments.
Conduct the Session
During the focus group session, introduce the topic, and review the objectives of the research. Encourage participants to share their thoughts and opinions by asking open-ended questions and probing deeper into their responses. Ensure that the discussion remains on topic and that all participants have an opportunity to contribute.
Record the Session
Use audio or video recording equipment to capture the discussion. Note-taking is also essential to ensure that you capture all key points and insights.
Analyze the data
Once the focus group is complete, transcribe and analyze the data. Look for common themes, patterns, and insights that emerge from the discussion. Use this information to generate insights and recommendations that can be applied to the research question.
When to use Focus Group Method
The focus group method is typically used in the following situations:
Exploratory Research
When a researcher wants to explore a new or complex topic in-depth, focus groups can be used to generate ideas, opinions, and insights.
Product Development
Focus groups are often used to gather feedback from consumers about new products or product features to help identify potential areas for improvement.
Marketing Research
Focus groups can be used to test marketing concepts, messaging, or advertising campaigns to determine their effectiveness and appeal to different target audiences.
Customer Feedback
Focus groups can be used to gather feedback from customers about their experiences with a particular product or service, helping companies improve customer satisfaction and loyalty.
Public Policy Research
Focus groups can be used to gather public opinions and attitudes on social or political issues, helping policymakers make more informed decisions.
Examples of Focus Group
Here are some real-time examples of focus groups:
- A tech company wants to improve the user experience of their mobile app. They conduct a focus group with a diverse group of users to gather feedback on the app’s design, functionality, and features. The focus group consists of 8 participants who are selected based on their age, gender, ethnicity, and level of experience with the app. During the session, a trained facilitator asks open-ended questions to encourage participants to share their thoughts and opinions on the app. The facilitator also observes the participants’ behavior and reactions to the app’s features. After the focus group, the data is analyzed to identify common themes and issues raised by the participants. The insights gathered from the focus group are used to inform improvements to the app’s design and functionality, with the goal of creating a more user-friendly and engaging experience for all users.
- A car manufacturer wants to develop a new electric vehicle that appeals to a younger demographic. They conduct a focus group with millennials to gather their opinions on the design, features, and pricing of the vehicle.
- A political campaign team wants to develop effective messaging for their candidate’s campaign. They conduct a focus group with voters to gather their opinions on key issues and identify the most persuasive arguments and messages.
- A restaurant chain wants to develop a new menu that appeals to health-conscious customers. They conduct a focus group with fitness enthusiasts to gather their opinions on the types of food and drinks that they would like to see on the menu.
- A healthcare organization wants to develop a new wellness program for their employees. They conduct a focus group with employees to gather their opinions on the types of programs, incentives, and support that would be most effective in promoting healthy behaviors.
- A clothing retailer wants to develop a new line of sustainable and eco-friendly clothing. They conduct a focus group with environmentally conscious consumers to gather their opinions on the design, materials, and pricing of the clothing.
Purpose of Focus Group
The key objectives of a focus group include:
Generating New Ideas and insights
Focus groups are used to explore new or complex topics in-depth, generating new ideas and insights that may not have been previously considered.
Understanding Consumer Behavior
Focus groups can be used to gather information on consumer behavior, attitudes, and perceptions to inform marketing and product development strategies.
Testing Concepts and Ideas
Focus groups can be used to test marketing concepts, messaging, or product prototypes to determine their effectiveness and appeal to different target audiences.
Gathering Customer Feedback
Informing decision-making.
Focus groups can provide valuable insights to inform decision-making in a range of fields including marketing, product development, and public policy.
Advantages of Focus Group
The advantages of using focus groups are:
- In-depth insights: Focus groups provide in-depth insights into the attitudes, opinions, and behaviors of a target audience on a specific topic, allowing researchers to gain a deeper understanding of the issues being explored.
- Group dynamics: The group dynamics of focus groups can provide additional insights, as participants may build on each other’s ideas, share experiences, and debate different perspectives.
- Efficient data collection: Focus groups are an efficient way to collect data from multiple individuals at the same time, making them a cost-effective method of research.
- Flexibility : Focus groups can be adapted to suit a range of research objectives, from exploratory research to concept testing and customer feedback.
- Real-time feedback: Focus groups provide real-time feedback on new products or concepts, allowing researchers to make immediate adjustments and improvements based on participant feedback.
- Participant engagement: Focus groups can be a more engaging and interactive research method than surveys or other quantitative methods, as participants have the opportunity to express their opinions and interact with other participants.
Limitations of Focus Groups
While focus groups can provide valuable insights, there are also some limitations to using them.
- Small sample size: Focus groups typically involve a small number of participants, which may not be representative of the broader population being studied.
- Group dynamics : While group dynamics can be an advantage of focus groups, they can also be a limitation, as dominant personalities may sway the discussion or participants may not feel comfortable expressing their true opinions.
- Limited generalizability : Because focus groups involve a small sample size, the results may not be generalizable to the broader population.
- Limited depth of responses: Because focus groups are time-limited, participants may not have the opportunity to fully explore or elaborate on their opinions or experiences.
- Potential for bias: The facilitator of a focus group may inadvertently influence the discussion or the selection of participants may not be representative, leading to potential bias in the results.
- Difficulty in analysis : The qualitative data collected in focus groups can be difficult to analyze, as it is often subjective and requires a skilled researcher to interpret and identify themes.
Characteristics of Focus Group
- Small group size: Focus groups typically involve a small number of participants, ranging from 6 to 12 people. This allows for a more in-depth and focused discussion.
- Targeted participants: Participants in focus groups are selected based on specific criteria, such as age, gender, or experience with a particular product or service.
- Facilitated discussion: A skilled facilitator leads the discussion, asking open-ended questions and encouraging participants to share their thoughts and experiences.
- I nteractive and conversational: Focus groups are interactive and conversational, with participants building on each other’s ideas and responding to one another’s opinions.
- Qualitative data: The data collected in focus groups is qualitative, providing detailed insights into participants’ attitudes, opinions, and behaviors.
- Non-threatening environment: Participants are encouraged to share their thoughts and experiences in a non-threatening and supportive environment.
- Limited time frame: Focus groups are typically time-limited, lasting between 1 and 2 hours, to ensure that the discussion stays focused and productive.
About the author
Muhammad Hassan
Researcher, Academic Writer, Web developer
You may also like

Quasi-Experimental Research Design – Types...

Textual Analysis – Types, Examples and Guide

Explanatory Research – Types, Methods, Guide

Experimental Design – Types, Methods, Guide

Phenomenology – Methods, Examples and Guide

Basic Research – Types, Methods and Examples
Thank you for visiting nature.com. You are using a browser version with limited support for CSS. To obtain the best experience, we recommend you use a more up to date browser (or turn off compatibility mode in Internet Explorer). In the meantime, to ensure continued support, we are displaying the site without styles and JavaScript.
- View all journals
- Explore content
- About the journal
- Publish with us
- Sign up for alerts
- Published: 05 October 2018
Interviews and focus groups in qualitative research: an update for the digital age
- P. Gill 1 &
- J. Baillie 2
British Dental Journal volume 225 , pages 668–672 ( 2018 ) Cite this article
33k Accesses
63 Citations
20 Altmetric
Metrics details
Highlights that qualitative research is used increasingly in dentistry. Interviews and focus groups remain the most common qualitative methods of data collection.
Suggests the advent of digital technologies has transformed how qualitative research can now be undertaken.
Suggests interviews and focus groups can offer significant, meaningful insight into participants' experiences, beliefs and perspectives, which can help to inform developments in dental practice.
Qualitative research is used increasingly in dentistry, due to its potential to provide meaningful, in-depth insights into participants' experiences, perspectives, beliefs and behaviours. These insights can subsequently help to inform developments in dental practice and further related research. The most common methods of data collection used in qualitative research are interviews and focus groups. While these are primarily conducted face-to-face, the ongoing evolution of digital technologies, such as video chat and online forums, has further transformed these methods of data collection. This paper therefore discusses interviews and focus groups in detail, outlines how they can be used in practice, how digital technologies can further inform the data collection process, and what these methods can offer dentistry.
You have full access to this article via your institution.
Similar content being viewed by others

Interviews in the social sciences

Professionalism in dentistry: deconstructing common terminology
A review of technical and quality assessment considerations of audio-visual and web-conferencing focus groups in qualitative health research, introduction.
Traditionally, research in dentistry has primarily been quantitative in nature. 1 However, in recent years, there has been a growing interest in qualitative research within the profession, due to its potential to further inform developments in practice, policy, education and training. Consequently, in 2008, the British Dental Journal (BDJ) published a four paper qualitative research series, 2 , 3 , 4 , 5 to help increase awareness and understanding of this particular methodological approach.
Since the papers were originally published, two scoping reviews have demonstrated the ongoing proliferation in the use of qualitative research within the field of oral healthcare. 1 , 6 To date, the original four paper series continue to be well cited and two of the main papers remain widely accessed among the BDJ readership. 2 , 3 The potential value of well-conducted qualitative research to evidence-based practice is now also widely recognised by service providers, policy makers, funding bodies and those who commission, support and use healthcare research.
Besides increasing standalone use, qualitative methods are now also routinely incorporated into larger mixed method study designs, such as clinical trials, as they can offer additional, meaningful insights into complex problems that simply could not be provided by quantitative methods alone. Qualitative methods can also be used to further facilitate in-depth understanding of important aspects of clinical trial processes, such as recruitment. For example, Ellis et al . investigated why edentulous older patients, dissatisfied with conventional dentures, decline implant treatment, despite its established efficacy, and frequently refuse to participate in related randomised clinical trials, even when financial constraints are removed. 7 Through the use of focus groups in Canada and the UK, the authors found that fears of pain and potential complications, along with perceived embarrassment, exacerbated by age, are common reasons why older patients typically refuse dental implants. 7
The last decade has also seen further developments in qualitative research, due to the ongoing evolution of digital technologies. These developments have transformed how researchers can access and share information, communicate and collaborate, recruit and engage participants, collect and analyse data and disseminate and translate research findings. 8 Where appropriate, such technologies are therefore capable of extending and enhancing how qualitative research is undertaken. 9 For example, it is now possible to collect qualitative data via instant messaging, email or online/video chat, using appropriate online platforms.
These innovative approaches to research are therefore cost-effective, convenient, reduce geographical constraints and are often useful for accessing 'hard to reach' participants (for example, those who are immobile or socially isolated). 8 , 9 However, digital technologies are still relatively new and constantly evolving and therefore present a variety of pragmatic and methodological challenges. Furthermore, given their very nature, their use in many qualitative studies and/or with certain participant groups may be inappropriate and should therefore always be carefully considered. While it is beyond the scope of this paper to provide a detailed explication regarding the use of digital technologies in qualitative research, insight is provided into how such technologies can be used to facilitate the data collection process in interviews and focus groups.
In light of such developments, it is perhaps therefore timely to update the main paper 3 of the original BDJ series. As with the previous publications, this paper has been purposely written in an accessible style, to enhance readability, particularly for those who are new to qualitative research. While the focus remains on the most common qualitative methods of data collection – interviews and focus groups – appropriate revisions have been made to provide a novel perspective, and should therefore be helpful to those who would like to know more about qualitative research. This paper specifically focuses on undertaking qualitative research with adult participants only.
Overview of qualitative research
Qualitative research is an approach that focuses on people and their experiences, behaviours and opinions. 10 , 11 The qualitative researcher seeks to answer questions of 'how' and 'why', providing detailed insight and understanding, 11 which quantitative methods cannot reach. 12 Within qualitative research, there are distinct methodologies influencing how the researcher approaches the research question, data collection and data analysis. 13 For example, phenomenological studies focus on the lived experience of individuals, explored through their description of the phenomenon. Ethnographic studies explore the culture of a group and typically involve the use of multiple methods to uncover the issues. 14
While methodology is the 'thinking tool', the methods are the 'doing tools'; 13 the ways in which data are collected and analysed. There are multiple qualitative data collection methods, including interviews, focus groups, observations, documentary analysis, participant diaries, photography and videography. Two of the most commonly used qualitative methods are interviews and focus groups, which are explored in this article. The data generated through these methods can be analysed in one of many ways, according to the methodological approach chosen. A common approach is thematic data analysis, involving the identification of themes and subthemes across the data set. Further information on approaches to qualitative data analysis has been discussed elsewhere. 1
Qualitative research is an evolving and adaptable approach, used by different disciplines for different purposes. Traditionally, qualitative data, specifically interviews, focus groups and observations, have been collected face-to-face with participants. In more recent years, digital technologies have contributed to the ongoing evolution of qualitative research. Digital technologies offer researchers different ways of recruiting participants and collecting data, and offer participants opportunities to be involved in research that is not necessarily face-to-face.
Research interviews are a fundamental qualitative research method 15 and are utilised across methodological approaches. Interviews enable the researcher to learn in depth about the perspectives, experiences, beliefs and motivations of the participant. 3 , 16 Examples include, exploring patients' perspectives of fear/anxiety triggers in dental treatment, 17 patients' experiences of oral health and diabetes, 18 and dental students' motivations for their choice of career. 19
Interviews may be structured, semi-structured or unstructured, 3 according to the purpose of the study, with less structured interviews facilitating a more in depth and flexible interviewing approach. 20 Structured interviews are similar to verbal questionnaires and are used if the researcher requires clarification on a topic; however they produce less in-depth data about a participant's experience. 3 Unstructured interviews may be used when little is known about a topic and involves the researcher asking an opening question; 3 the participant then leads the discussion. 20 Semi-structured interviews are commonly used in healthcare research, enabling the researcher to ask predetermined questions, 20 while ensuring the participant discusses issues they feel are important.
Interviews can be undertaken face-to-face or using digital methods when the researcher and participant are in different locations. Audio-recording the interview, with the consent of the participant, is essential for all interviews regardless of the medium as it enables accurate transcription; the process of turning the audio file into a word-for-word transcript. This transcript is the data, which the researcher then analyses according to the chosen approach.
Types of interview
Qualitative studies often utilise one-to-one, face-to-face interviews with research participants. This involves arranging a mutually convenient time and place to meet the participant, signing a consent form and audio-recording the interview. However, digital technologies have expanded the potential for interviews in research, enabling individuals to participate in qualitative research regardless of location.
Telephone interviews can be a useful alternative to face-to-face interviews and are commonly used in qualitative research. They enable participants from different geographical areas to participate and may be less onerous for participants than meeting a researcher in person. 15 A qualitative study explored patients' perspectives of dental implants and utilised telephone interviews due to the quality of the data that could be yielded. 21 The researcher needs to consider how they will audio record the interview, which can be facilitated by purchasing a recorder that connects directly to the telephone. One potential disadvantage of telephone interviews is the inability of the interviewer and researcher to see each other. This is resolved using software for audio and video calls online – such as Skype – to conduct interviews with participants in qualitative studies. Advantages of this approach include being able to see the participant if video calls are used, enabling observation of non-verbal communication, and the software can be free to use. However, participants are required to have a device and internet connection, as well as being computer literate, potentially limiting who can participate in the study. One qualitative study explored the role of dental hygienists in reducing oral health disparities in Canada. 22 The researcher conducted interviews using Skype, which enabled dental hygienists from across Canada to be interviewed within the research budget, accommodating the participants' schedules. 22
A less commonly used approach to qualitative interviews is the use of social virtual worlds. A qualitative study accessed a social virtual world – Second Life – to explore the health literacy skills of individuals who use social virtual worlds to access health information. 23 The researcher created an avatar and interview room, and undertook interviews with participants using voice and text methods. 23 This approach to recruitment and data collection enables individuals from diverse geographical locations to participate, while remaining anonymous if they wish. Furthermore, for interviews conducted using text methods, transcription of the interview is not required as the researcher can save the written conversation with the participant, with the participant's consent. However, the researcher and participant need to be familiar with how the social virtual world works to engage in an interview this way.
Conducting an interview
Ensuring informed consent before any interview is a fundamental aspect of the research process. Participants in research must be afforded autonomy and respect; consent should be informed and voluntary. 24 Individuals should have the opportunity to read an information sheet about the study, ask questions, understand how their data will be stored and used, and know that they are free to withdraw at any point without reprisal. The qualitative researcher should take written consent before undertaking the interview. In a face-to-face interview, this is straightforward: the researcher and participant both sign copies of the consent form, keeping one each. However, this approach is less straightforward when the researcher and participant do not meet in person. A recent protocol paper outlined an approach for taking consent for telephone interviews, which involved: audio recording the participant agreeing to each point on the consent form; the researcher signing the consent form and keeping a copy; and posting a copy to the participant. 25 This process could be replicated in other interview studies using digital methods.
There are advantages and disadvantages of using face-to-face and digital methods for research interviews. Ultimately, for both approaches, the quality of the interview is determined by the researcher. 16 Appropriate training and preparation are thus required. Healthcare professionals can use their interpersonal communication skills when undertaking a research interview, particularly questioning, listening and conversing. 3 However, the purpose of an interview is to gain information about the study topic, 26 rather than offering help and advice. 3 The researcher therefore needs to listen attentively to participants, enabling them to describe their experience without interruption. 3 The use of active listening skills also help to facilitate the interview. 14 Spradley outlined elements and strategies for research interviews, 27 which are a useful guide for qualitative researchers:
Greeting and explaining the project/interview
Asking descriptive (broad), structural (explore response to descriptive) and contrast (difference between) questions
Asymmetry between the researcher and participant talking
Expressing interest and cultural ignorance
Repeating, restating and incorporating the participant's words when asking questions
Creating hypothetical situations
Asking friendly questions
Knowing when to leave.
For semi-structured interviews, a topic guide (also called an interview schedule) is used to guide the content of the interview – an example of a topic guide is outlined in Box 1 . The topic guide, usually based on the research questions, existing literature and, for healthcare professionals, their clinical experience, is developed by the research team. The topic guide should include open ended questions that elicit in-depth information, and offer participants the opportunity to talk about issues important to them. This is vital in qualitative research where the researcher is interested in exploring the experiences and perspectives of participants. It can be useful for qualitative researchers to pilot the topic guide with the first participants, 10 to ensure the questions are relevant and understandable, and amending the questions if required.
Regardless of the medium of interview, the researcher must consider the setting of the interview. For face-to-face interviews, this could be in the participant's home, in an office or another mutually convenient location. A quiet location is preferable to promote confidentiality, enable the researcher and participant to concentrate on the conversation, and to facilitate accurate audio-recording of the interview. For interviews using digital methods the same principles apply: a quiet, private space where the researcher and participant feel comfortable and confident to participate in an interview.
Box 1: Example of a topic guide
Study focus: Parents' experiences of brushing their child's (aged 0–5) teeth
1. Can you tell me about your experience of cleaning your child's teeth?
How old was your child when you started cleaning their teeth?
Why did you start cleaning their teeth at that point?
How often do you brush their teeth?
What do you use to brush their teeth and why?
2. Could you explain how you find cleaning your child's teeth?
Do you find anything difficult?
What makes cleaning their teeth easier for you?
3. How has your experience of cleaning your child's teeth changed over time?
Has it become easier or harder?
Have you changed how often and how you clean their teeth? If so, why?
4. Could you describe how your child finds having their teeth cleaned?
What do they enjoy about having their teeth cleaned?
Is there anything they find upsetting about having their teeth cleaned?
5. Where do you look for information/advice about cleaning your child's teeth?
What did your health visitor tell you about cleaning your child's teeth? (If anything)
What has the dentist told you about caring for your child's teeth? (If visited)
Have any family members given you advice about how to clean your child's teeth? If so, what did they tell you? Did you follow their advice?
6. Is there anything else you would like to discuss about this?
Focus groups
A focus group is a moderated group discussion on a pre-defined topic, for research purposes. 28 , 29 While not aligned to a particular qualitative methodology (for example, grounded theory or phenomenology) as such, focus groups are used increasingly in healthcare research, as they are useful for exploring collective perspectives, attitudes, behaviours and experiences. Consequently, they can yield rich, in-depth data and illuminate agreement and inconsistencies 28 within and, where appropriate, between groups. Examples include public perceptions of dental implants and subsequent impact on help-seeking and decision making, 30 and general dental practitioners' views on patient safety in dentistry. 31
Focus groups can be used alone or in conjunction with other methods, such as interviews or observations, and can therefore help to confirm, extend or enrich understanding and provide alternative insights. 28 The social interaction between participants often results in lively discussion and can therefore facilitate the collection of rich, meaningful data. However, they are complex to organise and manage, due to the number of participants, and may also be inappropriate for exploring particularly sensitive issues that many participants may feel uncomfortable about discussing in a group environment.
Focus groups are primarily undertaken face-to-face but can now also be undertaken online, using appropriate technologies such as email, bulletin boards, online research communities, chat rooms, discussion forums, social media and video conferencing. 32 Using such technologies, data collection can also be synchronous (for example, online discussions in 'real time') or, unlike traditional face-to-face focus groups, asynchronous (for example, online/email discussions in 'non-real time'). While many of the fundamental principles of focus group research are the same, regardless of how they are conducted, a number of subtle nuances are associated with the online medium. 32 Some of which are discussed further in the following sections.
Focus group considerations
Some key considerations associated with face-to-face focus groups are: how many participants are required; should participants within each group know each other (or not) and how many focus groups are needed within a single study? These issues are much debated and there is no definitive answer. However, the number of focus groups required will largely depend on the topic area, the depth and breadth of data needed, the desired level of participation required 29 and the necessity (or not) for data saturation.
The optimum group size is around six to eight participants (excluding researchers) but can work effectively with between three and 14 participants. 3 If the group is too small, it may limit discussion, but if it is too large, it may become disorganised and difficult to manage. It is, however, prudent to over-recruit for a focus group by approximately two to three participants, to allow for potential non-attenders. For many researchers, particularly novice researchers, group size may also be informed by pragmatic considerations, such as the type of study, resources available and moderator experience. 28 Similar size and mix considerations exist for online focus groups. Typically, synchronous online focus groups will have around three to eight participants but, as the discussion does not happen simultaneously, asynchronous groups may have as many as 10–30 participants. 33
The topic area and potential group interaction should guide group composition considerations. Pre-existing groups, where participants know each other (for example, work colleagues) may be easier to recruit, have shared experiences and may enjoy a familiarity, which facilitates discussion and/or the ability to challenge each other courteously. 3 However, if there is a potential power imbalance within the group or if existing group norms and hierarchies may adversely affect the ability of participants to speak freely, then 'stranger groups' (that is, where participants do not already know each other) may be more appropriate. 34 , 35
Focus group management
Face-to-face focus groups should normally be conducted by two researchers; a moderator and an observer. 28 The moderator facilitates group discussion, while the observer typically monitors group dynamics, behaviours, non-verbal cues, seating arrangements and speaking order, which is essential for transcription and analysis. The same principles of informed consent, as discussed in the interview section, also apply to focus groups, regardless of medium. However, the consent process for online discussions will probably be managed somewhat differently. For example, while an appropriate participant information leaflet (and consent form) would still be required, the process is likely to be managed electronically (for example, via email) and would need to specifically address issues relating to technology (for example, anonymity and use, storage and access to online data). 32
The venue in which a face to face focus group is conducted should be of a suitable size, private, quiet, free from distractions and in a collectively convenient location. It should also be conducted at a time appropriate for participants, 28 as this is likely to promote attendance. As with interviews, the same ethical considerations apply (as discussed earlier). However, online focus groups may present additional ethical challenges associated with issues such as informed consent, appropriate access and secure data storage. Further guidance can be found elsewhere. 8 , 32
Before the focus group commences, the researchers should establish rapport with participants, as this will help to put them at ease and result in a more meaningful discussion. Consequently, researchers should introduce themselves, provide further clarity about the study and how the process will work in practice and outline the 'ground rules'. Ground rules are designed to assist, not hinder, group discussion and typically include: 3 , 28 , 29
Discussions within the group are confidential to the group
Only one person can speak at a time
All participants should have sufficient opportunity to contribute
There should be no unnecessary interruptions while someone is speaking
Everyone can be expected to be listened to and their views respected
Challenging contrary opinions is appropriate, but ridiculing is not.
Moderating a focus group requires considered management and good interpersonal skills to help guide the discussion and, where appropriate, keep it sufficiently focused. Avoid, therefore, participating, leading, expressing personal opinions or correcting participants' knowledge 3 , 28 as this may bias the process. A relaxed, interested demeanour will also help participants to feel comfortable and promote candid discourse. Moderators should also prevent the discussion being dominated by any one person, ensure differences of opinions are discussed fairly and, if required, encourage reticent participants to contribute. 3 Asking open questions, reflecting on significant issues, inviting further debate, probing responses accordingly, and seeking further clarification, as and where appropriate, will help to obtain sufficient depth and insight into the topic area.
Moderating online focus groups requires comparable skills, particularly if the discussion is synchronous, as the discussion may be dominated by those who can type proficiently. 36 It is therefore important that sufficient time and respect is accorded to those who may not be able to type as quickly. Asynchronous discussions are usually less problematic in this respect, as interactions are less instant. However, moderating an asynchronous discussion presents additional challenges, particularly if participants are geographically dispersed, as they may be online at different times. Consequently, the moderator will not always be present and the discussion may therefore need to occur over several days, which can be difficult to manage and facilitate and invariably requires considerable flexibility. 32 It is also worth recognising that establishing rapport with participants via online medium is often more challenging than via face-to-face and may therefore require additional time, skills, effort and consideration.
As with research interviews, focus groups should be guided by an appropriate interview schedule, as discussed earlier in the paper. For example, the schedule will usually be informed by the review of the literature and study aims, and will merely provide a topic guide to help inform subsequent discussions. To provide a verbatim account of the discussion, focus groups must be recorded, using an audio-recorder with a good quality multi-directional microphone. While videotaping is possible, some participants may find it obtrusive, 3 which may adversely affect group dynamics. The use (or not) of a video recorder, should therefore be carefully considered.
At the end of the focus group, a few minutes should be spent rounding up and reflecting on the discussion. 28 Depending on the topic area, it is possible that some participants may have revealed deeply personal issues and may therefore require further help and support, such as a constructive debrief or possibly even referral on to a relevant third party. It is also possible that some participants may feel that the discussion did not adequately reflect their views and, consequently, may no longer wish to be associated with the study. 28 Such occurrences are likely to be uncommon, but should they arise, it is important to further discuss any concerns and, if appropriate, offer them the opportunity to withdraw (including any data relating to them) from the study. Immediately after the discussion, researchers should compile notes regarding thoughts and ideas about the focus group, which can assist with data analysis and, if appropriate, any further data collection.
Qualitative research is increasingly being utilised within dental research to explore the experiences, perspectives, motivations and beliefs of participants. The contributions of qualitative research to evidence-based practice are increasingly being recognised, both as standalone research and as part of larger mixed-method studies, including clinical trials. Interviews and focus groups remain commonly used data collection methods in qualitative research, and with the advent of digital technologies, their utilisation continues to evolve. However, digital methods of qualitative data collection present additional methodological, ethical and practical considerations, but also potentially offer considerable flexibility to participants and researchers. Consequently, regardless of format, qualitative methods have significant potential to inform important areas of dental practice, policy and further related research.
Gussy M, Dickson-Swift V, Adams J . A scoping review of qualitative research in peer-reviewed dental publications. Int J Dent Hygiene 2013; 11 : 174–179.
Article Google Scholar
Burnard P, Gill P, Stewart K, Treasure E, Chadwick B . Analysing and presenting qualitative data. Br Dent J 2008; 204 : 429–432.
Gill P, Stewart K, Treasure E, Chadwick B . Methods of data collection in qualitative research: interviews and focus groups. Br Dent J 2008; 204 : 291–295.
Gill P, Stewart K, Treasure E, Chadwick B . Conducting qualitative interviews with school children in dental research. Br Dent J 2008; 204 : 371–374.
Stewart K, Gill P, Chadwick B, Treasure E . Qualitative research in dentistry. Br Dent J 2008; 204 : 235–239.
Masood M, Thaliath E, Bower E, Newton J . An appraisal of the quality of published qualitative dental research. Community Dent Oral Epidemiol 2011; 39 : 193–203.
Ellis J, Levine A, Bedos C et al. Refusal of implant supported mandibular overdentures by elderly patients. Gerodontology 2011; 28 : 62–68.
Macfarlane S, Bucknall T . Digital Technologies in Research. In Gerrish K, Lathlean J (editors) The Research Process in Nursing . 7th edition. pp. 71–86. Oxford: Wiley Blackwell; 2015.
Google Scholar
Lee R, Fielding N, Blank G . Online Research Methods in the Social Sciences: An Editorial Introduction. In Fielding N, Lee R, Blank G (editors) The Sage Handbook of Online Research Methods . pp. 3–16. London: Sage Publications; 2016.
Creswell J . Qualitative inquiry and research design: Choosing among five designs . Thousand Oaks, CA: Sage, 1998.
Guest G, Namey E, Mitchell M . Qualitative research: Defining and designing In Guest G, Namey E, Mitchell M (editors) Collecting Qualitative Data: A Field Manual For Applied Research . pp. 1–40. London: Sage Publications, 2013.
Chapter Google Scholar
Pope C, Mays N . Qualitative research: Reaching the parts other methods cannot reach: an introduction to qualitative methods in health and health services research. BMJ 1995; 311 : 42–45.
Giddings L, Grant B . A Trojan Horse for positivism? A critique of mixed methods research. Adv Nurs Sci 2007; 30 : 52–60.
Hammersley M, Atkinson P . Ethnography: Principles in Practice . London: Routledge, 1995.
Oltmann S . Qualitative interviews: A methodological discussion of the interviewer and respondent contexts Forum Qualitative Sozialforschung/Forum: Qualitative Social Research. 2016; 17 : Art. 15.
Patton M . Qualitative Research and Evaluation Methods . Thousand Oaks, CA: Sage, 2002.
Wang M, Vinall-Collier K, Csikar J, Douglas G . A qualitative study of patients' views of techniques to reduce dental anxiety. J Dent 2017; 66 : 45–51.
Lindenmeyer A, Bowyer V, Roscoe J, Dale J, Sutcliffe P . Oral health awareness and care preferences in patients with diabetes: a qualitative study. Fam Pract 2013; 30 : 113–118.
Gallagher J, Clarke W, Wilson N . Understanding the motivation: a qualitative study of dental students' choice of professional career. Eur J Dent Educ 2008; 12 : 89–98.
Tod A . Interviewing. In Gerrish K, Lacey A (editors) The Research Process in Nursing . Oxford: Blackwell Publishing, 2006.
Grey E, Harcourt D, O'Sullivan D, Buchanan H, Kipatrick N . A qualitative study of patients' motivations and expectations for dental implants. Br Dent J 2013; 214 : 10.1038/sj.bdj.2012.1178.
Farmer J, Peressini S, Lawrence H . Exploring the role of the dental hygienist in reducing oral health disparities in Canada: A qualitative study. Int J Dent Hygiene 2017; 10.1111/idh.12276.
McElhinney E, Cheater F, Kidd L . Undertaking qualitative health research in social virtual worlds. J Adv Nurs 2013; 70 : 1267–1275.
Health Research Authority. UK Policy Framework for Health and Social Care Research. Available at https://www.hra.nhs.uk/planning-and-improving-research/policies-standards-legislation/uk-policy-framework-health-social-care-research/ (accessed September 2017).
Baillie J, Gill P, Courtenay P . Knowledge, understanding and experiences of peritonitis among patients, and their families, undertaking peritoneal dialysis: A mixed methods study protocol. J Adv Nurs 2017; 10.1111/jan.13400.
Kvale S . Interviews . Thousand Oaks (CA): Sage, 1996.
Spradley J . The Ethnographic Interview . New York: Holt, Rinehart and Winston, 1979.
Goodman C, Evans C . Focus Groups. In Gerrish K, Lathlean J (editors) The Research Process in Nursing . pp. 401–412. Oxford: Wiley Blackwell, 2015.
Shaha M, Wenzell J, Hill E . Planning and conducting focus group research with nurses. Nurse Res 2011; 18 : 77–87.
Wang G, Gao X, Edward C . Public perception of dental implants: a qualitative study. J Dent 2015; 43 : 798–805.
Bailey E . Contemporary views of dental practitioners' on patient safety. Br Dent J 2015; 219 : 535–540.
Abrams K, Gaiser T . Online Focus Groups. In Field N, Lee R, Blank G (editors) The Sage Handbook of Online Research Methods . pp. 435–450. London: Sage Publications, 2016.
Poynter R . The Handbook of Online and Social Media Research . West Sussex: John Wiley & Sons, 2010.
Kevern J, Webb C . Focus groups as a tool for critical social research in nurse education. Nurse Educ Today 2001; 21 : 323–333.
Kitzinger J, Barbour R . Introduction: The Challenge and Promise of Focus Groups. In Barbour R S K J (editor) Developing Focus Group Research . pp. 1–20. London: Sage Publications, 1999.
Krueger R, Casey M . Focus Groups: A Practical Guide for Applied Research. 4th ed. Thousand Oaks, California: SAGE; 2009.
Download references
Author information
Authors and affiliations.
Senior Lecturer (Adult Nursing), School of Healthcare Sciences, Cardiff University,
Lecturer (Adult Nursing) and RCBC Wales Postdoctoral Research Fellow, School of Healthcare Sciences, Cardiff University,
You can also search for this author in PubMed Google Scholar
Corresponding author
Correspondence to P. Gill .
Rights and permissions
Reprints and permissions
About this article
Cite this article.
Gill, P., Baillie, J. Interviews and focus groups in qualitative research: an update for the digital age. Br Dent J 225 , 668–672 (2018). https://doi.org/10.1038/sj.bdj.2018.815
Download citation
Accepted : 02 July 2018
Published : 05 October 2018
Issue Date : 12 October 2018
DOI : https://doi.org/10.1038/sj.bdj.2018.815
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
This article is cited by
Assessment of women’s needs and wishes regarding interprofessional guidance on oral health in pregnancy – a qualitative study.
- Merle Ebinghaus
- Caroline Johanna Agricola
- Birgit-Christiane Zyriax
BMC Pregnancy and Childbirth (2024)
Translating brand reputation into equity from the stakeholder’s theory: an approach to value creation based on consumer’s perception & interactions
- Olukorede Adewole
International Journal of Corporate Social Responsibility (2024)
Perceptions and beliefs of community gatekeepers about genomic risk information in African cleft research
- Abimbola M. Oladayo
- Oluwakemi Odukoya
- Azeez Butali
BMC Public Health (2024)
Assessment of women’s needs, wishes and preferences regarding interprofessional guidance on nutrition in pregnancy – a qualitative study
‘baby mamas’ in urban ghana: an exploratory qualitative study on the factors influencing serial fathering among men in accra, ghana.
- Rosemond Akpene Hiadzi
- Jemima Akweley Agyeman
- Godwin Banafo Akrong
Reproductive Health (2023)
Quick links
- Explore articles by subject
- Guide to authors
- Editorial policies
- Skip to main content
- Skip to primary sidebar
- Skip to footer
- QuestionPro

- Solutions Industries Gaming Automotive Sports and events Education Government Travel & Hospitality Financial Services Healthcare Cannabis Technology Use Case AskWhy Communities Audience Contactless surveys Mobile LivePolls Member Experience GDPR Positive People Science 360 Feedback Surveys
- Resources Blog eBooks Survey Templates Case Studies Training Help center
Home Communities
Focus group: What It Is & How to Conduct It + Examples

In 1991, marketing and psychological expert Ernest Dichter coined the name “Focus Group.” The term described meetings held with a limited group of participants with the objective of discussion.
This interactive setting allows researchers to gain deeper insights into consumer behavior, attitudes, and preferences that might not emerge from other research methods like surveys or one-on-one interviews. Market research, product development, and public opinion studies often use focus groups to capture diverse viewpoints and uncover trends or issues that help inform decision-making.
The group’s purpose is not to arrive at a consensus or agreement on the topic. Instead, it seeks to identify and understand customer perceptions of a brand, product, or service. We’ll cover what a focus group is, how to conduct one, and example questions and best practices below.
What is a focus group?
A focus group is best defined as a small group of carefully selected participants who contribute to open discussions for research. The hosting organization carefully selects participants for the study to represent the larger population they’re attempting to target.
The group might look at new products, feature updates, or other topics of interest to generalize the entire population’s reaction. This research includes a moderator. Their job is to ensure legitimate results and reduce bias in the discussions.
- You use a focus group in qualitative research . A group of 6-10 people, usually 8, meet to explore and discuss a topic, such as a new product. The group shares their feedback, opinions, knowledge, and insights about the topic at hand.
- Participants openly share opinions and are free to convince other participants of their ideas.
- The mediator takes notes on the discussion and opinions of group members.
- The right group members affect the results of your research, so it’s vital to be picky when selecting members.
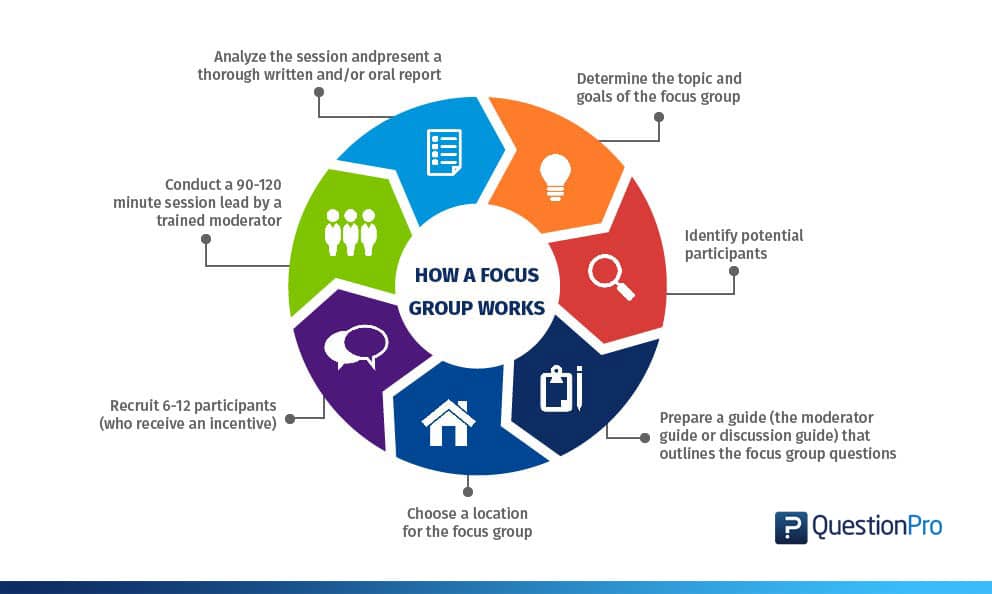
These groups possess a distinct advantage over other market research and market research methods. They capitalize on the moderator’s communication with participants and the flexibility to move the discussion. It allows you to extract meaningful insights and opinions.
Explore our latest article delving into real-world examples of qualitative data in education . Why not take a look and gather more insights from the valuable information we’ve shared?
LEARN ABOUT: Steps in Qualitative Research
Main pillars of a focus group
1. participant.
A crucial step in conducting a focus group is participant selection. The main criteria for selecting the participants must be their knowledge of the subject. If you need help selecting members, look for a market research-based organization that matches you with qualified participants.
2. The role of a moderator
The moderator conducts the focus group confidently and leads members through the questions. They must be impartial throughout the process. As the researcher, you can also be the moderator, so long as you remain objective. You can also hire a suitable professional moderator to run your survey.
Types of focus groups
Your choice of focus group depends on the needs of your action research . Types include:
- Dual moderator: There are two moderators for this event. One ensures smooth execution, and the other guarantees the discussion of each question.
- Two-way: A two-way group involves two separate groups having discussions on the topic at different times. As one group conducts its study, the other group observes the discussion. In the end, the group that observed the first session performed their conversation. The second group can use insights gained from watching the first discussion to dive deeper into the topic and offer more perspective.
- Mini: This type of small group restricts participants to 4-5 members instead of the usual 6-10.
- Client-involvement: Use this group when clients ask you to conduct a focus group and invite those who ask.
- Participant-moderated: One or more participants provisionally take up the role of moderator.
- Online: These groups employ online mediums to gather opinions and feedback. There are three categories of people in an online panel : observer, moderator, and respondent.
How to conduct a focus group
A focus group is a research method or technique that is used to collect opinions and ideas regarding a concept, service, or product. Follow the below steps to conduct it:

01. Recruit the right participants
A researcher must be careful while recruiting participants. Members need adequate knowledge of the topic to contribute to the conversation.
02. Choose a moderator
Your moderator should understand the topic of discussion and possess the following qualities:
- Ensures participation from all members of the group.
- Regulates dominant group members so others may speak.
- Motivates inattentive members through supportive words and positive body language.
- Should it become too heated, the executive decides to end or continue a discussion.
Verify that your moderator doesn’t know any of the participants. Existing relationships between a member and moderator can cause bias and skew your data.
03. Record the meeting for future purposes
Recording the sessions or meetings while conducting a focus group is essential. A researcher can record the discussion through audio or video. It would help to let participants know you’re planning to record the event and get their consent.
04. Write clear discussion guidelines
Writing down clear session guidelines before the session starts is crucial. Include key questions, expectations of focus group members, whether you’re recording the discussion, and methods of sharing results. Give out the instructions in advance and ask participants to comply with them.
05. Conduct the session and generate a report
Once participants understand their role, the moderator leads the survey. You can ask members to fill out a feedback form to collect quantitative data from the event. Use your data collection to generate reports on your study’s overall findings.
06. Use the data to make a plan of action
Share your report with stakeholders and decision-makers in your organization. The focus group feedback shows that a good report helps you design actionable plans to improve products or services. Update the group members on the changes you make and the results of those changes.
Focus Group Examples
Focus groups are common in three situations:
- Initial stages of a research study
- While creating a plan of action during research
- After the completion of the study to establish the results
For example, a laptop company needs customer feedback about an upcoming product. Focus group provides direct information about the marketing research from actual consumers.
The company chooses eight individuals representing their target market for a constructive discussion. The moderator asks questions regarding customer preference for laptop size and features. Group members discuss why they do or do not like certain aspects of a laptop. The company uses the opinions of the participants to create a product that fits customer needs and wants
Best practices for focus group research
Follow these five steps to create a market research focus group:
1. Have a clear plan for focus group members
The group’s goal must be clear before inviting participants to join. For example, does the researcher intend to discuss new products or the effect of current marketing campaigns? Use a written explanation to clarify the objective to members.
2. With a plan in place, begin writing your focus group survey questions
Questions should align with the research objective and complement one another. Start the discussion with the most crucial research problems and end with the least important ones. Asking open-ended questions increases the effectiveness of your research.
3. Schedule the time, place, and duration of the discussion
Be sure to inform members in advance so they can plan accordingly.
4. You can host it in person or through an online community
Offline groups meet in person at a physical location to conduct the discussion. An in-person event requires a venue that includes bathrooms and refreshments so participants are comfortable.
On the other hand, online groups meet virtually through an online discussion platform. Invitations and reminders for online discussions need to be sent out several times before the event. This helps participants remember your online event.
5. Create informational brochures or forum
Create informational brochures and posts with a welcome note, the meeting agenda, and the overall rules of the group discussion.
Focus group advantages and disadvantages
Focus group is a well-liked research technique due to its simple setup and the insightful data it can yield. It has advantages and disadvantages much, like other research techniques.
- A great complement to other mediums like online surveys and online polls . Focus groups give you access to why a customer feels a certain way about a product, and surveys help you collect supporting feedback in large batches.
- Immediate access to customer opinions, making data collection and analysis quick and convenient.
- Highly flexible to adapt to the needs and opinions of the group members.
- Easy to conduct regular discussions to eliminate inaccurate results due to current market outlooks.
- Focus groups are perfect sources to understand the true feelings and perceptions of your selected target audience.
Disadvantages
- Creating a representative sample is tough. Small-size sample makes focus groups unreliable.
- Due to the limited sample size, you cannot guarantee respondent anonymity, which may affect their willingness to speak freely.
- Getting honest opinions on sensitive topics can make the depth of analysis difficult.
- Data analysis is vulnerable to inaccuracy and observer research bias .
Focus group question examples
When using a focus group in market research , you must ask the right questions for accurate results. Good group questions have the following characteristics:
- A friendly and conversational tone
- Language or phrases that resonate with focus group participants
- Straightforward and accurate
- Each item includes one aspect and doesn’t merge multiple topics
- Clarify complex questions for more precise answers
Avoid asking questions to specific individuals to ensure the inclusion of all participants. Restrict discussion time per question to 5-20 minutes to keep the conversation efficient.
There are four categories:
1. Pr imary question: This first open-ended question initiates the entire discussion.
- We are here to discuss ____. What are your thoughts about it?
2. Probe questions: These questions dig deeper into the discussion of the primary question.
For example:
- What do you know about ____?
- How familiar are you with this organizational program?
- What do you love about our organization?
3. Questions to follow up : After establishing the overall knowledge and feelings of the group, the moderator identifies specific insights.
- What do you think are the pros and cons of this product?
- According to you, where can we improve to provide better customer service?
- Which factors prompted you to purchase our products/services?
- What is the likelihood of recommending our products to your friends and colleagues?
4. Questions for the conclusion: Review previous questions to avoid overlooking the main points. It is the time when a moderator can revisit specific topics to gather more data.
For example :
- Is there anything other than the already discussed questions you would like to talk about?
- Do you want to add to what is already spoken about?
Focus group questions to recruit participants
Here are some questions you may ask to recruit participants:
- Do you or any of your family members work in any of the following sectors?

- Select your age range:
- Kindly select your employment type:

- Please specify your level of education:

- Please state your family status:

Our focus group recruitment questionnaire template gives you a range of survey question types for maximum responses. These responses also help you make the best choice in recruiting the appropriate group members.
Best Online Focus Group Software: QuestionPro Communities
Online focus groups remove the need for a physical location. Like in-person groups, online groups involve 6-10 participants who share their opinions. Many researchers prefer online focus groups for convenience and cost-effectiveness.
QuestionPro Communities is an online focus group software . It’s a highly-effective market research tool that helps researchers find online focus groups for their research purposes, including market research.
QuestionPro Communities software includes:
- Discussions : Organizations invite participants to a moderated online discussion forum. Participants may answer questions at any time suitable to them.
- Idea Board : Idea Board allows respondents to share their ideas. Other group members can analyze, write feedback, and even vote on submissions.
- Topics : Users can submit topics, cast their votes in existing posts, and leave comments or feedback instantly.

Organizations can ensure that they gather the most valuable insights from their focus groups by carefully planning, recruiting, and conducting the sessions. The examples provided highlight the versatility of focus groups, highlighting the wide range of applications for this research method.
Organizations can gain a deeper understanding of their customers and make more informed decisions that drive success by leveraging the power of focus groups.
QuestionPro Communities is the only online focus group software available on desktop and mobile. Go mobile and take Discussions, Idea Board, and Topics anywhere your respondents go.
Start conducting online focus group surveys with participants from across the globe with QuestionPro Communities today.
Collect community feedback through our insights community software!
More like this.

QuestionPro: Leading the Charge in Customer Journey Management and Voice of the Customer Platforms
Sep 17, 2024

What is Driver Analysis? Importance and Best Practices

Was The Experience Memorable? (Part II) — Tuesday CX Thoughts

Data Discovery: What it is, Importance, Process + Use Cases
Sep 16, 2024
Other categories
- Academic Research
- Artificial Intelligence
- Assessments
- Brand Awareness
- Case Studies
- Communities
- Consumer Insights
- Customer effort score
- Customer Engagement
- Customer Experience
- Customer Loyalty
- Customer Research
- Customer Satisfaction
- Employee Benefits
- Employee Engagement
- Employee Retention
- Friday Five
- General Data Protection Regulation
- Insights Hub
- Life@QuestionPro
- Market Research
- Mobile diaries
- Mobile Surveys
- New Features
- Online Communities
- Question Types
- Questionnaire
- QuestionPro Products
- Release Notes
- Research Tools and Apps
- Revenue at Risk
- Survey Templates
- Training Tips
- Tuesday CX Thoughts (TCXT)
- Uncategorized
- What’s Coming Up
- Workforce Intelligence
Root out friction in every digital experience, super-charge conversion rates, and optimize digital self-service
Uncover insights from any interaction, deliver AI-powered agent coaching, and reduce cost to serve
Increase revenue and loyalty with real-time insights and recommendations delivered to teams on the ground
Know how your people feel and empower managers to improve employee engagement, productivity, and retention
Take action in the moments that matter most along the employee journey and drive bottom line growth
Whatever they’re saying, wherever they’re saying it, know exactly what’s going on with your people
Get faster, richer insights with qual and quant tools that make powerful market research available to everyone
Run concept tests, pricing studies, prototyping + more with fast, powerful studies designed by UX research experts
Track your brand performance 24/7 and act quickly to respond to opportunities and challenges in your market
Explore the platform powering Experience Management
- Free Account
- Product Demos
- For Digital
- For Customer Care
- For Human Resources
- For Researchers
- Financial Services
- All Industries
Popular Use Cases
- Customer Experience
- Employee Experience
- Net Promoter Score
- Voice of Customer
- Customer Success Hub
- Product Documentation
- Training & Certification
- XM Institute
- Popular Resources
- Customer Stories
- Artificial Intelligence
Market Research
- Partnerships
- Marketplace
The annual gathering of the experience leaders at the world’s iconic brands building breakthrough business results, live in Salt Lake City.
- English/AU & NZ
- Español/Europa
- Español/América Latina
- Português Brasileiro
- REQUEST DEMO
- Experience Management
- Focus Groups
Try Qualtrics for free
The definitive guide to focus groups.
15 min read Interested in focus groups but not sure where to start? Use our definitive guide to grasp the essentials and learn how you can leverage focus groups to better know your audience.
Written by : Will Webster
Fact Checked by : Karen Goldstein
What is a focus group?
Focus groups are a type of qualitative research that bring together a small group of people representing a target audience. In a conversation usually guided by a moderator, this group will discuss a specific topic, products, services or concepts in a controlled environment.
The purpose of focus groups is to have a relaxed, open-ended conversation to gain insights that may not be possible from a survey or individual interview. They’re a very valuable tool in the research toolkit.
Free eBook: 2024 global market research trends report

Focus group roles
In any focus group there are typically three main roles being played.
| 1 | They’re there to contribute to the discussion – sharing their thoughts, feelings and experiences – and provide the qualitative data focus groups exist to gather. They are typically chosen because they represent the target market or demographic being studied. | |
|---|---|---|
| 2 | The moderator’s role is to guide the conversation and focus group participants. They’re there to introduce the purpose of the focus group, lay the ground rules to the group members, and create a safe and respectful environment for discussion. The moderator should both follow a discussion framework and be prepared to adapt to the flow of conversation. Although rarely common, there can be two moderators in some types of focus groups. | |
| 3 | The observers are there to, well, observe. They are typically members of the research team or the company conducting the focus group research, who watch the focus group discussion without participating. They’re there for several reasons: to hear the discussion live, to ask the moderator to probe on certain points of interest, to collect data, to observe body language and group interaction, and to gather any additional insights. |

When should a focus group be used?
Focus groups are a very popular type of research method that’s used in virtually every sector, from tech to academia, and marketing to political science.
Focus groups are a great choice if you want to go deep into a particular topic. If surveys are a brilliant tool for understanding what someone feels about something, focus groups help us to explore why – which is why the two work great in tandem. Focus groups give us an opportunity to capture the human element – the emotions and non-verbal cues that numbers often miss – and help us to explore underlying motivations.
Here are some of the most common focus group use cases.
New product or concept testing
If you’ve got a new product or concept in the works, a focus group can provide valuable feedback before you launch it into the market. You can get a sense of how people might react to it, what they like or dislike, and any improvements they might suggest.
In fact, focus groups are often used by brands to improve on and even co-create products in real time, with concepts discussed and iterated over the course of the session.
Understanding customers better
Focus groups are a great market research tool to help you better understand why customers think and behave the way they do. If, for example, a product isn’t selling as expected, a focus group with your customers can shine light on their barriers to purchase.
Beyond current customers, businesses can also use focus groups to better understand new prospects and bring their target customer segments to life.
Marketing and advertising
Before you invest a lot of money into a marketing or advertising campaign, you could use a focus group to test your messaging and visuals. Once any tweaks are made, you should be left with a campaign that will better resonate with your target audience.
Exploratory research
Focus groups are great when you don’t know what you don’t know. If you’re entering a new market or targeting a new customer segment, they can help you explore and understand the landscape.
When quantitative data isn’t enough
Sometimes, numbers and stats don’t tell the whole story. If you have quantitative data but want to delve deeper into the ‘why’ and ‘how’, focus groups are a great way to do that.
Focus groups can provide rich, qualitative insights that quantitative research methods might miss. But it’s important to remember that they aren’t right for every situation.
If you need to make definitive conclusions about a large population, a quantitative survey will be a better option. The same applies if you’re focusing on sensitive topics that people may not feel comfortable discussing in a group setting, such as financial or health matters.
At the end of the day, the best research method for your use case really depends on your specific goals, who you’re collecting insights from and the nature of the information you’re seeking.
Types of focus groups
Focus groups can take different forms depending on the objectives of the study, the participants, and the nature of the topic being discussed. Ranging from the common to the seldom used, here are the different types of focus group methods.
One-way focus groups
The classic focus group format: a moderator leads a discussion among a group of participants about a particular topic.
Two-way focus groups
Here one group watches another , observing the discussion, interactions and conclusions. This format is used to provide additional insights and a deeper understanding of the topic.
Dual-moderator focus groups
A focus group with two moderators. One ensures the session runs along smoothly; the other makes sure all topics are covered. The aim of this format is to create a more comprehensive discussion.
Dueling-moderator focus groups
Like dual moderator focus groups in that there are two moderators, but here the moderators take opposing viewpoints on the topic. The purpose of this format is to help the participants consider and discuss a wider range of points.
Respondent-moderator focus groups
Where one respondent – or several – plays the role of moderator. This format counters the unintentional bias that can come from a single moderator, and encourages variety in the discussion,
Mini focus groups, dyads and triads
Exactly as they sound, mini focus groups involve fewer participants than usual. These smaller groups – typically made up of 4 to 5 participants – are well suited to complex topics.
There are also focus groups involving two participants and a moderator – known as dyads – and groups with three participants and a moderator, which are known as triads.
Remote focus groups
An online focus group. This format is a great way to give your research a wider geographical reach and access a greater pool of people.
How to run a focus group: Step-by-step guide
The focus groups that generate the best insights are often those that are planned best. Here’s our guide for every step of the process.
1. Research and define your goal
The first step is to identify what you want to learn from the focus group. Are you testing a new product or exploring consumer behavior? Maybe you’re seeking feedback on a marketing campaign or getting to know a new target market?
2. Choose a moderator
If planning is the key ingredient for a great focus group, a good moderator is a close second.
The moderator is the most important person in the room, and needs to be someone who can facilitate discussions, manage a group of strangers, and keep the conversation on track and be able to elicit the feedback desired..
3. Choose a location
The most important consideration here is how you create a comfortable, non-judgmental environment where participants feel safe to share their thoughts and opinions.
And you also need to answer the big question: in-person or online? In-person sessions typically enable better conversation and group chemistry, while online focus groups give you access to a much bigger, broader pool of potential participants.
4. Recruit the right participants
Next, work out who you need to participate in the focus group to reach your goal. Whatever your target audience is, you want the respondents to meet the baseline criteria – noting that the ideal size for a focus group is typically between 6 and 8 participants, and that none of your participants should know each other.
Once you’ve worked out who you want there, you need to recruit them. This is often done via ads, invitations to your CMS database or a third party. Incentives, like cash or gift cards, are typically used to encourage participation.
5. Create a discussion guide
In tandem with step four, it’s time for the moderator to develop a document that will guide the discussion. Based on your research goal or goals, this guide should include a list of focus group questions or topics you want to cover during the session, and strike a good balance between structured and flexible – so you can gather the data you need while not discouraging spontaneous conversation.
6. Conduct the focus group
The big day has arrived. With everything in place, all you need to do is make sure that every participant is given an opportunity to speak.
Don’t forget to record the focus group (with the participants’ consent) and make efforts to capture non-verbal cues from participants.
7. Debrief and iterate
Debrief after each session to understand your key findings, and if necessary, edit the discussion guide for future focus groups based on your learnings and observations so far.
8. Analyse and report on the findings
Now’s time to transcribe your recordings and analyse them for key themes and insights. The aim here is to interpret your findings in the context of your initial goal.
It’s best practice to present your key focus group results and findings in a report, alongside recommendations based on them.
How many people should be in a focus group?
The ideal size of a focus group is generally said to fall between 6 and 8 participants .Why is this the sweet spot? Because it’s small enough to ensure that everyone has a chance to speak and share their views, but large enough to provide a variety of perspectives.
That said, the goal of your research and the topic(s) you’re focusing on can change things. For instance, if the topic is particularly complex or sensitive, a smaller group may be better.
If you have a larger pool of potential focus group attendees, best practice would be to split them up and conduct multiple focus groups, instead of one focus group with too many people.
Focus groups vs in-depth interviews
Focus groups and in-depth interviews are two of the most popular forms of qualitative research . They do, however, differ in what they can bring to your research – which is why they’re often used in tandem to answer a single research question.
The benefits of focus groups over in-depth interviews
Focus groups are designed to encourage interaction between a collection of people, often revealing insights that may not surface in a one-on-one conversation. They give researchers an opportunity to observe group dynamics and how individuals influence each other and can be influenced themselves.
A big advantage of focus groups is their efficiency – in one session you can gather a broad range of insights from multiple individuals.
The benefits of in-depth interviews over focus groups
In-depth interviews are one-on-one discussions between a researcher and participant.
Whereas focus groups are by definition a group discussion, in-depth interviews provide a more personal and detailed exploration of an individual’s perspectives and experiences. Because of this, interviews are great for sensitive or personal topics, and the interviewee won’t be as influenced by others when giving their honest opinions – which is a risk with focus groups.
Another benefit of in-depth interviews is that the researcher/interviewer has greater control over the conversation, which gives you a greater chance of covering all topics thoroughly.
Advantages and disadvantages of focus groups
Like any research method, focus groups come with a variety of pros and cons that are typically associated with any type of qualitative research.
Advantages of focus groups
- They give you qualitative insights . Exploring the ‘why’ behind people’s behaviors, views and decisions
- They enable interactive discussions . Often leading to deeper insights as participants explore topics and ideas
- They give immediate findings . Observing real-time reactions means you can quickly implement them on a concept, product or campaign
- You can capture non-verbal data . Non-verbal cues and body language often give a further layer of insight into participants’ attitudes and feelings
- You have real-time flexibility . The moderator can steer the conversation to explore new points and topics if they arise
Disadvantages of focus groups
- Your sample size is small . And less likely to represent how the total population feels
- You’re at risk of conforming beliefs . Meaning that participants may change what they’re saying to match the majority opinion or the loudest voice
- They require a skilled moderator . Your findings could be a lot less valuable without one
- Data analysis can be time consuming . If you’re hosting multiple groups, transcribing and deciphering data can be labour-intensive and complex
- They can be expensive (especially if done in person) . You may need to pay for participant travel, accommodation and incentives, venue rent and even moderator fees
Related resources
Market intelligence 10 min read, marketing insights 11 min read.
Analysis & Reporting
Thematic Analysis 11 min read
Ethnographic research 11 min read, mixed methods research 17 min read, data saturation in qualitative research 8 min read, how to determine sample size 12 min read, request demo.
Ready to learn more about Qualtrics?
Qualitative study design: Focus groups
- Qualitative study design
- Phenomenology
- Grounded theory
- Ethnography
- Narrative inquiry
- Action research
- Case Studies
- Field research
- Focus groups
- Observation
- Surveys & questionnaires
- Study Designs Home
Focus Groups
Focus groups bring individuals from the study population together in a specific setting in order to discuss an issue as a group. The discussion generates research data.
Focus groups typically have these features:
- Four to ten participants meeting for up to two hours
- A facilitator or facilitators to guide discussion using open-ended questions
- An emphasis on the group talking among itself rather than to the facilitator
- Discussion is recorded and then transcribed for analysis by researchers
Researchers conduct several individual focus group meetings to produce a series. The number of focus groups in the series depends on the study’s aim, methods and resources.
Focus groups use a group setting to generate data different to that obtained in a one-to-one interview. The group context may allow for better examination of beliefs, attitudes, values, perspectives, knowledge and ideas.
Focus groups can be useful in action research methodology and other study designs which seek to empower research participants. Focus groups are also useful in multimethod studies utilising different forms of data collection.
- Quick way to collect data from several people
- Produces data unique to group setting (e.g. teasing, arguing and non-verbal behaviour) due to the interaction between participants. This is a unique feature of focus groups.
- Unlike written questionnaires, focus groups don’t rely on participant literacy to generate data
- Can encourage participation from marginalised groups
- Can facilitate discussion of stigmatised or counter-cultural topics due to feeling of mutual support among focus group participants
- Can generate more critical comments than individual interviews. This is valuable for research aimed at improving products or services.
- Can be used to validate findings from quantitative research methods by providing a deeper understanding that statistics cannot.
Limitations
- Individual perspectives that dissent from the focus group’s majority may remain hidden due to overriding behavioural or cultural norms, or a desire to be seen as conforming.
- Confidentiality of individual responses is compromised due to the existence of the group
- Only applicable when the population of interest has shared social and cultural experience or share common areas of concern.
- Group discussion does not provide enough depth for researchers to understand experiences, especially in comparison to in-depth interviews.
- Data is representative of the range of views in a population, not the prevalence of such views.
- The facilitator has a strong effect on the focus groups behaviour and can therefore influence the extent to which issues or views are explored.
- Data analysis is usually very time consuming due to the quantity produced.
Example questions
- What are the experiences, needs and wishes of mothers who received midwifery care at tertiary hospitals in Victoria, Australia?
- How useful is the patient perspective for the creation of an information information booklet for patients with liver cancer?
- What factors influence nursing students' development of end-of-life communication skills?
Example studies
Harrison, M., Ryan, T., Gardiner, C., & Jones, A. (2017). Psychological and emotional needs, assessment, and support post-stroke: a multi-perspective qualitative study . Top Stroke Rehabil, 24 (2), 119-125. doi: 10.1080/10749357.2016.1196908
Shilubane, H. N., Ruiter, R. A., Bos, A. E., Reddy, P. S., & van den Borne, B. (2014). High school students' knowledge and experience with a peer who committed or attempted suicide: a focus group study . BMC Public Health, 14 , 1081. doi: 10.1186/1471-2458-14-1081
Wiles, J. L., Leibing, A., Guberman, N., Reeve, J., & Allen, R. E. (2012). The meaning of "aging in place" to older people . Gerontologist , 52(3), 357-366. doi: 10.1093/geront/gnr098
Kitzinger, J. (1995). Qualitative research: introducing focus groups . BMJ, 311 (7000), 299. doi: 10.1136/bmj.311.7000.299
Rice, P. L., & Ezzy, D. (1999). Qualitative research methods: a health focus . South Melbourne, Australia: Oxford University Press.
- << Previous: Methods
- Next: Observation >>
- Last Updated: Jul 3, 2024 11:46 AM
- URL: https://deakin.libguides.com/qualitative-study-designs
Research Methods at SCS
- Basic Strategies
- Literature Reviews & Annotated Bibliographies
- Qualitative & Quantitative Methods
Case Studies
Focus groups.
- White Papers
- << Previous: Qualitative & Quantitative Methods
- Next: Surveys >>
- Last Updated: Jan 26, 2024 10:52 AM
- URL: https://guides.library.georgetown.edu/research
What Is a Focus Group?
Saul McLeod, PhD
Editor-in-Chief for Simply Psychology
BSc (Hons) Psychology, MRes, PhD, University of Manchester
Saul McLeod, PhD., is a qualified psychology teacher with over 18 years of experience in further and higher education. He has been published in peer-reviewed journals, including the Journal of Clinical Psychology.
Learn about our Editorial Process
Olivia Guy-Evans, MSc
Associate Editor for Simply Psychology
BSc (Hons) Psychology, MSc Psychology of Education
Olivia Guy-Evans is a writer and associate editor for Simply Psychology. She has previously worked in healthcare and educational sectors.
A focus group is a qualitative research method that involves facilitating a small group discussion with participants who share common characteristics or experiences that are relevant to the research topic. The goal is to gain insights through group conversation and observation of dynamics.

In a focus group:
- A moderator asks questions and leads a group of typically 6 to 12 pre-screened participants through a discussion focused on a particular topic.
- Group members are encouraged to talk with one another, exchange anecdotes, comment on each others’ experiences and points of view, and build on each others’ responses.
- The goal is to create a candid, natural conversation that provides insights into the participants’ perceptions, attitudes, beliefs, and opinions on the topic.
- Focus groups capitalize on group dynamics to elicit multiple perspectives in a social environment as participants are influenced by and influence others through open discussion.
- The interactive responses allow researchers to quickly gather more contextual, nuanced qualitative data compared to surveys or one-on-one interviews.
Focus groups allow researchers to gather perspectives from multiple people at once in an interactive group setting. This group dynamic surfaces richer responses as participants build on each other’s comments, discuss issues in-depth, and voice agreements or disagreements.
It is important that participants feel comfortable expressing diverse viewpoints rather than being pressured into a consensus.
Focus groups emerged as an alternative to questionnaires in the 1930s over concerns that surveys fostered passive responses or failed to capture people’s authentic perspectives.
During World War II, focus groups were used to evaluate military morale-boosting radio programs. By the 1950s focus groups became widely adopted in marketing research to test consumer preferences.
A key benefit K. Merton highlighted in 1956 was grouping participants with shared knowledge of a topic. This common grounding enables people to provide context to their experiences and allows contrasts between viewpoints to emerge across the group.
As a result, focus groups can elicit a wider range of perspectives than one-on-one interviews.
Step 1 : Clarify the Focus Group’s Purpose and Orientation
Clarify the purpose and orientation of the focus group (Tracy, 2013). Carefully consider whether a focus group or individual interviews will provide the type of qualitative data needed to address your research questions.
Determine if the interactive, fast-paced group discussion format is aligned with gathering perspectives vs. in-depth attitudes on a topic.
Consider incorporating special techniques like extended focus groups with pre-surveys, touchstones using creative imagery/metaphors to focus the topic, or bracketing through ongoing conceptual inspection.
For example
A touchstone in a focus group refers to using a shared experience, activity, metaphor, or other creative technique to provide a common reference point and orientation for grounding the discussion.
The purpose of Mulvale et al. (2021) was to understand the hospital experiences of youth after suicide attempts.
The researchers created a touchstone to focus the discussion specifically around the hospital visit. This provided a shared orientation for the vulnerable participants to open up about their emotional journeys.
In the example from Mulvale et al. (2021), the researchers designated the hospital visit following suicide attempts as the touchstone. This means:
- The visit served as a defining shared experience all youth participants could draw upon to guide the focus group discussion, since they unfortunately had this in common.
- Framing questions around recounting and making meaning out of the hospitalization focused the conversation to elicit rich details about interactions, emotions, challenges, supports needed, and more in relation to this watershed event.
- The hospital visit as a touchstone likely resonated profoundly across youth given the intensity and vulnerability surrounding their suicide attempts. This deepened their willingness to open up and established group rapport.
So in this case, the touchstone concentrated the dialogue around a common catalyst experience enabling youth to build understanding, voice difficulties, and potentially find healing through sharing their journey with empathetic peers who had endured the same trauma.
Step 2 : Select a Homogeneous Grouping Characteristic
Select a homogeneous grouping characteristic (Krueger & Casey, 2009) to recruit participants with a commonality, like shared roles, experiences, or demographics, to enable meaningful discussion.
A sample size of between 6 to 10 participants allows for adequate mingling (MacIntosh 1993).
More members may diminish the ability to capture all viewpoints. Fewer risks limited diversity of thought.
Balance recruitment across income, gender, age, and cultural factors to increase heterogeneity in perspectives. Consider screening criteria to qualify relevant participants.
Choosing focus group participants requires balancing homogeneity and diversity – too much variation across gender, class, profession, etc., can inhibit sharing, while over-similarity limits perspectives. Groups should feel mutual comfort and relevance of experience to enable open contributions while still representing a mix of viewpoints on the topic (Morgan 1988).
Mulvale et al. (2021) determined grouping by gender rather than age or ethnicity was more impactful for suicide attempt experiences.
They fostered difficult discussions by bringing together male and female youth separately based on the sensitive nature of topics like societal expectations around distress.
Step 3 : Designate a Moderator
Designate a skilled, neutral moderator (Crowe, 2003; Morgan, 1997) to steer productive dialogue given their expertise in guiding group interactions. Consider cultural insider moderators positioned to foster participant sharing by understanding community norms.
Define moderator responsibilities like directing discussion flow, monitoring air time across members, and capturing observational notes on behaviors/dynamics.
Choose whether the moderator also analyzes data or only facilitates the group.
Mulvale et al. (2021) designated a moderator experienced working with marginalized youth to encourage sharing by establishing an empathetic, non-judgmental environment through trust-building and active listening guidance.
Step 4 : Develop a Focus Group Guide
Develop an extensive focus group guide (Krueger & Casey, 2009). Include an introduction to set a relaxed tone, explain the study rationale, review confidentiality protection procedures, and facilitate a participant introduction activity.
Also include guidelines reiterating respect, listening, and sharing principles both verbally and in writing.
Group confidentiality agreement
The group context introduces distinct ethical demands around informed consent, participant expectations, confidentiality, and data treatment. Establishing guidelines at the outset helps address relevant issues.
Create a group confidentiality agreement (Berg, 2004) specifying that all comments made during the session must remain private, anonymous in data analysis, and not discussed outside the group without permission.
Have it signed, demonstrating a communal commitment to sustaining a safe, secure environment for honest sharing.
Berg (2004) recommends a formal signed agreement prohibiting participants from publicly talking about anything said in the focus group without permission. This reassures members their personal disclosures are safeguarded.
Develop questions starting general then funneling down to 10-12 key questions on critical topics. Integrate think/pair/share activities between question sets to encourage inclusion. Close with a conclusion to summarize key ideas voiced without endorsing consensus.
Krueger and Casey (2009) recommend structuring focus group questions in five stages:
Opening Questions:
- Start with easy, non-threatening questions to make participants comfortable, often related to their background and experience with the topic.
- Get everyone talking and open up initial dialogue.
- Example: “Let’s go around and have each person share how long you’ve lived in this city.”
Introductory Questions:
- Transition to the key focus group objectives and main topics of interest.
- Remain quite general to provide baseline understanding before drilling down.
- Example: “Thinking broadly, how would you describe the arts and cultural offerings in your community?”
Transition Questions:
- Serve as a logical link between introductory and key questions.
- Funnel participants toward critical topics guided by research aims.
- Example: “Specifically related to concerts and theatre performances, what venues in town have you attended events at over the past year?”
Key Questions:
- Drive at the heart of study goals, and issues under investigation.
- Ask 5-10 questions that foster organic, interactive discussion between participants.
- Example: “What enhances or detracts from the concert-going experience at these various venues?”
Ending Questions:
- Provide an opportunity for final thoughts or anything missed.
- Assess the degree of consensus on key topics.
- Example: “If you could improve just one thing about the concert and theatre options here, what would you prioritize?”
It is vital to extensively pilot test draft questions to hone the wording, flow, timing, tone and tackle any gaps to adequately cover research objectives through dynamic group discussion.
Step 5 : Prepare the focus group room
Prepare the focus group room (Krueger & Casey, 2009) attending to details like circular seating for eye contact, centralized recording equipment with backup power, name cards, and refreshments to create a welcoming, affirming environment critical for participants to feel valued, comfortable engaging in genuine dialogue as a collective.
Arrange seating comfortably in a circle to facilitate discussion flow and eye contact among members. Decide if space for breakout conversations or activities like role-playing is needed.
Refreshments
- Coordinate snacks or light refreshments to be available when focus group members arrive, especially for longer sessions. This contributes to a welcoming atmosphere.
- Even if no snacks are provided, consider making bottled water available throughout the session.
- Set out colorful pens and blank name tags for focus group members to write their preferred name or pseudonym when they arrive.
- Attaching name tags to clothing facilitates interaction and expedites learning names.
- If short on preparation time, prepare printed name tags in advance based on RSVPs, but blank name tags enable anonymity if preferred.
Krueger & Casey (2009) suggest welcoming focus group members with comfortable, inclusive seating arrangements in a circle to enable eye contact. Providing snacks and music sets a relaxed tone.
Step 6 : Conduct the focus group
Conduct the focus group utilizing moderation skills like conveying empathy, observing verbal and non-verbal cues, gently redirecting and probing overlooked members, and affirming the usefulness of knowledge sharing.
Use facilitation principles (Krueger & Casey, 2009; Tracy 2013) like ensuring psychological safety, mutual respect, equitable airtime, and eliciting an array of perspectives to expand group knowledge. Gain member buy-in through collaborative review.
Record discussions through detailed note-taking, audio/video recording, and seating charts tracking engaged participation.
The role of moderator
The moderator is critical in facilitating open, interactive discussion in the group. Their main responsibilities are:
- Providing clear explanations of the purpose and helping participants feel comfortable
- Promoting debate by asking open-ended questions
- Drawing out differences of opinion and a range of perspectives by challenging participants
- Probing for more details when needed or moving the conversation forward
- Keeping the discussion focused and on track
- Ensuring all participants get a chance to speak
- Remaining neutral and non-judgmental, without sharing personal opinions
Moderators need strong interpersonal abilities to build participant trust and comfort sharing. The degree of control and input from the moderator depends on the research goals and personal style.
With multiple moderators, roles, and responsibilities should be clear and consistent across groups. Careful preparation is key for effective moderation.
Mulvale et al. (2021) fostered psychological safety for youth to share intense emotions about suicide attempts without judgment. The moderator ensured equitable speaking opportunities within a compassionate climate.
Krueger & Casey (2009) advise moderators to handle displays of distress empathetically by offering a break and emotional support through active listening instead of ignoring reactions. This upholds ethical principles.
Advantages and disadvantages of focus groups
Focus groups efficiently provide interactive qualitative data that can yield useful insights into emerging themes. However, findings may be skewed by group behaviors and still require larger sample validation through added research methods. Careful planning is vital.
- Efficient way to gather a range of perspectives in participants’ own words in a short time
- Group dynamic encourages more complex responses as members build on others’ comments
- Can observe meaningful group interactions, consensus, or disagreements
- Flexibility for moderators to probe unanticipated insights during discussion
- Often feels more comfortable sharing as part of a group rather than one-on-one
- Helps participants recall and reflect by listening to others tell their stories
Disadvantages
- Small sample size makes findings difficult to generalize
- Groupthink: influential members may discourage dissenting views from being shared
- Social desirability bias: reluctance from participants to oppose perceived majority opinions
- Requires highly skilled moderators to foster inclusive participation and contain domineering members
- Confidentiality harder to ensure than with individual interviews
- Transcriptions may have overlapping talk that is difficult to capture accurately
- Group dynamics adds layers of complexity for analysis beyond just the content of responses
Goss, J. D., & Leinbach, T. R. (1996). Focus groups as alternative research practice: experience with transmigrants in Indonesia. Area , 115-123.
Kitzinger, J. (1994). The methodology of focus groups: the importance of interaction between research participants . Sociology of health & illness , 16 (1), 103-121.
Kitzinger J. (1995). Introducing focus groups. British Medical Journal, 311 , 299-302.
Morgan D.L. (1988). Focus groups as qualitative research . London: Sage.
Mulvale, G., Green, J., Miatello, A., Cassidy, A. E., & Martens, T. (2021). Finding harmony within dissonance: engaging patients, family/caregivers and service providers in research to fundamentally restructure relationships through integrative dynamics . Health Expectations , 24 , 147-160.
Powell, R. A., Single, H. M., & Lloyd, K. R. (1996). Focus groups in mental health research: enhancing the validity of user and provider questionnaires . International Journal of Social Psychiatry , 42 (3), 193-206.
Puchta, C., & Potter, J. (2004). Focus group practice . Sage.
Redmond, R. A., & Curtis, E. A. (2009). Focus groups: principles and process. Nurse researcher , 16 (3).
Smith, J. A., Scammon, D. L., & Beck, S. L. (1995). Using patient focus groups for new patient services. The Joint Commission Journal on Quality Improvement , 21 (1), 22-31.
Smithson, J. (2008). Focus groups. The Sage handbook of social research methods , 357-370.
White, G. E., & Thomson, A. N. (1995). Anonymized focus groups as a research tool for health professionals. Qualitative Health Research , 5 (2), 256-261.
Download PDF slides of the presentation ‘ Conducting Focus Groups – A Brief Overview ‘
Focus Groups 101

July 31, 2022 2022-07-31
- Email article
- Share on LinkedIn
- Share on Twitter
It is no secret that the field of user experience often favors objective, observational research methods over subjective, attitudinal methods. After all, when something is observed, with proof that it has actually happened, it can be hard to argue against it. However, it takes more than observational research to truly empathize and understand the full complexity of a person’s experience, which includes emotional experiences, mindsets, values, and belief systems. Since there is no other way to gather this data (at the writing of this article, mind reading with neural implants is not possible) researchers must use attitudinal methods to solicit the thoughts and opinions of target customers. A focus group is one of these methods.
In This Article:
What is a focus group, limitations and risks of focus groups, benefits of focus groups, you can run an effective focus group.
Definition: A focus group is a qualitative, attitudinal research method in which a facilitator conducts a meeting or workshop (typically about 1–2 hours long) with a group of 6–9 people to discuss issues and concerns about their experiences with a product or service. The term “focus” relates to the role of the facilitator, who maintains the group’s focus on certain topics during discussions.
Traditionally, focus groups have been a market-research method, used to get a sense of some aspect of a product, service, or concept. In these settings, the focus would typically be on certain words, graphics, videos, or other noninteractive media. All participants are presented with the media as a group and then prompted to provide their thoughts to the facilitator and the rest of the group.
Generally speaking, focus groups can provide useful information about your customers’ overall opinions and their impressions of a product or service.
Focus groups are notoriously problematic and often improperly used. Here are some of their limitations:
- They do not provide detailed insights on usability. People will comment on what is shown or remembered and offer opinions, so, by their nature, focus groups cannot provide any objective information on behavior when using a product or service. Thus, they cannot provide detailed usability insights, which would be best found with a usability test or field study . Even if there are some usability insights uncovered when presenting a design, products are almost never used by a whole committee; they’re used individually.
- People don’t always know what they will do or what will MOST benefit them in the future. In many focus groups, participants are asked whether they would use a particular product. But users do not always do what they say they will do. So, while it’s helpful to listen to customers’ concerns, preferences, or requests for features or product offerings — especially to uncover unmet user needs — the requests themselves are not always going to be the best solutions to address customers’ needs in a systematic and prioritized way.
- Negativity bias often results in people more readily recalling what was bad about an experience (particularly if it was not a great one), which can skew the discussion negatively for everyone else.
- The peak-end rule can cause people to overly focus on the most memorable and most recent moments, at the expense of other possibly more-meaningful ones.
- Priming can cause participants to overemphasize an aspect of their experience, because it so happened that someone else mentioned it and made them remember it.
- Group dynamics may impact how much (or how little) people share. Strong personalities in the group may affect what and how much is shared. Depending on the focus group’s format, it may disproportionately represent the opinions of those who are more talkative or quick to answer. Groupthink is also more likely to occur in these settings if only verbal contributions are given attention. To paraphrase my colleague Sarah Gibbons : a poorly run focus group can be a great way to pay 9 people for the opinions of three.
Given these limitations, focus groups should NOT be utilized in the following contexts:
- Evaluating a design’s usability
- Evaluating workflows
- Creating a list of design requirements
- Determining a UI’s impact on emotions
- Quantifying satisfaction or other sentiments
Despite these shortcomings, there are some good reasons to consider a focus group:
- Participants with similar goals or perspectives can build on each other’s responses or recall experiences in greater detail. Sometimes during interviews, a participant might have trouble recalling all the details of an experience. However, hearing another participant mention something related may trigger the recollection of an important detail, which would otherwise get skimmed over in an interview.
- They can help teams clarify users’ mental models and language (vocabulary) around the problem space during discovery phases , before conducting further research. While you should generally run a pilot study for most research studies anyway, a focus group can help researchers rework a research plan or facilitator guide with language that could be more user-centered.
- They are a time-efficient method for the researcher. Rather than dedicate 9–12 hours interviewing 6–9 individual participants, a researcher can dedicate 1–2 hours to gather the perspectives of 6–9 people at the same time. It can be a quick way to learn from many people and perspectives (and certainly a 100% improvement to conducting no research at all). These can be especially time-efficient if the researcher is facilitating the focus group online rather than in person.
- When run properly, they can yield rich qualitative insights due to a format similar to semistructured interviews . Unlike questionnaires — which can sometimes limit the level of detail covered — focus groups give facilitators the flexibility to explore topics in which the participants are interested. This format is especially useful if the team is still in early stages of product development and trying to discover new information about the problem space.
Given these benefits, focus groups are BEST utilized in the following contexts:
- Early discovery research to gauge customer familiarity or interest in a concept and initial impressions
- Understanding users’ mental models and expectations
- Cocreation workshops with sponsored customers
It’s fair to say that focus groups are often unfairly maligned, considering the many benefits they can yield with relatively less time commitment compared to other methods. The key to reaping these benefits and mitigating limitations is to use a combination of other research methods (like other behavioral or attitudinal methods), and having a strong research plan.
Here are the key things to consider when planning your focus group:
1. Recruit participants that are representative of your target audience(s).
Who do you want to learn about? What specific segment of users are you interested in? Even if your user is “everybody,” use personas , archetypes , or jobs-to-be-done to identify key recruiting criteria . Recruiting is a tricky balance of finding similar user motivations and goals (not demographics) while inviting a mix of backgrounds to reduce bias from other sources — such as having an overly westernized sample when studying a global offering.
2. Note potential sources of bias from the focus group’s structure.
Note who is not included, and why, for consideration during analysis and when strategizing future research. Is it a different segment that’s intentionally excluded? Lack of response? Lack of interest/trust? Bias is difficult to totally eliminate, but awareness of sources of bias can help during analysis and might inform future research. For example:
- With online focus groups, there may be potential participants who are excluded from participating (be it due to a poor internet connection, lack of a desktop device, or low literacy in certain digital tools). Thus, they may not be able join a video chat or, if they do join, they may be less likely to participate when using an unfamiliar online-meeting tool or whiteboard platform for the first time.
- With in-person focus groups, it’s fair to assume that the study will only involve participants from the immediate commutable vicinity (i.e., within the city or state), especially if travel is not funded by the study or if insufficient notice is provided for those commuting from further distances.
- Is your focus group accessible? This is relevant for both in-person and online focus groups. Can disabled participants get into the facility and participate readily? Can nonverbal participants contribute?
3. Treat your focus group like a workshop . Make participants comfortable with participating, verbally or nonverbally.
As you plan your agenda for the focus group, remember that most of your participants likely do not know each other and will be asked to speak honestly, potentially revealing information that may make them feel vulnerable or unlike others. Some people may do it, others may not. Consider having the following in your focus group:
- It gives a structured way for participants to build rapport with the facilitator and with each other.
- It builds participants’ confidence, in themselves and in the format (particularly if you’re using online-meeting tools or digital whiteboards). Note: Do not “break the ice” with highly personal or sensitive topics, which will likely cause participants to withdraw instead. (In fact, those types of answers are probably not going to come easily in a focus-group format, even with the most “warmed up” group. These types of questions are better suited to 1:1 interviews).
- Both written and verbal participation opportunities As with any other UX workshop , offer multiple methods of engagement (verbal and nonverbal) to encourage maximum participation and contribution. This ensures that less vocal or nonnative speakers feel comfortable contributing. You can also use the diverge–converge technique to maximize participation while decreasing bias potential. Note: If covering sensitive topics, offer an anonymous way to contribute (or, again, consider a different, more-private method altogether).
4. Have a (written) plan and guide.
Construct your prompts in advance to avoid leading or biasing participants. As with semistructured interviews, focus-group questions should use the funnel technique : be open-ended and broad at the beginning and progressively build detail and specificity with concepts as the conversation progresses. On a related note: remember to frame followup questions both positively and negatively to avoid leading participants, particularly when the conversation may naturally skew in one of these directions.
Focus groups don’t accurately predict future behavior. However, they can help gauge attitudes and guide future exploration, thus avoiding wasted research time. Still, they should be considered a starting point to further research, rather than a validation step. The good news? If your focus-group participants are willing, not only will you have their input to guide your further research, you may also have a group of customers willing and able to test what you create to further guide your design.
Related Courses
User research methods: from strategy to requirements to design.
Pick the best UX research method for each stage in the design process
User Interviews
Uncover in-depth, accurate insights about your users
ResearchOps: Scaling User Research
Orchestrate and optimize research to amplify its impact
Related Topics
- Research Methods Research Methods
Learn More:
Please accept marketing cookies to view the embedded video. https://www.youtube.com/watch?v=e9nZRMN49J0

Frequency ≠ Importance in Qualitative Data
Tanner Kohler · 3 min

Deductively Analyzing Qualitative Data

Analyzing Qualitative User Data in a Spreadsheet to Show Themes
Kim Flaherty · 4 min
Related Articles:
Obtaining Consent for User Research
Therese Fessenden · 8 min
Data Is More than Numbers: Why Qualitative Data Isn’t Just Opinions
Page Laubheimer · 9 min
6 Mistakes When Crafting Interview Questions
Maria Rosala · 5 min
Should You Run a Survey?
Maddie Brown · 6 min
Why 5 Participants Are Okay in a Qualitative Study, but Not in a Quantitative One
Raluca Budiu · 7 min
How Many Participants for a UX Interview?
Maria Rosala · 6 min
- - Google Chrome
Intended for healthcare professionals
- My email alerts
- BMA member login
- Username * Password * Forgot your log in details? Need to activate BMA Member Log In Log in via OpenAthens Log in via your institution

Search form
- Advanced search
- Search responses
- Search blogs
- Qualitative Research:...
Qualitative Research: Introducing focus groups
- Related content
- Peer review
- Jenny Kitzinger , research fellow a
- a Glasgow University Media Group, Department of Sociology, University of Glasgow, Glasgow G12 8LF
This paper introduces focus group methodology, gives advice on group composition, running the groups, and analysing the results. Focus groups have advantages for researchers in the field of health and medicine: they do not discriminate against people who cannot read or write and they can encourage participation from people reluctant to be interviewed on their own or who feel they have nothing to say.
This is the fifth in a series of seven articles describing non-quantitative techniques and showing their value in health research
**FIGURE OMITTED**
Rationale and uses of focus groups
Focus groups are a form of group interview that capitalises on communication between research participants in order to generate data. Although group interviews are often used simply as a quick and convenient way to collect data from several people simultaneously, focus groups explicitly use group interaction as part of the method. This means that instead of the researcher asking each person to respond to a question in turn, people are encouraged to talk to one another: asking questions, exchanging anecdotes and commenting on each other's experiences and points of view. 1 The method is particularly useful for exploring people's knowledge and experiences and can be used to examine not only what people think but how they think and why they think that way.
Focus groups were originally used within communication studies to explore the effects of films and television programmes, 2 and are a popular method for assessing health education messages and examining public understandings of illness and of health behaviours. 3 4 5 6 7 They are widely used to examine people's experiences of disease and of health services. 8 9 and are an effective technique for exploring the attitudes and needs of staff. 10 11
The idea behind the focus group method is that group processes can help people to explore and …
Log in using your username and password
BMA Member Log In
If you have a subscription to The BMJ, log in:
- Need to activate
- Log in via institution
- Log in via OpenAthens
Log in through your institution
Subscribe from £184 *.
Subscribe and get access to all BMJ articles, and much more.
* For online subscription
Access this article for 1 day for: £50 / $60/ €56 ( excludes VAT )
You can download a PDF version for your personal record.
Buy this article
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
The PMC website is updating on October 15, 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- J Patient Exp
Focus Group Discussion as a Tool to Assess Patient-Based Outcomes, Practical Tips for Conducting Focus Group Discussion for Medical Students—Learning With an Example
Balaji zacharia.
1 Department of Orthopedics, Government Medical College, Kozhikode, Kerala, India
Puneeth Katapadi Pai
2 Government Medical College, Kozhikode, Kerala, India
3 Department of Surgical Oncology, Regional Cancer Center, Trivandrum, Kerala, India
Patient-based outcomes (patient-reported outcomes) of any intervention can change according to factors like age, gender, region, culture, education, and socioeconomic status. Most of the available outcome measuring tools have a surgeon-related bias. Focus group discussion (FGD) is a simple and effective way to assess the outcome of an intervention. In FGD, people from similar backgrounds and experiences discuss a specific topic of interest. Our objective is to discuss the problems of common outcome measuring tools for patient satisfaction and to understand the method of conducting an FGD. We have set our own published article on patient-based outcomes after total knee arthroplasty (TKA) as an example for explaining the method of conducting an FGD. The planning, advantages, disadvantages, practicalities, and problems of conducting an FGD are explained. In conclusion, many of the tools used for assessing patient satisfaction is surgeon-centered. Focus group discussion is simple, cost-effective, requiring a small number of participants, and can be completed in a short period. It is an effective tool for assessing patient-based outcomes in TKA.
Introduction
The patient satisfaction assessment is very important in medical practice. It helps to improve medical care and make the patient happier ( 1 ). A patient’s expectation after a procedure is defined as the anticipation of certain events happening during or after surgery ( 2 ). Patient dissatisfaction can result either from inappropriate expectations or from a lack of proper information regarding the outcomes. The surgeon gives importance to procedural success. They are usually unaware of patient dissatisfaction. Regional, social, cultural, and economic factors have a bearing on the outcomes of any treatment ( 3 ).
Surgical outcomes refer to data regarding operation results, including information about mortality and morbidity, recovery time, operative numbers, and repeat rates ( 4 ). This is different from the surgeon’s expectations about the outcome which vary with the type of surgery, the seriousness of the condition, the age and fitness of the patient, the experience of the surgeon, and the volume of surgery done. Most of the tools used to find out the outcomes and measure the ability of the surgeon to produce statistically significant data using certain prescribed parameters ( 5 ). The surgeon judges the success of surgery based on the anatomical, radiological, and functional outcomes. The majority of the tools used for measuring the outcomes of surgery are based on the fact that the patient and the clinician have a common viewpoint about the outcome. This is not always true as the patient and the doctor have different perceptions about all domains of outcomes. This is true in subjective quality-of-life domains like emotional and social functioning ( 6 ). This may be probably due to the differing priorities of the 2 groups. This discrepancy between patient and clinician in the validation of health-related outcomes has guided the development of many validated patient-related outcome measures like Short Form 36 (SF 36), Eating disorder Quality of life (ED-QOL), Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC), Oxford Knee Score, and so on. These tools allow patients to rate their health and they are the center of outcome assessment ( 7 ).
Total knee replacement (TKR) is a common surgery done for osteoarthritis (OA) of the knee worldwide. It has a major effect on the activities of daily living. The geographical, social, cultural, economic, and many factors of a population can influence the outcomes of TKR. Expectations after the knee replacement will differ entirely among different populations ( 8 ). A successful TKR may not be a satisfactory one for the patient due to differences in factors determining the outcome measures ( Table 1 ). Many previous studies have looked into the patient-reported outcomes of TKR ( Table 2 ).
A Comparison Between the Factors Affecting the Outcomes in a Successful Total Knee Replacement and Patient Satisfaction After a Total Knee Replacement.
| Successful TKR | Patient satisfaction after TKR |
|---|---|
| Based on implant longevity | Based on patient satisfaction |
| Based on the revision rate | Depends on pain relief and functional improvement |
| The unrevised implant may not function well | The patient will be symptomatic even when the implant is proper |
| A third party interpret the outcome | The patient interpret it |
| Mainly depend on functional and radiological parameters | A variety of factors like functional status, emotional aspect, and social behavior can influence the outcomes |
| An in-person assessment is necessary | Can be assessed using electronic and social media also |
| Less costly | Some PRO methods can be costly and some privacy issues |
Abbreviation: TKR, total knee replacement.
The List of Few Previous studies to Assess Patient-Reported Outcomes After Total Knee Replacement With the Methods Used for Assessment and Their Conclusions.
| References | Method used assessment | Conclusions |
|---|---|---|
| Williams DP, Price AJ, Beard DJ, Hadfield SG, Arden NK, Murray DW, et al. The effects of age on patient-reported outcome measures in total knee replacements. The Bone Joint J. 2013;95-B:38-44. | Oxford knee score (OKS) and EuroQoL-5D (EQ-5D) | The early outcome after TKA by OKS and EQ-5D is comparable across all age groups. Patients <55 years are more likely to be dissatisfied with surgery. The OKS and EQ-5D alone might not accurately reflect the true outcome in all age-groups |
| Lange JK, Yang HY, Collins JE, Losina E, Katz JN. Association between preoperative radiographic severity of osteoarthritis and patient-reported outcomes of total knee Replacement. JB JS Open Access. 2020;5: e19.00073-e19.00073. | WOMAC and KOOS | TKA offers substantial symptomatic relief and functional improvement regardless of the radiographic severity of osteoarthritis. |
| Wylde V, Blom AW, Whitehouse SL, Taylor AH, Pattison GT, Bannister GC. Patient-reported outcomes after total hip and knee arthroplasty. J Arthroplasty. 2009;24:210-16. | OKS | TKA patients experience a significantly poorer functional outcome than THA patients 5 to 8 years postoperatively. |
| Collins NJ, Roos EM. Patient-reported outcomes for total hip and knee arthroplasty. Clin Geriatr Med. 2012;28:367-94. | The osteoarthritis-specific and arthroplasty-specific measures like HOOS, KOOS, WOMAC, Oxford Hip, and Knee Scores can more consistently be considered “good” patient-reported outcomes for THA and TKA. | |
| Bin Sheeha B, Williams A, Johnson DS, Granat M, Jones R. Patients’ experiences and satisfaction at one year following primary total knee arthroplasty: A focus-group discussion. Musculoskeletal Care. 2020;18:434-49. | FGD | Patient attitudes, expectations, preoperative education, communication with the surgeon, and rehabilitation affect postoperative outcomes. |
| Kennedy D, Wainwright A, Pereira L, Robarts S, Dickson P, Christian J, et al. A qualitative study of patient education needs for hip and knee replacement. BMC Musculoskelet Disord. 2017;18:413. | FGD | A multimodal patient education tailored to individual preferences and experiences according to age and gender is important before arthroplasty |
| Ayyar V, Burnett R, Coutts FJ, van der Linden ML, Mercer TH (2012). The influence of obesity on patient reported outcomes following total knee replacement. Arthritis, 2012, 1-6. | OKS | There is no significant difference in outcomes of TKA in obese and nonobese patients |
| Trieu J, Gould DJ, Schilling C, Spelman T, Dowsey MM, Choong PF. Patient-reported outcomes following total knee replacement in patients. J Clin Med. 2020;9:3150. | Pain and functional deterioration start during the second decade after TKA | |
| Ayers DC, Li W, Oatis C, Rosal MC, Franklin PD. Patient-reported outcomes after total knee replacement vary on the basis of preoperative coexisting disease in the lumbar spine and other nonoperatively treated joints. J Bone Joint Surg Am. 2013;95:1833-37. | WOMAC and ODI | Preoperative musculoskeletal pain in the lower extremity joints and low back is associated with poorer physical function at 6 months after total knee replacement. |
| Feng JE, Gabor JA, Anoushiravani AA, Long WJ, Vigdorchik JM, Meere PA, et al. Payer type does not impact patient-reported outcomes after primary total knee arthroplasty. Arthroplast Today. 2019;5:113-18. | KOOS and Veterans RAND 12 Health Survey | Regardless of insurance type, the surgeon can expect similar patient-reported outcomes if baseline demographics are similar |
Abbreviations: FGD, focus group discussion; HOOS, Hip disability and Osteoarthritis Outcome Score; KOOS, Knee injury and Osteoarthritis Outcome Score; ODI, Oswestry Disability Index; RAND, RAND-36 scales; TKA, total knee arthroplasty; WOMAC, Western Ontario and McMaster Universities Osteoarthritis Index.
Focus group discussion (FGD) is a qualitative research method. It can be used for evaluating the outcomes of health care interventions ( 9 ). A focused group discussion is an effective way to bring people from similar backgrounds and experiences to discuss a specific topic of interest. This group is guided by a moderator/leader. The moderator introduces the topic for discussion and helps the group to participate in a lively and natural way. The participants should stay on the topic and not wander ( 10 – 12 ).
There are many advantages to FGD. It can be used to explore the outcomes that cannot be explained statistically. Responses in FGD are spoken open-ended, relatively broad, and qualitative ( 13 ). They have more depth and variety. There can be nonverbal communication and group interactions. They can give an idea closer to what people are thinking and feeling. Focus group discussion is a good way to gather in-depth information about the community’s thoughts and opinions on a topic ( 14 , 15 ). Focus group discussion can yield a lot of information about a topic in a relatively short time. All these pieces of information may not be relevant. Observations and the opinions we get from FGD have to be mentioned in their own words. It can cause difficulties during translation ( 16 , 17 ). Thematic analysis and constant comparison techniques are used for data analysis ( 18 ).
Our objective is to discuss FGD as a tool to assess patient satisfaction. We also want to give some general guidelines for conducting FGD. This is based on our article published in the Journal of Medical Devices : Evidence and Research “Patient-based outcome analysis is important to determine the success of total knee arthroplasty: the result of a focus group discussion” ( 19 ) (We have taken permission from the publisher).
Materials and Methods
Fifty patients were selected for FGD. Among them, 42 patients participated in FGD. The remaining 8 did not participated. We included persons who had completed 2 years after primary TKR. Six FGD sessions was conducted. We included participants who were homogeneous in terms of age, status, class, occupation, and follow-up characteristics. Patients with inflammatory arthritis, secondary OA, posttraumatic arthritis, old high tibial osteotomy, and revision TKR were excluded from our study. Since we aimed to find out the patient-reported outcomes, we used a purposive sampling method. We collected the patient details from our hospital records. We selected a moderator who had no relationship with the patients. The participants were divided into 8 groups, each having 6 members. The allocation was done by simple randomization. After each FGD, we went through the discussions and created new domains and subdomains. Based on this, we prepared new questions for the next sessions. It helped us to discuss a bit deeper into the new domains ( 19 ). Proper planning is needed before the conduct of FGD ( Appendix A ).
The group’s composition and the discussion should be carefully planned to create a nonthreatening environment. All participants feel free to talk openly and give honest opinions. There is freedom for the participants to agree or disagree with each other. We have to support them to come out with their own opinions. They are free to express their thoughts and feelings, although their responses are hard or impossible to record on a scale.
The demographic data of the participants were collected. We also checked the knee society score of all the participants before FGD. The FGD sessions were started with a self-introduction session. We gave some time for the participants for getting to know each other. This helped them to alleviate their fear of open discussion. Then the moderator introduced himself and his team. The moderator explained the objective of this discussion and the procedure. Then he initiated the FGD by putting an open general question. Group members were free to talk openly. The groups took more time to respond than individuals. Some group members felt hesitant to speak openly. Participants were actively encouraged to express their own opinions and to respond to other members and questions posed by the leader. The moderator made sure that the discussions revolved around the topic. The group members could often stimulate thought for each other which might not have occurred otherwise. We stopped the sessions when no fresh domains emerged ( 20 , 21 ).
During our FGD, most of the participants were discussing the problems they had before the knee arthroplasty and about various treatment methods used by them to overcome these difficulties. They discussed about why they were reluctant to come for operative treatment, how they felt after surgery, and their satisfaction after TKR. We created new domains and subdomains after each FGD by making a transcript of the discussions in the patient’s own words and carefully analyzing them. No fresh domains or subdomains emerged after the fourth FGD.
During each FGD, the opinions of the participants in their own words were taken down by a person. We used both written and voice recordings of our FGD. The data obtained are analyzed by 2 different individuals who are not part of the FGD. This was to ensure the naturality and credibility of the findings. A thematic analysis of the findings was done. Thematic analysis is a qualitative descriptive method to identify and analyze the narrative materials to report patterns or themes. This method has the flexibility for analysis. These interpretations and observations were combined and a conclusion was made.
We had obtained institutional research committee approval for this study. The patients were informed about the study and that data from the FGD would be submitted for publication and their consent was taken.
We have taken the results from 4 FGD because the opinions plateaued thereafter. There were 24 participants between the ages of 50 to 65 years. Among the 24 participants, 15 were males and 9 females. The average knee society score was 1.18 with a standard deviation of 0.50. Five major domains were evolved after our FGD. From the major domains, many minor domains were also developed ( Table 3 ). From the FGD conducted, we found that the socioeconomic impact of OA of the knee is worse than the clinical and radiological severity of the disease. Patients with high preoperative expectations have low satisfaction levels. Surgeon–patient communication has a major impact on patient-reported outcomes. The patient satisfaction level is different from those measured using objective scoring systems. Patient satisfaction levels are high for pain relief, pain-free movements, and social independence. But they are not satisfied because of their inability to returning to their original occupation and performing activities that require knee flexion.
The Major and Minor Domains Emerged From our Focus Group Discussion to Assess Patient Satisfaction After Total Knee Replacement.
| 1. Patient complaints (a) Knee pain (b) Deformity of the knee (c) Cosmetic properties after surgery | 2. Loss of function (a) Inability to walk alone (b) Inability to climb upstairs (c) Inability to use Indian toilet (d) Inability to do prayer (kneeling) |
| 3. Socioeconomic aspect (a) Restricted to home (b) Dependent on others (c) Mental stress (d) Inability to go to work | 4. Delay in surgery. (a) Tried alternative modalities of treatment (b) High cost of surgery (c) Not aware of the results of TKR (d) Fear of failure of surgery (e) Fear of undergoing surgery |
| 5. Satisfaction level achieved (a) Relief from pain (b) Increased range of movements (c) Social independence: (1) walk alone/(2) go for work (d) Reasonable pre-operative expectations (e) Preoperative education (f) Postop rehabilitation | |
From our analysis, we found that loss of function was a major concern before surgery. The pain and deformity were the next. One patient told us, “Walking caused severe pain that I was restricted to my home. I was unable to squat in the toilet.” Some of them even converted their squat toilets to western type of toilets.
The social disabilities due to OA of the knee were far more than we thought. The majority of patients were restricted to their homes. They avoided attending family functions. The majority said they needed help from their children or others in climbing upstairs or for walking long distances. The difficulty to use squat toilets was another social issue. These issues were causing mental stress and depression in some patients. Loss of income due to inability to go to work was another problem. Some stopped going to work while others went to work but were less efficient. They had to take more leaves which led to reduced pay. Most of these patients were belonging to a low- or middle-income group. This affected their daily livelihood. There was a delay of 2 to 3 years before surgery for most of the patients. The affordability of total knee arthroplasty (TKA) was the major issue. They tried different modalities like Ayurveda, massaging, and acupuncture in-between. The majority were unaware of the results of TKR. Some were reluctant to do a TKR due to the fear of undergoing surgery.
Most of them were happy after TKR as they could walk and climb stairs independently. They had minimum pain compared to the preoperative level. Some patients thought they could go for manual work and use the squat toilet after TKR. They opined low satisfaction levels because they couldn’t do it after TKR. But some patients were aware of these problems before surgery and their satisfaction level was high. Proper preoperative education and expectations have a bearing on postoperative outcomes. We also came to know that most of the patients were not getting proper postoperative rehabilitation. They were taught about the rehabilitation protocol postoperatively but were not doing it properly. Some said that they were hesitant to flex the knee because they feared something might happen to the implant. Some blamed the doctors for not explaining these things.
There are some reasons behind selecting patients after TKR for assessing their satisfaction. The number of patients opting for TKR is increasing in our population. We are working in a government medical college in a developing country. Most of our patients for TKR hail from low socioeconomic status. Most of them are manual laborers and living in rural areas having limited road connectivity to their houses. They have to walk or climb hilly terrains. They have to work on farms or fields to earn their livelihood. They use squat toilets. After TKR, most of them want to return to their prior occupation. They can’t change their living conditions. Most patients become aware of the postoperative limitations only after TKR. Many of our patients were unhappy after TKR even when they are clinically and radiologically fine. This prompted us to find out the patient-reported outcome of our patients after TKR. We used FGD as a tool for knowing our patient’s satisfaction and opinions regarding TKR. The usually used measuring tools are surgeon-dependent and originate from developed countries.
Practical Problems in Conducting an FGD
As in any research method, finding a representative sample is very important in FGD. Make sure that all the participants are similar in their regional, cultural, educational, language, and socioeconomic status. Otherwise, there can be disparities in their opinions regarding the same issues. For example, if we are conducting an FGD about strengthening public transport and participants from rural and urban areas are included, their perceptions and opinion may vary. The city dwellers may be using their vehicles for travel they may be worried about traffic blocks or pathetic situations on the road, whereas the rural dwellers will be more worried about the number of buses and the making of new roads. In our case, all patients belonged to the same region, similar age-group, same diagnosis, and similar socioeconomic status ( 22 , 23 ).
Focus group discussion can be a powerful tool for gathering data on experiences, beliefs, attitudes, and perceptions. Asking sensitive questions is not at all a problem in the FGD. As all the participants belong to the same cohort, hence the topic of discussion becomes very simple for them ( 24 ). Usually, 1 or 2 questions for the starting of the discussion are needed. Usually, they are simple and general questions. Sometimes, new questions will be added which are emerging from the analysis of previous FGD. The questions are formed by the participants and the answers of which come from themselves. We have not come across any difficult situations where we have a problem with asking a sensitive question. We have prepared a set of questions for our FGD ( Table 4 ).
The Main Questions and the Probes Prepared for Our Focus Group Discussion.
| Main questions (open-ended questions) | Probes |
|---|---|
| What were the problems due to osteoarthritis of the knee? | Pain, deformities, loss of earning, restriction of activities of daily living |
| Have you taken any treatment for osteoarthritis of the knee? | Modern medicine, Ayurveda, Homeopathy, indigenous treatment modalities, no treatment done |
| How did you come to know about TKA? | Doctors, friends, magazines |
| What are the factors that delayed you from undergoing TKA | Economic factors, fear of surgery, apprehension regarding loss/failure to return to the occupation |
| What were your expectations about TKA? | |
| Are you satisfied after TKA? | Pain relief, functional improvement, activities of daily living, return to the occupation |
| Are you dissatisfied after TKA? | Pain relief, functional improvement, activities of daily living, return to the occupation |
| Did you aware of these limitations before TKA? Did your doctor explain it? | |
| Have you got instruction regarding postoperative rehabilitation? | |
| Did you follow the rehabilitation protocol? |
Abbreviation: TKA, total knee arthroplasty.
Recruiting participants is not a difficult task in FGD. In most cases, we can find out the participants from the cohort. We can collect the details of the participants from the outpatient clinic, from community nurses, hospital records, or from registries ( 25 ). We have obtained the details about our participants from the hospital records. We contacted them over telephones. One of our residents was given the charge of contacting the participants before each session.
Language barrier can be a problem. The participants and the moderator need to be well-versed in the language in which they are conducting FGD. Analysis of data and their interpretations also becomes difficult if they are not using the same language. We conducted the FGD in our mother tongue Malayalam. We did have some difficulty in translating certain colloquial terms into the English language during the publication of our results.
Maintaining quality and consistency during each session is very important ( 26 ). The audio or video recording of the FGD sessions helps to maintain the quality of the procedure. Quality control is the responsibility of the moderator. We had an audio recording of all our proceedings. And the moderator had full control of the whole team during the entire session.
Our Experiences
Our journey started by searching the literature for a simple but practical method for assessing patient satisfaction after TKA. After deciding to conduct FGD, we collected patients from the hospital records. They were randomly allocated to 6 groups. The date, time, and place of each session were decided. There was a delay of 10 days between each FGD. The moderator, a person for writing, and another one for recording were identified. Two senior doctors from our department were assigned for data analysis. A table with 7 chairs was arranged for the moderator and team members. All the data collected were handed over to the team leader after the end of each session. Each session lasted for about 1.5 to 3 hours. We can surely say that the success of our project is the result of teamwork not only among the persons involved in the conduct of the FGD but also among all the participants. Since there are no interventions involved in this research, there is little to worry about the safety aspect of the researcher and participants. But great care was taken to protect the identity of the participants. Our greatest difficulty was in translating the data during publication.
Assessment of patient-reported outcomes is important in any health care intervention. This helps the treating doctor to make necessary modifications in their practices which will ultimately help the community. The regional, cultural, social, and economic status of the patients have a bearing on their level of satisfaction. It is better to develop tools that can be used for various populations. From our experience, we think that FGD is a very effective tool for measuring patient-reported outcomes/satisfaction. It can be conducted with a minimum number of participants. Planning and preparations are less cumbersome. As we are ensuring the homogeneity of the participants, we can get an emic perspective about the subject. Even information about certain sensitive issues can be obtained during FGD. As there are no interventions involved, it is well accepted and cost-effective. We found that patient-based outcomes of TKR differ from the Knee Society Score. Focus group discussion is a simple and surgeon-friendly tool for measuring patient-reported outcomes after TKR.
Patient-based outcome measurements are important for the evaluation of any intervention. Focus group discussion is a simple and effective way to find out the patient-based outcomes. Focus group discussion is a simple and surgeon-friendly tool for measuring patient-reported outcomes after TKR.
Important Points to Be Noted While Planning a Focus Group Discussion
- Decide the number of groups*
- Make sure all participants are homogenous
- Assign the place, date, time of each focus group discussion (FGD)
- Inform the participants early regarding the FGD**
- Find out a moderator who is knowledgeable in the topic and knows the vernacular language
- Ask the moderator to prepare some leading questions***
- Arrange a person for writing and arrange an audiovisual team.
*Better to create small groups and 5 to 6 groups are enough. Too many participants make it difficult to control them during FGD, also the discussion can get going out of context.
**So that they can come on time.
***These questions should be based on the experiences of the moderator and also from the previously published literature about the topic.
Authors’ Note: The corresponding author Balaji Zacharia contributed to conceptualize the idea, helped in collecting data, analyzing, statistics, writing, and editing the manuscript. The coauthors helped in collecting data, analysis, statistics, writing, and editing the manuscript.
We have no conflict of interest for this manuscript and we have not accepted any financial assistance from within or outside of our institution for collecting data, writing the manuscript, and for its publications. This study was approved by the institutional ethics committee of Government Medical College, Kozhikode, Kerala, India. Written informed consent was obtained from the patients for their anonymised information to be published in this article. This article does not contain any studies with human subjects.
Declaration of Conflicting Interests: The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding: The author(s) received no financial support for the research, authorship, and/or publication of this article.


Contact Us (315) 303-2040
- Market Research Company Blog
Restaurant Focus Groups: Your Recipe for Success
by Emily Rodgers
Posted at: 10/6/2023 12:30 PM

In the ever-evolving landscape of the culinary world, understanding the preferences of your customers is incredibly important.
Enter: Restaurant focus groups.
These curated groups of diners offer a direct line into the minds (and palates) of your target audience, providing insights that can transform your eatery into a dining destination of choice.
In this blog post, our restaurant market research company explores focus groups: what they are, their value in the restaurant industry, and examples.
We'll also delve into a real-world case study, showcasing the tangible impact these groups can have on a restaurant's success.
Interested in conducting focus groups for your restaurant? Our market research company can help. Contact Drive Research today by filling out an online form or emailing [email protected] .
What is a Focus Group in a Restaurant?
Focus groups for restaurants provide in-depth consumer insights so that management teams can improve their food, services, marketing, and related outreach.
Focus groups can be conducted in person at a focus group facility or online through Zoom and other video conferencing tools.
Because dining out has many different layers to it for the consumer, in-person focus groups allow the following…
- Cultivation of easy participant discussions
- Researchers can pick up on nonverbal cues
- Simple follow-up questions
Importance of Conducting Restaurant Focus Groups
Running restaurant focus groups are all about improving the customer experience.
This is important for any business, of course. But it's especially important for restaurants since dining out and ordering food for pickup or delivery, is so consumer-centric.
In fact, our market research company recently polled over 950 consumers about their fast food consumption and preferences. Our survey results showed that speed of service is important to 42% of people when choosing where they are going to eat.
Moreover, focus groups are valuable for restaurants because they provide in-depth insights into:
- Quality of product (or food, in this case)
- Menu development
- Brand perception
- Service quality
- Areas of improvement
Of course, these are just a few benefits of focus groups for restaurants. Management teams can go into focus groups with certain objectives and work with their research team to meet them.
Overall, the value of conducting focus groups for a restaurant lies in the ability to gain deep insights into customer preferences, perceptions, and behavior, which can inform strategic decisions to enhance the customer experience and ultimately drive business success.
For more, check out our short video on the benefits of focus groups.
Examples of Restaurant Focus Groups
Let's review some examples of focus groups in the restaurant industry.
Menu Development Group
Offering invaluable advice for one of the most prominent aspects of a restaurant, this group relays what should be included (or excluded) from a menu.
What meals are appealing?
Which are less-than-pleasant?
Is pricing fair?
It's questions like these that will be answered by menu development groups.
Concept Testing Group
These groups will provide feedback about the general concept of a restaurant. With many restaurants failing due to an " undefined concept ," this group is not to be dismissed.
Common feedback themes included:
Basically, everything that sets the tone for a great dining experience can be measured by concept groups.
Cuisine Preferences Group
Everyone has a favorite cuisine they like to dine out on. This group centers around identifying preferred cuisine types.
Since there are so many restaurants focused on different cuisines, a preferences group will provide data to help a restaurant stand out.
Decor and Ambiance Group
Who doesn't like going to a restaurant with the perfect ambiance? That said, coming up with the "perfect" ambiance can be a challenge. Groups designed around this concept are especially helpful when conducting food market research.
Their feedback will allow restaurant management teams to nail details like...
Target Audience Group
Hitting the right target demographic is especially important for restaurants. With this group, participants will go over their typical habits when dining out.
This information will then be used by the restaurant team to cater to the correct audience.
Online Presence and Marketing Group
What gives a restaurant that special "edge" against competitors? Having a great social media and online presence.
This group will provide important insight into what a restaurant can do to nail these categories. By being active online, restaurants can attract new customers, thus creating a loyal base.
New Location Evaluation Group
This group is ideal for restaurant focus groups focusing on franchises. The more successful these locations become, the more consumers will demand.
But what makes the ideal location for a franchise?
Thankfully, management teams will be able to answer these questions based on data from evaluation groups.
Restaurant Focus Group Case Study
In this section, we provide an overview of a restaurant market research project completed for a national chain eatery at our focus group facility in Syracuse .
Learn more about the project overview, our qualitative recruitment process, the two focus groups, and the deliverables.
Project Background
A national restaurant chain with several restaurants in the Syracuse area was interested in hiring our restaurant market research company to host two focus groups in their area.
The objective of the restaurant market research was centered around consumers who ate at a fast-casual restaurant at least twice in the past 3 months.
Each focus group was also divided between heavy users and light or non-users:
- Heavy users: Visited the fast-casual restaurant 4+ times in the past year.
- Light or non-users: Visited the fast-casual restaurant less than 2 times in the past year.
Both focus groups were held at the Drive Research focus group facility in NY .
Recruiting Participants for the Focus Groups
The process of recruiting participants for the local restaurant transpired over two stages.
- First, Drive Research constructed targeted email lists of panel participants living in Syracuse.
- Second, our restaurant market research company created and ran paid randomized social media ads through Facebook and Instagram.
Both email and social promotion encouraged the target audience to take a recruitment screener created by Drive Research in order to pre-screen prospective focus group participants.
Those who qualified then received an additional re-screening phone call so that we could ask additional questions, verifying their online survey answers.
If selected, the focus group recruits received a confirmation email asking them to reply back “yes” if they wanted to participate in the restaurant market research.
Lastly, our focus group recruitment agency then called participants a day or two before the restaurant focus group, as well as a final reminder text the day of the sessions.
Hosting the Restaurant Focus Groups
On a Wednesday evening, the first focus group began at 5:30 p.m. with the second focus group to follow at 7:30 p.m.
Our restaurant market research company recommends holding two separate groups to answer similar questions.
That's because hosting a second focus group will act as a gut check to verify the data and findings discovered from the first group.
Additionally, Drive Research invited stakeholders from the local restaurant and the advertising agency assisting with the branding to our focus group facility in Syracuse.
Here clients were able to sit in our 14’ by 14’ viewing room to watch and listen as pictured below.

Upon leaving, the client also received a USB flash drive holding all audio and video files from the focus group sessions for further analysis and reporting.
For those unable to attend either session, stakeholders could still have an inside look into the qualitative research as the focus groups were streamed live off-site in HD.
The video stream also includes chat functionality to make the experience immersive and engaging.
Contact our Restaurant Market Research Company
Drive Research is a restaurant market research company that specializes in qualitative and quantitative studies. Whether it be surveys, focus groups, menu optimization, or ad concept testing - we can help.
Are you interested in conducting market research? Contact us.
- Message us on our website
- Email us at [email protected]
- Call us at 888-725-DATA
- Text us at 315-303-2040

Emily Rodgers
A SUNY Cortland graduate, Emily has taken her passion for social and content marketing to Drive Research as the Marketing Manager. She has earned certificates for both Google Analytics and Google AdWords.
Learn more about Emily, here .

Categories: Market Research Case Studies Focus Groups
Need help with your project? Get in touch with Drive Research.
View Our Blog
- Open access
- Published: 16 September 2024
“ You close the door , wipe your sadness and put on a smiling face ”: a qualitative study of the emotional labour of healthcare professionals providing palliative care in nursing homes in France
- Benoite Umubyeyi 1 ,
- Danièle Leboul 1 &
- Emmanuel Bagaragaza 1
BMC Health Services Research volume 24 , Article number: 1070 ( 2024 ) Cite this article
Metrics details
Palliative care provided to frail and dying older persons in nursing homes results in intense emotions for residents and their relatives as well as for healthcare professionals. In France, scant attention has been given to how nursing home professionals manage their emotions when providing palliative care. This study analysed the emotional demands of providing palliative care in the nursing home context, the emotional strategies used by healthcare professionals to navigate such demands, and how these demands affect their emotional wellbeing.
This qualitative study used a multiple case study approach. We purposively selected nine nursing homes from three geographical provinces in France with diverse ownership statuses (public, private, associative). Individual interviews and focus group discussions were held with 93 healthcare professionals from various occupational groups employed in the participating nursing homes. Data was collected from April 2021 to September 2022 and was analysed using thematic content analysis.
Data revealed that providing palliative care to dying residents within the nursing home context results in intertwined rewarding and exhausting emotional experiences for healthcare professionals. Professionals have to utilize multifaceted emotional strategies to navigate these experiences, including suppressing and modifying emotions and distancing themselves emotionally from residents to protect themselves from emotional suffering. Participants noted a lack of formal space to express emotions. Unrecognized emotional labour undermines the wellbeing of healthcare professionals in nursing homes, whereas acknowledging emotions enhances satisfaction and gives enhanced meaning to their crucial role in resident care.
Acknowledging emotional labour as an inevitable component of providing palliative care in nursing homes is critical to supporting healthcare professional wellbeing, resilience, and retention, which may ultimately improve the quality of care for dying residents. Ensuring quality care and supporting the emotional wellbeing of nursing home professionals requires an organisational culture that considers emotional expression a collective strength-building resource rather than an individual responsibility, in hopes of shaping a new culture that fully acknowledges their humanity alongside their professional skills.
Trial registration
ClinicalTrials.gov ID: NCT04708002; National registration: ID-RCB number: 2020-A01832-37, Registration date: 2020-12-03.
Peer Review reports
The steady increase in the number of older persons affected by multiple and complex health needs has led to a growing number of nursing home (NH) residents worldwide spending their final moments of life and dying within these settings [ 1 ]. In turn, this trend has generated heightened attention for the necessity of integrating palliative care within the NH, an approach that has not traditionally been an area of focus [ 2 , 3 , 4 ].
The core philosophy and values of the NH are to provide a home-like environment for residents. When residents require palliative and end-of-life care, the focus shifts from supporting quality living to facilitating quality dying [ 5 ]. Such a shift is accompanied by intense emotions for residents, their relatives, and NH professionals who have had intimate interactions with residents and built strong ties and long-lasting relationships with them during the extended caregiving process. The process becomes even more emotionally laden for professionals, as they often see themselves as holding a professional caring role while also taking on the emotional work of a family member role [ 6 ]. When confronted with providing quality living while simultaneously supporting quality dying [ 5 ], NH professionals have to perform significant emotional labour to provide quality care and preserve the professional-resident therapeutic relationship, all the while maintaining their own health and emotional wellbeing [ 7 ].
In France, as in many other countries, the provision of palliative care in NHs relies heavily on a multidisciplinary staff mainly composed of nursing assistants, personal support workers, registered nurses, and other regulated professionals, under the supervision of a medical coordinator. A medical coordinator in the French nursing home context is a physician, generally with geriatric competences, who has an overall coordination and medical advisory role for nursing home and external provider team for enhanced quality care. Moreover, as elsewhere, NHs in France suffer significant staff shortages due to professional fatigue, burnout, and professional turnover [ 8 ]. The recent COVID-19 pandemic has worsened the situation in NHs, with increased COVID-19-related deaths, augmented workloads, expanded isolation, and added psychological burden among care workers [ 9 , 10 ]. There is a pressing need for NH organisations to acknowledge the emotional labour endured by healthcare professionals during the caregiving process, particularly when it involves providing palliative and end-of-life care to residents.
Current evidence has demonstrated a strong link between burnout, job satisfaction, performance, staff retention, and attrition and the emotional labour of caring [ 11 , 12 ]. When healthcare professionals have to suppress or modify their emotions, they experience dissonance between feelings and performance, which in the long term can result in emotional distress, burnout, and intention to leave the profession [ 12 , 13 ]. Other studies have noted that when emotions are freely expressed and supported, they may have a positive impact on professional-patient interpersonal relationships, staff member wellbeing, and the quality of patient care [ 14 ]. However, most studies that have explored the emotional labour involved in providing palliative care have focused on hospital, hospice, or palliative care unit settings. Rarely have these studies been conducted in NH contexts. In fact, the physical labor associated with caring in NHs and the economic aspects of the work, such as wages and scheduling, receive more attention than does emotional labour [ 15 ]. In addition, emotional intelligence is an expected competency of healthcare professionals, particularly an individual’s ability to manage their own emotions to the point that failing to do so is viewed as an individual weakness and professional failure [ 16 ]. Yet, it has been documented that the effectiveness of emotional labour depends on various factors, including the nature of the service and the organisational culture [ 13 ]. This requires situated knowledge to better understand the emotional work performed by healthcare professionals in specific contexts, such as NHs.
Emotional labour in palliative care and in nursing homes
Emotional labour has been defined as the process through which healthcare professionals suppress or change their feelings to align with organisational rules and guidelines while still conveying to others a sense of being cared for [ 17 ]. Emotional labour involves three strategies: surface acting, deep acting, and displaying genuine emotions [ 18 ]. Surface acting entails suppressing or hiding felt emotions or faking unfelt emotions to alter outwards expression. Deep acting entails a conscious attempt to modify inner feelings and felt emotions to match expected emotions [ 18 , 19 ]. Displaying genuine emotions entails the expression of natural emotions that are congruent with felt feelings without any adjustment [ 18 ]. In this study, we conceptualize emotional labour as the efforts deployed by healthcare professionals to manage their emotions when providing palliative care to NH residents.
Nurse scholars have expanded the concept of emotional labour to nursing, emphasizing the emotional component and the demand associated with caring in nursing [ 19 ]. Nurses perform emotional labour when they have to induce or suppress their feelings to align them with what is expected by their institutions to make patients feel cared for and safe, irrespective of their own actual feelings [ 20 , 21 ]. For example, when nurses are confronted with death but feel unable to facilitate a ‘good death’, they may have complex feelings of guilt and anger but may have to suppress these feelings to continue attending to patients and their relatives [ 22 , 23 ].
Emotions are inherently linked to caring, as they are essential to the development of effective and meaningful relationships with patients, their relatives, and other professionals [ 24 ]. Studies that have explored the emotional labour associated with providing palliative care highlight the complexities of the emotionally demanding experiences healthcare professionals encounter in their practice [ 6 , 23 ]. The cumulative emotional effects of grief and sadness experienced by NH professionals attending to dying individuals require them to deploy significant effort to balance the demands of the healthcare organization, the emotional needs of others, and their own wellbeing [ 23 ].
The limited available literature on emotional labour in NHs illuminates the critical influence that the physical and social environments of NHs have on shaping care providers’ emotional experiences of caring for dying residents [ 7 ]. Caring for ill, disoriented residents with aggressive behaviours as well as dying residents in their last stages of life requires NH professionals to regulate their emotions, often masking their true feelings to prioritize the emotional needs of residents and their families above their own [ 6 , 15 ]. Additionally, ethical and moral concerns that professionals face during end-of-life-care provision, such as preserving residents’ dignity, engaging in end-of-life conversations, respecting end-of-life preferences, life-prolonging treatment or treatment withdrawal, likely play a role in emotional regulation and strategies undertaken by professionals [ 23 , 25 ]. All these may affect healthcare professionals’ capacity to interact effectively with residents and co-workers, nurture their sense of self, and provide optimal care [ 7 , 22 ]. However, it is important to note that the regulation of emotions may also produce positive effects, such as facilitating caring and forming the bonds necessary to foster a home-like NH environment [ 5 , 15 ].
Despite the crucial role that emotions play in providing care in NHs, the emotional labour undertaken by NH care professionals remains an invisible aspect of job requirements [ 15 ]. Notwithstanding the critical role that healthcare professionals play in supporting quality living and quality dying for residents in the French NH context, little is known about how they manage their emotions amidst the complex situations they encounter in their practice or how they continue to provide care without jeopardizing their own emotional wellbeing. This study aimed to help fill this gap in the research by (1) analysing the emotional dimensions of providing palliative care in the NH context as well as the strategies used by healthcare professionals to manage the emotional aspects of caring for dying residents and (2) exploring the effects of emotional labour on NH professionals’ wellbeing. To this end, this study sought to answer the following research questions: (1) How do NH professionals manage the emotional demands of caring for residents requiring palliative care? (2) What effects do emotional demands have on professional-resident interactions and the emotional wellbeing of NH professionals? This study’s findings will inform NH management on strategies and interventions to not only reduce the emotional exhaustion and burnout of healthcare professionals but also improve their resilience and wellbeing at work, ensuring that they are best equipped to provide optimal care to residents and their relatives.
Study overview and design
The findings presented in this manuscript originate from a broader implementation study that evaluated the effectiveness of a timely and integrated palliative care approach in 21 NH facilities in France. The initial study used a mixed-method [ 26 ] approach and was segmented into three phases: pre-implementation, implementation, and post-implementation. The current manuscript reports materials from the pre-implementation phase. A detailed methodological description of the broader study has been reported elsewhere [ 27 ]. The qualitative component of the study follows a multiple case study approach [ 28 ]. Among the aims of the qualitative study were to explore NH professionals’ experiences and quality of life at work and to understand how they navigate the emotional demands associated with providing palliative care to residents.
Participants and settings
This manuscript presents qualitative findings from nine out of the 21 NHs that participated in the broader study. The nine NHs were purposively selected to ensure a balanced sample of three NHs per geographical region (Iles de France, Nouvelle Aquitaine, Provence-Alpes-Côte d’Azur) as well as diversity in terms of ownership status (public, private, and private non-profit).
For this study, we purposively included healthcare professionals from various occupational groups employed on a fixed contract in the selected NHs. Participants had to have a minimum of five months of experience and had experience providing palliative care to residents in the same NH. Casual and non-fixed contractual professionals were excluded from the study.
Data collection
A combination of focus group discussions and individual in-depth interviews was used to collect data. This was to achieve an enhanced understanding of the phenomenon of emotional labour within a NH context by exploring views at individual and social contexts [ 29 ]. Nine focus group discussions were conducted with various healthcare professionals who provide direct care to residents. Each focus group was composed of seven to eleven professionals. Given the purpose of the study which was to explore how different professionals navigate the emotional demands of providing palliative care within a NH context, group composition brought together all professionals involved at varying degrees in providing such a type of care. However, to allow participants to share their experiences freely and to avoid any status distinction or hierarchical influence [ 30 ], professionals in the managerial roles were not included in the focus groups. They were involved in individual interviews.
Prior to data collection, a meeting was organized at each participating NH to introduce the broader interventional study to professionals and invite them to take part in the study. The focus group sessions were held at a predetermined location within the NH at a time convenient to the participants and facility and lasted between 90 and 120 min. Individual in-depth interviews were conducted with the supervisory teams, namely the nurse coordinators and medical coordinators. Each individual interview lasted approximately 45 min and was held at a time and place convenient to participants. We used the interview guide developed by the researchers for the purpose of this study (supplementary material 1). The same interview guide was used for individual and focus group discussions, with slights changes on the phrasing of questions for interviews with the management team. Focus group and individual interview questions inquired about experiences of providing palliative and end-of-life care to residents, the emotional dimensions associated with such a type of care, how professionals navigate those experiences and the perceived consequences on professional wellbeing. Examples of questions included the following: How would you describe your experience of caring for dying residents in NHs? What are the emotional aspects of providing palliative care to residents, and how do you navigate those experiences? The last author conducted most of the individual interviews and some focus group discussions, while a trained research assistant under the supervision of the last author moderated the remaining focus groups. Both hold PhD degrees and have experience in conducting qualitative interviews for health research. All interviews and focus group discussions were conducted from April 2021 to September 2022. The interviews were audio-recorded after the participants granted permission. Regular field notes were written immediately after interviews and focus groups. Data collection continued until we have gained adequate and in-depth understanding [ 31 ] of emotional experiences of providing palliative care in NH.
Data analysis
Thematic content analysis following the analytical approach of Paillé and Mucchielli [ 32 ] guided the analysis. The level of analysis was a NH, with each NH considered a case. After verbatim transcription of all the data from the nine cases, two authors (BU & DL) became acquainted with the data by rereading the transcribed interviews, examining participants’ narratives from each case separately, and then developed a list of codes. From the code list, they created a thematization journal using code subdivision, integration, and hieararchization [ 32 ]. Next, the same two authors grouped related codes from all the cases, with a third team member (BE) resolving any discrepancies between the previous analysts. At the end of this stage, a thematic tree of three themes and eight subthemes was constructed. NVivo 14 software assisted with data management and facilitated the coding process.
To ensure methodological rigor, the authors used the recommended strategies for trustworthiness of qualitative data [ 33 ]. To ensure the reliability of the findings, two analysts completed the coding of transcripts, organized peer debriefing meetings throughout the analysis, and kept a reflexive journal recording all the steps taken and decisions made. A third analyst resolved any disagreements through consensus. To ensure credibility of findings, the authors triangulated methods (individual in-depth interviews and focus groups) and collected participant perspectives from various healthcare professions (nurses, nurse assistants, personal support workers, psychologists, occupational therapists, physiotherapists, medical doctors). The writing of the manuscript followed the “consolidated criteria for reporting qualitative research (COREQ)” [ 34 ] (Supplementary material 2).
Ethical considerations
The French Committee of Protection of Person (CPP) granted ethical approval for this study (Approval number: 2020.09.06 bis_20.07.31.64318). All focus groups and interviews respected the rights of participants to choose to participate in the study through informed consent. To ensure confidentiality and anonymity of the collected data, the reporting used codes instead of names.
Demographic characteristics of participants
All NH professionals who met the inclusion criteria and who were available on the day of the focus group were included in the study. In total, 93 professionals participated, including 79 participants in nine focus groups and 14 participants in individual interviews. Tables 1 and 2 provide the detailed characteristics of the settings and demographic characteristics of participants.
Quotes from individual interviews are followed by an acronym designating the profession of the participant (for example NC for Nurse Coordinator, MedCo for Medical Coordinator) as well as the code number of the NH. Quotes from focus groups are designated by the acronym FG, followed by an acronym for the location of the NH (IDF for Ile de France, NA for Nouvelle Aquitaine, PACA for Provence-Alpes-Côte d’Azur), and the code number of the NH.
Analysis of participants’ narratives revealed three overarching themes related to the emotional dimensions of providing palliative care in NHs: (1) intertwined emotionally rewarding and challenging experiences; (2) multifaceted emotional strategies; and (3) switching between emotional engagement, detachment and exhaustion. Supplementary material 3 illustrates the generation of themes and subthemes with illustrative quotes.
Theme 1. Intertwined emotionally rewarding and challenging experiences
Participants’ narratives revealed two intertwined and simultaneous emotional dimensions of providing palliative care to dying residents in NHs: (1) emotionally rewarding experiences and (2) emotionally challenging experiences. The emotionally rewarding dimension of the experiences was supported by the individual professionals’ intrinsic commitment, devotion, and engagement with older persons under their care and a professional duty to provide them with the “best possible care” they deserve. On the other hand, the NH context as a place of living and of care, with its organisational constraints, rendered the experience of providing palliative care to residents emotionally challenging. Specifically, it hindered the care providers’ ability to facilitate what they perceived to be a “dignified death,” leaving them with feelings of distress, frustration, guilt, and uselessness.
Caring for dying residents: emotionally rewarding experiences
Numerous participants described working in NH as a deliberate professional choice and vocation, stemming from their sense of commitment and engagement to offer dependant older people the care they deserve. The relational dimension associated with caring for NH residents gives meaning to their work and becomes a source of pleasure, satisfaction, and self-worth, as illustrated by the following registered nurse:
“Helping older persons is my passion. I find that there is less invasive care in NHs , and there is a relationship that develops and that I enjoy” (NC , NA , 751).
For the majority of healthcare professionals, this deliberate choice to work in NHs implies that confronting death on an ongoing basis is a professional responsibility. Despite the emotional challenges that come with multiple exposures to death, the participants affirmed their commitment to confront death as part of caring for residents. They held the belief that dying is part of living and that accompanying death is a normal process that comes with caring for the living. The devotion to accompanying residents until the end was perceived by NH professionals as a rewarding experience when they felt they had fulfilled their responsibility of facilitating a dignified death:
“It feels so rewarding to see a resident dying the way they should: with dignity , respect , free of pain and with the best possible comfort. That is what we are here for” (FG , PACA , 935).
Although death is considered an expected life trajectory in NHs, participants recognized that dying older persons are often overlooked as a category of the population requiring adequate palliative care. Their perceived duty to accompany residents until the end demonstrates their commitment to ensuring that dying residents experience comfort and dignity equal to that experienced by individuals dying in settings outside the NH.
Similarly, for some residents, NH professionals are the sole individuals they can bond with at a human level and who can meet their diverse emotional needs. Participants believed their role goes beyond that of care providers. Their drive to go above and beyond and make a difference in the end-of-life trajectory of residents becomes a rewarding experience that provides a sense of pride and self-worth. The NH professionals expressed feeling honoured to be the ones to accompany residents in that ultimate moment, even if it means forgetting themselves:
“Aging comes with many losses and emotional needs: most of them do not want to be here [in the NH]; they feel abandoned by their families , they lose their autonomy over things they used to do , they need to feel cared for. Being there for them through the most important moments of their stay here is very rewarding to us. Basically , in the first place , if they are put here , it is so they do not die alone” (FG , PACA , 931). “It’s truly a phase full of emotions where everything comes out: their past traumas , their anxiety , their worries. We try to hold it together , to forget ourselves a little so we can give them what they deserve…” (FG , NA , 755).
Participants’ accounts bring to the forefront that despite the emotionally laden experience of providing palliative care in an NH context, their commitment and determination to accompany residents in their last living moments make this experience emotionally rewarding.
A living and dying space: emotionally challenging experience
Narratives from healthcare professionals emphasized the context of the NH as being initially designed to serve as a living space. Such a home-like living environment that progressively becomes a place of care and ultimately a place of dying leads to the development of close bonds between NH professionals and residents for an extended period. The emotional and physical closeness formed with residents during their stay transcends the caregiver-resident therapeutic relationship. Healthcare professionals have to navigate these different aspects of the NH and remain professional caregivers, all the while providing a home-like environment. One participant explained:
“I’m here from 8am to 8 pm; we live with them [residents]. I do not call some of them by their names anymore. I call them grandpa , grandma. By living with and caring for them for an extended period , they end up becoming like family. When they die , it breaks our hearts” (FG , PACA , 931).
Boundary-setting issues such as these make the relational dimension of care especially difficult, as NH professionals can become too close to residents, which naturally complicates the transition to end-of-life care. Accompanying death for older persons who they have accompanied for living represented a challenging transition for participants who considered residents like their own relatives, as expressed by the following medical coordinator:
“They’re not just people we care for; we live with them. These are the people for whom we’ve fought for every minute to make life worth living. Professionals look after them almost as if they were their parents. Accompanying someone who is going to die , while you have accompanied them so they can live , is in itself emotionally hard” (MedCo , IDF , 116).
Their strong emotional bond with residents became a challenge for NH professionals when discussing the residents’ end-of-life preferences and the palliative decisions that needed to be made in preparation for the end-of-life care plan. Many shared avoiding these discussions, even when residents prompted them, as they did not feel ready to engage in such emotionally charged conversations.
“Palliative care supposes that we should help them think about their death , but we are unable to do that. We are primarily a place of life , and at the end , there is always death. That’s the complexity of [providing] palliative care in NHs” (NC , NA , 753).
The experience of providing palliative care in NHs was also challenged by structural and organisational constraints such as heavy workloads, a lack of time, and unmanaged pain. As a result, some participants reported that they were unable to provide dying residents with the required relief, which caused NH professionals lingering regret even after the death of the resident.
“That resident who died last week , I would have wished to have been able to stay with them a little longer , hold their hand , put on some music , so that there is a presence , like putting life into the end of life. Unfortunately , I was not able to free myself. And it is difficult to live with such a feeling” (FG , IDF , 116).
Theme 2. Multifaceted emotional strategies
When asked how they cope with the emotional demands of providing palliative care to residents, participants highlighted a diversity of emotional strategies they deployed to protect themselves and to continue fulfilling their caring roles. These ranged from genuinely expressing their emotions to modifying and suppressing their emotions to fit the moment. Modification and suppression of emotions were cited as the most commonly used strategies as opposed to the authentic expression of emotions.
“We shed tears”, “We’ve laughed with” : genuine display of emotions
Participants used expressions such as “We cry with” , “We’ve shed tears” , “We’ve laughed with” to convey the authentic emotional strategies put in place. They genuinely expressed their emotions in situations when they felt a deep connection with residents. Most of these genuine emotional strategies occurred in the moments approaching death or following death.
“All the residents on the floor are like my family. Last time I went to see Mrs. B , when my colleague told me she was dead , I was shocked , truly shocked. It was quick. I cried all my tears. I was so sad. I was unable to continue work because I was crying” (FG , IDF , 111).
In some situations, the NH professional’s personal history prompted the authentic expression of feelings. For example, if a resident’s death mirrored the death of their own loved ones, it made it difficult for them to conceal their true feelings as they usually do. Some referred to it as not being able to pretend to have no feelings.
“I accompanied my dying father in palliative care. Every time there is a death of a resident , it echoes my father’s. We had a resident death not long ago. When I saw him , I completely broke down. I cannot pretend anymore” (FG , IDF , 117).
The authenticity of emotions also manifested through allowing oneself time to grieve the death of a resident. A participant discussed requesting a day off to grieve, but some NHs also provided space for grieving the deceased residents.
“I was truly attached to Mr G. When he died , I took a day off. Everyone else [colleagues] continued living their life… laughing. For me , I could not come to work because I was grieving his death” (FG , IDF , 116).
Other participants also recognized a need for the authentic expression of emotions and requested emotional management support for the team.
“For a resident we’d known for a long time to whom we were very attached , we felt helpless with her end-of-life care , and so we genuinely asked for help. We held a round table… , and we asked for help from an external person” (FG , NA , 751).
While some participants expressed their genuine feelings, many participants across focus groups were in favour of emotions being unnoticed and noted a lack of formalized organisational strategies to deal with emotions. Many NH professionals admitted to frequently modifying their feelings to display emotions that are “acceptable.”
“ You wipe your sadness and put a smile on your face ”: modification of displayed emotions
Some NH professionals described their emotional work as involving frequent switching between sadness and joy to respond to the needs of the moment. Many shared trying to display emotions that were not what they truly felt because the situation at hand required them to convey different, often contradictory emotions; for the participants, this constituted difficult emotional labour.
“On one hand , you’ve got one person who is dying and next to them residents who are living. It is very difficult because you have to go into the room [and] take care of someone who is dying. You are sad because you know you will not see that person again. Nevertheless , the moment you see this person for a few minutes , you have to close the door , wipe your sadness , and put a smile on your face to accompany the next-door resident with a serene face. It is difficult to manage all these emotions at the same time. In one day , you have to give contradictory feelings. You are sad for one person , but at the same time , you have to bring joy to the other resident. You have to show them a different face , and that is not easy” (FG , IDF , 117).
The modification of emotions was compounded in the NH environment for some participants who not only adopted an expression in accordance with what was expected but also tried to set limits and find the appropriate time and space for revealing their true feelings when out of the NH. Participants described this ability to emotionally detach as protective:
“The moment I remove my uniform , I immediately put a different face…. When I reach home , if I have situations that have been painful , I allow myself to be restless and sad; I vent my true feelings…” (FG , PACA , 933).
“ You become numb and move on ”: suppression of feelings
Participants discussed the organisational expectation to suppress emotions in order to continue providing effective care. In a quest to fit into institutional norms, many NH professionals who describe themselves as normally prone to showing their emotions had to learn to suppress them.
“By nature , I am a very sensitive person , but now I keep all my emotions inside of me , and at the end , it becomes difficult to unload. Here , it is not common to open up and show emotions or talk about them. We are expected to keep it to ourselves and move on” (FG , PACA , 933).
Multiple exposures to death and a lack of time and a safe space to grieve deceased residents forced NH professionals to suppress their feelings in an attempt to cope with the distress and to continue providing care to residents.
“How can you display feelings when you have four successive deaths? You become numb and move on. Tomorrow you will have another one. You pretend as if everything is fine but there is a problem…” (FG , IDF , 117).
Theme 3. Switching between emotional engagement, detachment and exhaustion
Participants reported that the emotional labour of providing palliative care in NHs results in both negative and positive consequences. The majority of NH professionals noted that the negative consequences of emotional labour resulted in an inability to provide effective care, and the lack of supportive space to express their feelings caused emotional distress, feelings of guilt, and a sense of failure and powerlessness. Some participants accepted emotions as essential to their caring role and mentioned that they give meaning to their work.
“ Everyone was satisfied ”: enhanced satisfaction and meaning of work
Only a few NHs involved in the study had formalized procedures in place to support the emotional wellbeing of their healthcare professionals. These procedures included formal debriefs, a consultation with a psychologist, and massage therapy. In the majority of the NHs, informal peer-to-peer support was mentioned. In settings where emotions are acknowledged and supported, both professionals and managers reported increased satisfaction when accompanying dying residents.
“We had a resident to whom the team was so emotionally involved. When the end was approaching , emotions were high for both professionals and the resident. We [the supervisory team] requested the intervention of the external palliative care team to introduce a third party in the relationship and gently distance the team without completely disengaging them. At the end , everyone was satisfied , and the resident was properly accompanied. It ended up being one of the memorable end-of-life care for the staff” (NC , NA , 751).
When participants believed that they gave their best up to the end and that the outcome was a peaceful death, they gained a sense of pride and accomplishment. They felt they had attained their mission, which, for many, was one of the reasons they remained working in the NH despite the stressful environment.
“On his passing , the resident was so peaceful , so were relatives. It was a real sense of satisfaction. It is the kind of end-of-life care where you feel you have done the right care and that gives you motivation to stay” (FG , NA , 753).
“ It is heart-breaking ”: a sense of guilt and powerlessness
Suppression or modification of emotions affected the wellbeing of participants as well as the care they provided to residents. Different constraints such as time pressure and competing tasks added to their frustration. Their emotional distress manifested itself as constant feelings of guilt, powerlessness, and a sense of failure for not providing adequate care to residents. One of the most common sources of guilty feelings was when the NH professionals believed that they were unable to offer a peaceful, quality presence during end-of-life moments and that the resident died alone. Dying alone was considered inhumane by participants, as they believed that residents were placed in NHs mainly to ensure they do not die alone.
“Very often you tell yourself , ‘Well , I could have been by her side , tell her a comforting word , play the music she loved , rub her forehands , make sure she had a presence… , but no , she is gone and all alone’. It is not human at all , and you carry this with you for long” (FG , PACA , 933).
Participants also expressed feeling powerless when they saw residents in pain and discomfort, and their inability to provide the required comfort to the dying residents left them with an immense sense of failure and uselessness, which negatively affected their wellbeing and their satisfaction with the work done.
“It breaks your heart to see people suffering like this and little is done about it. It’s heart-breaking to think , ‘We are here to help them , but in fact we’re not even doing that’. We are useless” (FG , NA , 755).
“ You finally give up ”: distancing and exhaustion
To protect themselves from the distress associated with multiple exposures to death and a lack of institutional support, some participants admitted that they banalized death to emotionally distance themselves from dying residents, a strategy that the NH professionals recognized as inadequate.
“We give , we give , one day we can’t take it anymore and we banalize death. We don’t see death anymore. It does not affect us any longer , it becomes a commonplace gesture , mundane. Someone dies today; you attend to the next person who will be gone tomorrow , and so forth and so on. You keep accumulating and one day you explode” (FG , IDF , 117).
Other NH professionals adopted a superficial attitude in an attempt to distance themselves and detach themselves from their true feelings. They chose to involve themselves less in the therapeutic relationship by concentrating more on carrying out instrumental and technical care and less on offering a caring and relational presence.
“I go in [the room] , I give the injection and I get out. Not because I do not want to stay , but because I am thinking of the others. I cannot stay with the one who is dying while I have 70 others who are still alive. I have to look after those who are not dying” (NC , PACA , 935).
Some participants dealt with emotionally challenging situations by refusing to accept the palliative care plan of residents with whom they had strong ties. They would ignore the team’s decisions when it involved withdrawing feeding and restricting movement and instead provide the usual care such as taking blood pressure, providing hydration, and mobilizing residents, irrespective of the futile outcome or the risk of causing more suffering. In this way, they felt more useful towards the residents.
“We had a staff meeting , and they said Mrs X was in end-of-life care…that we should avoid mobilizing her and emphasize comfort care. When I arrived in the room , I did not do anything they said. Rather , I got her up from bed , I washed her , I dressed her , I brought the wheelchair , and I was about to take her out. When the nurse coordinator arrived , she could not understand what I was doing. I was in denial. I could not believe she was dying” (FG , IDF , 116).
Several participants reported feeling emotionally strained, exhausted, and lacking the energy to accomplish their mission. Some of them even resigned or verbalized their intentions to resign from their posts. Their emotional exhaustion reportedly stemmed from an accumulation of frustration, discouragement and a lack of accomplishment, feeling incompetent, and a lack of support, which prompted them to resign rather than form a negative view of the residents and fail to deliver effective care.
“You fight , you try your best to keep going , you get discouraged and finally you give up. That is why I want to do something else. Eventually , I want to take care of people and give them what they deserve. Here , I do not give them what they deserve , which frustrates me , and I accumulate. I resigned. I would rather leave the job to someone who wants to do it the way it is done. As for me , I am going to hold onto something else. I do not want to become a bitter caregiver….” (FG , PACA , 933).
The findings from this study illustrate that providing palliative care to dying residents within the NH context exposes healthcare professionals to intertwined rewarding and exhausting emotional experiences. This emotionally demanding work results in a constant switching between feelings of pride and accomplishment on the one hand and guilt, distress, and grief on the other, and it prompts healthcare professionals to identify and distance themselves from the residents to protect themselves from emotional suffering. These findings lead to greater insights into how NH professionals navigate these emotionally laden situations to meet the needs of the residents and the NH as well as their own needs. Drawing from these important findings, our discussion focuses on three key insights from the study: (1) Caring for dying residents results in both emotionally rewarding and emotionally exhausting experiences, (2) NH professionals have to perform emotional labour to navigate the experiences associated with providing palliative care, and (3) Unrecognized emotional labour undermines the wellbeing of NH professionals.
Caring for dying residents results in both emotionally rewarding and emotionally exhausting experiences
Genuine interest in caring for frail older persons is at the heart of the engagement and commitment demonstrated by the participants in our study. Participants described becoming emotionally attached to residents they care for as “unavoidable and the right thing to do,” especially given the expected “home-like” environment of the NH. In that sense, the affective dimension of working in NH and the internal motivation of the healthcare professionals aligned and helped them navigate the emotional labour of caring for dying residents and added meaning to their work. In line with other studies, the unique characteristics of NH, where care providers and residents engage repeatedly in deep personal and intimate exchanges for an extended time, forged closer and more trusting reciprocal relationships than are typically found within acute care setting nurse-patient interactions [ 35 , 36 ].
A majority of participants recalled the emotionally rewarding experiences associated with caring for frail and dying residents. The NH professionals described accompanying residents as their professional duty and took pride in making their last days as dignified, comfortable, home-like, and respectful as possible. Moreover, accompanying residents in their final moments was considered a moral responsibility by participants. The positive experiences and feelings stemming from close and trusting relationships with residents have been recognized by previous studies as central to the emotional wellbeing of NH professionals [ 15 ]. Direct caregivers for dying residents characterize those particular moments as the rare moments they feel appreciated, noticed, and like they are making a difference in settings where they generally feel unseen [ 36 ]. In particular, our participants expressed positive emotions such as engagement, pride, accomplishment, and self-worth in situations where they felt they had achieved dignity in caring for the dying residents. This is relevant because dignity represents an essential part of caring in NHs and in palliative care [ 37 , 38 ]. These personal characteristics and intrinsic motives constitute the internal resources and resilience attributes that allow healthcare professionals to cope with distressing situations surrounding accompanying death in NHs [ 10 ]. Future interventions and training should aim to reinforce the internal resources of NH professionals with a strong focus on building resilience.
Although participants perceived caring for dying residents as a rewarding experience, when the challenging working conditions within NH hindered them from achieving their moral and professional responsibility, it turned the experience into difficult emotional labour. The current NH working environment fails to provide necessary organisational resources and subsequently creates discrepancies between the ideals held by NH professionals on what constitutes the right comfort care to provide and the current practices. Under severe labour shortages, NHs prioritize technical and task-oriented activities over relational moments [ 39 ]. However, for participants in this study, not being present to hold the hands of the dying resident left them feeling guilty of failing their moral responsibility and their professional duty. Consistent with previous studies, the NH culture was found to prioritize tasks and expect healthcare professionals to be consistently “doing something” for residents versus “being” with residents [ 13 , 40 ]. This dissonance creates the most difficult emotional challenges, moral concerns, and distress for NH professionals [ 25 ]. That perceived inability to facilitate a “good death” due to organisational constraints results in moral distress for NH professionals and complicates their grieving process [ 23 , 41 ]. Echoing this, participants in our study shared how emotionally burdensome it was to constantly feel guilty of devoting less time to the “dying resident” because they were required to attend to the “living residents” instead. NH managers and policymakers should take measures to build a culture that enables healthcare professionals to prioritize the emotional needs of residents alongside their physical care needs, as both are equally important to end-of-life care.
Professionals have to perform emotional labour to navigate the experiences associated with providing palliative care
Participants in the current study used different emotional labour strategies to navigate the rewarding and challenging aspects of caring for dying residents in the NH context. Some adopted distancing strategies, such as focusing on task-based care and mechanical actions as well as avoiding feelings and emotional involvement, while others trivialized death or denied the impending death of residents. This process of strategy switching between engagement and detachment is prevalent among palliative care professionals as a way of coping with emotional demands and preventing grief [ 13 , 23 ].
Numerous participants reported that they tended to modify their feelings by displaying emotions that were different from those they felt. For example, some noted “wiping [their] face and showing a smiley face,” while others suppressed their feelings to “become numb and move on” in an attempt to display composure in the moment and comply with institutional rules. Attempting to modify one’s felt emotions to match displayed emotions is known as deep acting, whereas displaying fake, unfelt emotions and suppressing one’s felt emotions indicates a surface acting strategy [ 18 ]. The emotional strategies used by the participants in our study are similar to those commonly used by healthcare professionals in different care contexts [ 12 ]. Particularly in the NH context, emotional labour is intensified by the long-term therapeutic relationship, as the longer the therapeutic relationship the more complicated the emotional labour [ 7 , 15 ]. Participants in our study shared that the stronger and the closer the bond with the resident, the harder it was to navigate the emotional labour associated with witnessing their suffering and providing them with end-of-life care. Debates persist on the appropriate emotional distance to take when accompanying a resident with whom the healthcare professional has formed a close bond. It is noteworthy, however, that healthcare professionals who try to convey caring while remaining emotionally detached may experience increased emotional dissonance and potentially negative effects [ 23 ]. This phenomenon resonates particularly within the NH care context, where professional boundaries are blurred and difficult to respect [ 6 ].
Some participants in this study identified the importance of safe spaces where they can freely express their emotions without faking and without feeling judged, such as spending time informally with colleagues during breaks or with relatives at home. Researchers classify this as the backstage area of emotional expression, owing to the lack of formal recognition and poor appreciation of emotional labour in practice [ 42 , 43 ]. Given the complexity of emotional labour associated with providing palliative and end-of-life care in NHs, scholars recommend more strengthened, explicit, and structured backstage areas to recognize the emotional needs of healthcare professionals and support their emotional growth and resilience [ 43 ]. Unfortunately, findings from our study reiterate the inadequate support available in the NH context for their mental and emotional wellbeing.
In a few instances, some participants in our study allowed themselves to express naturally felt emotions. The close bond they had formed with residents prompted those who adopted the genuine manifestation of feelings to view the resident’s death as a parallel of their own loved one’s death; hence, they allowed themselves to react accordingly. Some took a leave of absence to process the grief, while others requested formal support as they struggled to come to terms with the death of the resident. Studies have shown that adopting naturally felt emotions as an emotional labour strategy can protect healthcare professionals from burnout, as it allows for authenticity and empathy expressions in care [ 12 ]. Genuine emotions have also been found to support nurses in the provision of compassionate care and to inspire cooperation from less-cooperative residents [ 6 ]. In our study, however, the absence of a formal supportive space within the NH to vent emotions discouraged the genuine expression of feelings. Even in the few NHs where opportunities for emotional sharing existed through support groups and psychologist interventions, the participants were reluctant to take advantage of these opportunities. One possible explanation could be that openly expressing emotions might be seen as a sign of weakness, incompetency, and inability to respect professional boundaries. Yet, organisational studies have shown that when grief and emotional suffering are acknowledged and collectively shared as a team, emotional distress is no longer perceived as an individual weakness but rather a collective suffering that requires collective measures to address. However, this cultural shift is only possible when it is supported by the institution through the provision of time, space, and opportunity to debrief and grieve [ 44 ].
Unrecognized emotional labour undermines the wellbeing of nursing home professionals
This study revealed that the emotions experienced by professionals receive relatively little attention within the NH context. This finding supports other studies that have highlighted the invisible nature of the emotional labour endured by healthcare professionals in end-of-life and palliative care within NHs [ 7 , 15 ]. Current institutional rules reinforced by professional norms such as the self-imposed emotional strategies used by healthcare professionals implicitly discourage the open expression of emotions and position genuine displays of emotion as incompetence [ 6 ]. Considering the expression of emotions as weak and a sign of a problem to be addressed leads to emotional labour being unrecognized, professionally undervalued, and even discriminated against [ 24 ]. This is deeply problematic, as unrecognized emotional labour can lead to personal, professional, and organisational negative outcomes.
The effect of emotional labour on a healthcare professional varies depending on the frequency, intensity, diversity, and length of the needed emotional displays as well as the degree of emotional dissonance between the emotions experienced and those anticipated [ 14 ]. Evidence demonstrates that a constant mismatch between felt feelings and displayed emotions leads to emotional dissonance, an internal state of conflict that can cause healthcare professionals to experience difficulty in patient interactions, high levels of stress and burnout [ 12 ], emotional “estrangement” (p.443) [ 13 ], and increased intention to leave [ 45 ]. Consistent with these studies, participants in our study felt drained and worn out by the emotional efforts associated with caring for the dying residents. They experienced guilt and feelings of powerlessness and failure, and a significant number expressed their intention to leave the NH.
At the organisational level, studies have demonstrated that poor patient outcomes and poor quality of care, including missing care opportunities and mistreating residents, are potential negative outcomes of emotional exhaustion and unrecognized emotional labour, as well as lower levels of staff recruitment and retention [ 46 ]. In contrast, emerging evidence suggests that when institutional expectations allow and support authentic emotional expression, positive effects can result for healthcare professionals, care recipients, and the healthcare system [ 12 , 14 ].
Implications for policy, practice, and research
The findings from this study expand our understanding of the complex emotional demands associated with caring for dying residents in NHs. Caring for frail older persons requires extensive time, effort, and mental and physical energy, and it involves the interplay of physical and emotional tasks and skills [ 13 ]. These findings represent a valuable contribution to the NH care system, a system that has been predominated by instrumental-focused care. The data highlights the need for a paradigm shift toward valuing the emotional labour involved in accompanying life and death in contexts that are not palliative-care specialised. Upholding quality care alongside the wellbeing of healthcare professionals requires an organisational culture that does not separate instrumental acts from the emotional labour at the very heart of the caring profession. Instead, it requires organisational changes that result in emotional support seen as a collective routine practice that strengthens the team rather than as an individual responsibility and weakness. This will allow NH professionals to regularly share their feelings and emotions, leading to emotional openness and acceptance [ 40 ].
Regular in-service training initiatives should be put in place in NHs to equip healthcare professionals with effective emotional management skills. In particular, the nursing assistants and personal support workers in our study appeared to be most affected by the negative impact of emotional labour. These categories of professional groups require tailored training to help bridge their skill gap. Capacity building approaches such as critical companionship have been proven to equip healthcare professionals with skills on the effective use of emotions in therapeutic relationships and to allow them to reflect on the use of self in caring [ 19 ]. As a lack of institutional support and peer support discourages emotional expression, NH settings should reinforce work environments in which leadership, supervisor, and co-worker support are an integral part of routine practices.
Structural deficiencies such as inadequate staffing, heavy workloads, and competing tasks leave NH healthcare professionals with inadequate time to provide optimal care. This underpins most of the challenges healthcare professionals experience in the NH context and is a primary factor in the emotional burden they experience when they fail to provide quality palliative care to dying residents. There is a need to adapt resource allocation to the complexity of providing palliative care within NHs. Further studies are needed to design interventions that support emotional regulation while increasing the resilience and emotional intelligence of healthcare professionals in NHs.
A strength of our study was the use of individual and focus groups interviews, which enabled a comprehensive exploration of individual and group views on emotional labour of NH professionals. Including professionals involved in direct care and leaders, i.e. nurse and medical coordinators, enabled to capture a diverse set of experiences and perspectives across professional categories and roles. This study did not intend to establish the levels of influence of factors such as professional category, years of work experience, level of interaction with residents or settings characteristics on emotional labour and strategies used. This may constitute the focus of future research.
This study brought to the forefront the complex emotional labour performed by NH professionals while caring for residents requiring palliative care. The results demonstrated that emotions are an undeniable part of caring for frail and dying older persons in the context of a home-like environment; however, current NH culture discourages genuine emotional sharing and emphasizes emotional suppression. Unrecognized emotions undermine the wellbeing of healthcare professionals, leading to negative individual and organisational outcomes. Understanding and acknowledging the emotional labour of NH professionals is critical to supporting their wellbeing, resilience, and retention, and it ultimately may improve the quality of care for dying residents. The stigma surrounding the emotional labour of caring can be broken by decision makers who design healthy workplace environments that celebrate emotional transparency as a strength as well as by each and every healthcare worker who bravely displays their genuine emotions in hopes to shape a new culture that fully acknowledges their humanity alongside their professional skills.
Data availability
The datasets used in this study are available on a reasonable request from the corresponding author.
Honinx E, Van den Block L, Piers R, Onwuteaka-Philipsen B, Payne S, Szczerbińska K, et al. Large differences in the organization of palliative care in nursing homes in six European countries: findings from the PACE cross-sectional study. BMC Palliat care. 2021;20:1–12.
Article Google Scholar
Carpenter JG, Lam K, Ritter AZ, Ersek M. A systematic review of nursing home palliative care interventions: characteristics and outcomes. J Am Med Dir Assoc. 2020;21(5):583–96. e2.
Article PubMed PubMed Central Google Scholar
Reitinger E, Froggatt K, Brazil K, Heimerl K, Hockley J, Kunz R, et al. Palliative care in long-term care settings for older people: findings from an EAPC taskforce. Eur J Palliat Care. 2013;20(5):251–3.
Google Scholar
Froggatt K, Payne S, Morbey H, Edwards M, Finne-Soveri H, Gambassi G, et al. Palliative care development in European care homes and nursing homes: application of a typology of implementation. J Am Med Dir Assoc. 2017;18(6):550. e7-. e14.
Article PubMed Central Google Scholar
Sussman T, Kaasalainen S, Mintzberg S, Sinclair S, Young L, Ploeg J, et al. Broadening end-of-life comfort to improve palliative care practices in long term care. Can J Aging/La Revue Canadienne Du Vieillissement. 2017;36(3):306–17.
Yan Z. I tried to control my emotions: nursing home care workers’ experiences of emotional labor in China. J Cross-Cult Gerontol. 2022;37(1):1–22.
Giesbrecht M, Stajduhar KI, Cloutier D, Dujela C. We are to be like machines… fill the bed before it gets cold: exploring the emotional geographies of healthcare providers caring for dying residents in long-term care facilities. Soc Sci Med. 2021;272:113749.
Article PubMed Google Scholar
Beyrie A, Douguet F, Mino J-C. Accompagner la fin de vie en maison de retraite: spécificités et limites d’un travail inestimable. ethnographiques org. 2017. (35-Vieillir en institution, vieillesses institutionnalisées. Nouvelles populations, nouveaux lieux, nouvelles pratiques).
Curtin M, Richards HL, Fortune DG. Resilience among health care workers while working during a pandemic: a systematic review and meta synthesis of qualitative studies. Clin Psychol Rev. 2022;95:102173.
Chang SO, Kim EY. The resilience of nursing staffs in nursing homes: concept development applying a hybrid model. BMC Nurs. 2022;21(1):129.
Yeh S-CJ, Chen S-HS, Yuan K-S, Chou W, Wan TT. Emotional labor in health care: the moderating roles of personality and the mediating role of sleep on job performance and satisfaction. Front Psychol. 2020;11:574898.
Kim JS. Emotional labor strategies, stress, and burnout among hospital nurses: a path analysis. J Nurs Scholarsh. 2020;52(1):105–12.
Hanlon N. Professional caring in affective services: the ambivalence of emotional nurture in practice. Eur J Social Work. 2023;26(3):441–53.
Xu Y-w. Emotional labor and job satisfaction among nurses: the mediating effect of nurse–patient relationship. Front Psychol. 2023;14:1094358.
Franzosa E, Tsui EK, Baron S. Who’s caring for us? Understanding and addressing the effects of emotional labor on home health aides’ well-being. Gerontologist. 2019;59(6):1055–64.
Wen J, Huang SS, Hou P. Emotional intelligence, emotional labor, perceived organizational support, and job satisfaction: a moderated mediation model. Int J Hospitality Manage. 2019;81:120–30.
Hochschild AR. Travail émotionnel, règles de sentiments et structure sociale 1. Travailler. 2003;1:019–49.
Diefendorff JM, Croyle MH, Gosserand RH. The dimensionality and antecedents of emotional labor strategies. J Vocat Behav. 2005;66(2):339–57.
Smith P, Gray B. Emotional labour of nursing revisited: caring and learning 2000. Nurse Educ Pract. 2001;1(1):42–9.
Badolamenti S, Sili A, Caruso R, FidaFida R. What do we know about emotional labour in nursing? A narrative review. Br J Nurs. 2017;26(1):48–55.
Gray B, Smith P. Emotional labour and the clinical settings of nursing care: the perspectives of nurses in East London. Nurse Educ Pract. 2009;9(4):253–61.
Ingebretsen LP, Sagbakken M. Hospice nurses’ emotional challenges in their encounters with the dying. Int J Qualitative Stud Health well-being. 2016;11(1):31170.
Funk LM, Peters S, Roger KS. The emotional labor of personal grief in palliative care: balancing caring and professional identities. Qual Health Res. 2017;27(14):2211–21.
Fernández-Basanta S, Lois‐Sandá L, Movilla‐Fernández MJ. The link between task‐focused care and care beyond technique: a meta‐ethnography about the emotional labour in nursing care. J Clin Nurs. 2023;32(13–14):3130–43.
Wiersma E, Marcella J, McAnulty J, Kelley ML. That just breaks my heart’: moral concerns of direct care workers providing palliative care in LTC homes. Can J Aging/La Revue Canadienne Du Vieillissement. 2019;38(3):268–80.
Guével M-R, Pommier J. Recherche par les méthodes mixtes en santé publique: Enjeux Et illustration. Santé Publique. 2012;24(1):23–38.
Bagaragaza E, Colombet I, Perineau M, Aegerter P, Guirimand F. Assessing the implementation and effectiveness of early integrated palliative care in long-term care facilities in France: an interventional mixed-methods study protocol. BMC Palliat care. 2023;22(1):35.
Yin RK. Case study research and applications. Sage Thousand Oaks, CA; 2018.
Lambert SD, Loiselle CG. Combining individual interviews and focus groups to enhance data richness. J Adv Nurs. 2008;62(2):228–37.
Patton MQ. Qualitative research & evaluation methods. 3rd ed. Thousand Oaks, CA: Sage; 2002.
Braun V, Clarke V. To saturate or not to saturate? Questioning data saturation as a useful concept for thematic analysis and sample-size rationales. Qualitative Res Sport Exerc Health. 2021;13(2):201–16.
Paillé P, Mucchielli A. L’analyse qualitative en sciences humaines et sociales-5e éd. Armand Colin; 2021.
Maher C, Hadfield M, Hutchings M, De Eyto A. Ensuring rigor in qualitative data analysis: a design research approach to coding combining NVivo with traditional material methods. Int J Qualitative Methods. 2018;17(1):1609406918786362.
Tong A, Sainsbury P, Craig J. Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. Int J Qual Health Care. 2007;19(6):349–57.
Rodriquez J, editor. Editor it’sa dignity thing: nursing Home Care Workers’ Use of emotions 1. Sociological forum. Wiley Online Library; 2011.
Cagle JG, Unroe KT, Bunting M, Bernard BL, Miller SC. Caring for dying patients in the nursing home: voices from frontline nursing home staff. J Pain Symptom Manag. 2017;53(2):198–207.
Holmberg B, Godskesen T. Dignity in Care at the End of Life in a Nursing Home: an Ethnographic Study. 2022.
Östlund U, Blomberg K, Söderman A, Werkander Harstäde C. How to conserve dignity in palliative care: suggestions from older patients, significant others, and healthcare professionals in Swedish municipal care. BMC Palliat care. 2019;18:1–12.
Herr M, Raharimanana S, Bagaragaza E, Aegerter P, Sipos I, Fabre C, et al. Evaluation de la culture de sécurité en etablissement d’Hébergement pour Personnes Agées Dépendantes (EHPAD): adaptation française du questionnaire nursing Home Survey on Patient Safety Culture. Can J Aging/La Revue Canadienne Du Vieillissement. 2017;36(4):453–62.
Funk LM, Peters S, Roger KS. Caring about dying persons and their families: interpretation, practice and emotional labour. Health Soc Care Commun. 2018;26(4):519–26.
Young A, Froggatt K, Brearley SG. Powerlessness’ or ‘doing the right thing’–Moral distress among nursing home staff caring for residents at the end of life: an interpretive descriptive study. Palliat Med. 2017;31(9):853–60.
Bolton S. Changing faces: nurses as emotional jugglers. Sociol Health Illn. 2001;23(1):85–100.
Slootman M, Mudde AL, The AM. Frontstage nursing and backstage growth: the emotional labour of student nurses in Dutch nursing homes. Nurs Inq. 2023;30(4):e12570.
Simard J. Autour de la souffrance soignante en soins palliatifs: entre idéal de Soin et juste distance 1. Frontières. 2014;26(1).
Bartram T, Casimir G, Djurkovic N, Leggat SG, Stanton P. Do perceived high performance work systems influence the relationship between emotional labour, burnout and intention to leave? A study of Australian nurses. J Adv Nurs. 2012;68(7):1567–78.
Eltaybani S, Yamamoto-Mitani N, Ninomiya A, Igarashi A. The association between nurses’ burnout and objective care quality indicators: a cross-sectional survey in long-term care wards. BMC Nurs. 2021;20:1–10.
Download references
Acknowledgements
The authors of this article sincerely thank the funders of this study cited above and the scientific committee members for their valuable support. We acknowledge the contributions of all members of the Padi-Palli team. We are also grateful to the nursing homes and professionals who participated in the study. The authors thank Professor Margaret Fitch for her valuable insights into the manuscript.
This study was supported by the French Ministry of Health and Solidarity through a call for projects PREPS (Healthcare System Performance Research Program): grant number PREPS 19–0066, by the Association des Dames du Calvaire (ADC) and by the Regional Health Agencies (Agence Régionale de Santé) of Ile de France (ARS IDF) and Provence-Alpes-Côte d’Azur (ARS PACA). The funders had no role or responsibilities in the study design, data collection, data management, analysis and interpretation, or publication of this manuscript.
Author information
Authors and affiliations.
Département Recherche Enseignement Formation, Etablissements Jeanne Garnier, 106 avenue Émile Zola, Paris, 75015, France
Benoite Umubyeyi, Danièle Leboul & Emmanuel Bagaragaza
You can also search for this author in PubMed Google Scholar
Contributions
EB conceptualized and designed the study, collected and analysed the data, and revised the manuscript. BU analysed the data and drafted and revised the manuscript. DL analysed the data and revised the manuscript. All authors have reviewed and approved the final manuscript.
Corresponding author
Correspondence to Emmanuel Bagaragaza .
Ethics declarations
Ethics approval and consent to participate.
Research ethics approval for this study was granted by the French Committee of Protection of Person, approval number 2020.09.06 bis 20.07.31.64318. The study is registered in the National Study Database as ID-RCB 2020-A01832-37. The use of databases and data processing were implemented in accordance with French law (“Informatique et Libertés” dated January 6, 1978 and amended June 20, 2018) and European regulations (General Data Protection Regulation - GDPR dated April 27, 2016). All participants provided their informed consent in writing before their inclusion in the study. Confidentiality was ensured using codes and pseudonyms.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Supplementary material 1., supplementary material 2., supplementary material 3., rights and permissions.
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/ .
Reprints and permissions
About this article
Cite this article.
Umubyeyi, B., Leboul, D. & Bagaragaza, E. “ You close the door , wipe your sadness and put on a smiling face ”: a qualitative study of the emotional labour of healthcare professionals providing palliative care in nursing homes in France. BMC Health Serv Res 24 , 1070 (2024). https://doi.org/10.1186/s12913-024-11550-7
Download citation
Received : 28 May 2024
Accepted : 05 September 2024
Published : 16 September 2024
DOI : https://doi.org/10.1186/s12913-024-11550-7
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Nursing home
- Emotional labour
- Staff wellbeing
- Palliative care
- End-of-life care
- Emotional labour strategies
- Healthy environment
- Healthcare professionals
BMC Health Services Research
ISSN: 1472-6963
- General enquiries: [email protected]
Learning and Teaching
- Curriculum Design
- Embedding sustainability
Case study: Student focus groups in Chemical Engineering map path to enhanced climate and sustainability teaching in undergraduate curriculum.
The Department of Chemical Engineering at University of Bath has run focus groups with students to understand how staff can enhance climate and sustainability teaching provision in their courses. In May 2024, the Equality, Diversity, and Inclusion (ED&I) Committee Chair Dr Hannah Leese and departmental Climate Advocate Dr Sandhya Moise co-organised a consultation session with final-year Chemical Engineering students, one of whom also sits on the ED&I Committee. Participants were drawn from the MEng Chemical Engineering and MEng Environmental Engineering courses. The focus groups prioritised discussion of the links between sustainability and social justice in these disciplinary contexts.
Published on: 16/09/2024 · Last updated on: 18/09/2024
Questions of social justice are central to the relationship between engineering, climate, and sustainability.
The impetus for the consultation, which aligned climate change, sustainability, and ED&I efforts across the department, stemmed from the recognition that climate change is intricately linked with questions of social justice: climate change disproportionately affects vulnerable and marginalised communities, limiting their access to resources such as clean water, food, energy, and healthcare. As such, engineering solutions must be inclusive and avoid exacerbating inequalities. Future engineers must be equipped with the skills and tools to evaluate climate change solutions through a lens of equality, diversity, and inclusivity. How, then, can engineering curricula respond to this challenge?
Insights on curriculum design and delivery
The student focus groups identified key areas that will feed into the continuous development of the Chemical Engineering curriculum:
- Whilst Chemical Engineering curricula have successfully embedded knowledge and tools to assess various aspects of environmental sustainability, the discipline and its curricula would benefit from increased focus on people and social justice.
- Adopting principles of course-wide design, the links between environmental sustainability and social justice should be signposted at all levels of the curriculum.
- Students are especially excited by novel and innovative areas of study (e.g. renewable energies, hydrogen, biotech).
- Students value explicit marking criteria around sustainability and inclusive design in engineering.
Prioritising student voice and co-creation in climate and sustainability education initiatives
Student feedback on the session was very positive: “I found the EDI-Sustainability focus group to be valuable, as it provided a safe space to voice our views and experiences, and to reassure us that diverse student perceptions and viewpoints are heard and valued. My main takeaways were a deeper understanding of existing EDI and sustainability initiatives in the department, and how these aspects are currently recognised and embedded into the Chemical Engineering curriculum. I appreciated the opportunity to give constructive feedback on how this can be built upon, with the understanding this can be used for continuous improvement for future cohorts.”
Next steps: consolidating climate and sustainability provision and ED&I perspectives across Chemical Engineering courses
Following the focus groups, the Department is introducing further mechanisms to ensure that students are at the heart of its initiative to align climate and sustainability education with ED&I and social justice perspectives. The Department of Chemical Engineering will continue working alongside the Chemical Engineering Sustainability Group (CESG; a subsidiary of the Chemical Engineering Student Association) to enable students to drive the sustainability agenda forward within the department. Dr Moise runs a ‘Climate change and Chemical Engineering’ talk in Freshers Week to foreground this aspect of the curriculum and to signpost the CESG. The CESG President is also regularly invited to appropriate lectures across year groups to remind students of opportunities for engagement. In parallel, the ED&I Committee Chair attends all Head of Department Welcome Talks for Freshers and returning students and is working closely with teaching staff across the Department to support students to reflect on inclusive design, and ED&I experiences. Provision in this area is driven by a broad belief that both ED&I perspectives and climate and sustainability education necessitate an engagement with students’ broader lived experience, an insight borne out by the focus groups.
Find out more
Do you want to know more about embedding climate and sustainability skills in your teaching? Find guidance and resources for embedding sustainability in the curriculum on the Teaching Hub, or learn more about Climate Action Education at Bath.

Related Articles
- Case Study: A course-wide approach to embedding climate and sustainability skills in Electronic and Electrical Engineering degrees
- Embedding sustainability in the curriculum
- Case study: Empowering students with design thinking
- Identifying sustainability in the curriculum
Article Contents

Battlefield Triage A Resolvable Moral Tragedy
Article sidebar.

Main Article Content
In a non-military setting, the answer is clear: it would be unethical to treat someone based on non-medical considerations such as nationality. We argue that Battlefield Triage is a moral tragedy, meaning that it is a situation in which there is no morally blameless decision and that the demands of justice cannot be satisfied.
INTRODUCTION
Medical resources in an austere environment without quick recourse for resupply or casualty evacuation are often limited. The shortage extends not only to supplies like blood products and drugs, but physicians and other medical personnel. In the midst of a mass casualty scenario, such as a battle that includes intense ground fighting, the medical staff will stretch scarce resources and triage casualties according to specific criteria. Typically, they proceed by providing care for the most severely wounded first, referred to here as conventional triage. At times, though, the staff may reverse the triage so that soldiers with minor wounds can return to the fight. In a mass casualty situation, when medical personnel apply conventional triage and treat casualties from opposing forces, a dilemma may arise. We argue that it can be permissible for military physicians to prioritize their own soldiers over enemy combatants in a mass casualty triage, where reverse triage does not apply. The case we will focus on is as follows:
Battlefield Triage: During combat operations on a remote island in the Pacific Ocean, a compatriot soldier and an enemy combatant arrive at the compatriot soldier country’s medical treatment facility. Both have similar gunshot wounds to the abdomen, and they arrive with similar conditions. Both have low oxygen saturation and excessive blood loss. The sole physician only has enough time to stabilize one person.
The scenario is brief, and we are aware that medical rules of eligibility will most often dictate how the physician proceeds, [1] but this scenario is useful in setting up the question we focus on in this paper: would it be wrong to favor the stabilization of a soldier just because the soldier is the physician’s compatriot? In other words, can nationality serve as an ethically justified tiebreaker in a situation such as Battlefield Triage? [2]
In a non-military setting, the answer is clear: it would be unethical to treat someone based on non-medical considerations such as nationality. The AMA’s Code of Medical Ethics asserts that physicians have “ethical obligations to place patients’ welfare above their self-interest and above obligations to other groups.” [3] The World Medical Association’s Declaration of Tokyo affirms that “no motive, whether personal, collective or political, shall prevail against this higher purpose” of alleviating distress. [4] Physicians are taught early on that triage decisions must be medically indicated and made without consideration of factors such as race, ethnicity, religion, social status, and nationality. They are taught that public trust and obligations of justice grounded in equality demand that only medical indications be considered. But military physicians in a military setting are beholden to obligations, duties, and responsibilities as members of the military, and when these obligations, duties, and responsibilities conflict, as they do in Battlefield Triage, which loyalties win out and why? [5]
Critics of partiality on national grounds argue that partiality undermines public trust in medicine and justice because everyone should be treated equally regardless of nationality. [6] Proponents of partiality argue that military obligations supersede equality and that justice requires partiality in such cases. [7] Despite the critics’ disagreement, both agree that there is a morally right, perhaps even blameless, course of action. Drawing on insights from virtue ethics, we argue that Battlefield Triage is a moral tragedy in which justice is unattainable and there is no action without moral cost. The assumption that there is a morally right choice is flawed. We argue that while no decision in this scenario is free from moral blame, there are reasons to favor treating one’s soldiers over enemy combatants.
I. The Case Against Partiality
There is a common assumption that there is a morally right or just decision in Battlefield Triage. A number of organizations and scholars claim that it is wrong for military physicians to favor their own soldiers on the grounds of nationality or some form of ‘group membership.’ (In a conflict involving service members from multiple nations working as a coalition, a soldier from an allied country may receive the same priority as the US service member due to ‘group membership.’) The World Medical Association’s WMA Declaration of Lisbon on the Rights of the Patient, which was reaffirmed in 2015, posits that, “[i]n circumstances where a choice must be made between potential patients for a particular treatment that is in limited supply, all such patients are entitled to a fair selection procedure for that treatment. That choice must be based on medical criteria and made without discrimination.” [8] This echoes what was set forth in Article 12 of the Geneva Conventions, which states that “[o]nly urgent medical reasons will authorize priority in the order of treatment to be administered.” [9] The argument for impartiality in Battlefield Triage is that every person is morally equal, and equality entails that medical distribution is, “based on a combination of medical need and urgency.” [10] This is in keeping with the bioethical principles that are generally applied. [11]
II. The Case for Partiality
On the other side, there are arguments that favoritism is the ethically right decision in Battlefield Triage. [12] The argument asserts that members of the military form a morally significant community of friends and participation in these relationships demands partiality. Just as parents have strong ethical duties to their children and not just any children, military personnel have ethical duties to their group, a group that involves an affirmation of mutual aid and support. Some have termed these ‘associative duties. According to Michael Gross, obligations of friendship, care, and solidarity “leave very little room for generally applicable principles of justice that would obligate a medic to treat enemy or non-compatriot wounded ahead of their compatriots.” [13] This is true in Battlefield Triage, but it may also be true even if the enemy’s soldier were more seriously wounded: “the ethics of small group cohesion, largely an ethics of care, mostly replaces the demands of impartial justice.” [14] In a more recent article, Gross explains that preferential treatment is ethically justified based on fighting capability and “the special obligations people owe friends, family, and, no less, comrades-in-arms.” [15] To not show partiality to the US soldier would be morally wrong on the grounds of friendship and mutual care. [16]
III. The Moral Tragedy of Battlefield Triage
Defenders and critics of Battlefield Triage favoritism based on nationality both frame their position as just or fair. For example, Justin List argues that physicians are “bound to practice medical neutrality,” [17] Marcus Adams denies that physicians “possess special ethical obligations” to enemy combatants because of their profession. [18] These perspectives assume that there is a morally right decision and that justice is attainable. The assumption that there is or can be a morally right Battlefield Triage decision, and we need to put our heads together to figure it out, remains strongly entrenched. However, the facts of the situation should give us pause; there are too many people and too few resources, and this demands a decision-making process that determines who will receive scarce resources. By its very nature, a battlefield triage decision has to be made based on some characteristic or value, a characteristic or value that will inevitably favor some at the expense of others. This is precisely why competing analyses “in the military context struggle to resolve these conflicts satisfactorily.” [19]
Drawing on the insights of virtue ethics, we suggest that Battlefield Triage is a moral tragedy. Virtue ethics suggests that morality is about acting virtuously, which is to say that we should do what a virtuous person would do in the situation. Ethics is about figuring out how a just, wise, compassionate, loving, and fair person would act, and then doing that, as one grows in virtue. But life is not always clear cut, and it is possible that virtuous people may find themselves in a moral tragedy, a situation in which, through no fault of one’s own, a person must make a morally objectionable decision. After the action the virtuous person “emerges having done a terrible thing, the very sort of thing that the callous, dishonest, unjust, or in general vicious agent would characteristically do.” [20] Stated differently, a moral tragedy presents a virtuous person with two or more courses of action, all of which have a moral cost. [21] In Battlefield Triage, no matter how the physician goes about deciding, there is going to be defensible concern from those not saved. The fact that there are more people than can be helped fosters competing values in battlefield triage: maximize lives saved, treat people equally, treat the worse off, and support the war effort. Treating people equally may create tension between treating the worse off, maximizing lives saved, and supporting the war effort. Reverse triage is a case in point, as supporting the war effort conflicts with treating the worse off first, as is a fair lottery system since deploying a lottery may not maximize lives saved or support the war effort. There can be reasons why one person is selected over another, to be sure. Yet, there are reasons for making a decision, and that the decision is subject to legitimate moral concern is another.
To recognize the moral tragedy of Battlefield Triage is to recognize the impossibility of acting blamelessly in the situation. In this situation, the virtuous military physician is going to have to sacrifice important values such as justice, compassion, and respect for others, even with a defensible criterion in hand. The physician will grieve this sacrifice accordingly. The physician may find her decision difficult or stressful, and rightly so, because of what her circumstances require of her. This kind of moral tragedy results “in actions which betray and violate the rights of persons to whom there may be a strong duty of care. When this happens, it properly triggers an appropriate moral emotion since our moral integrity has been violated and this affects how we think of ourselves and what we have become.” [22] Rather than view her triage decision as the morally superior choice, the virtuous military physician will view her decisions in these circumstances in a different light: it is the least bad option in a terrible situation, and she did something ethically problematic, something that is contrary to her moral character. She deeply regrets the circumstances in which she had to act.
IV. Virtue Ethics
A virtue ethicist has insight into how one should go about deciding what to do in a moral tragedy, although virtue ethics may not be as helpful as one may hope. The goal of the virtuous military physician in Battlefield Triage is to adopt the best course of action or the action that she feels she ought to do, all things considered. This does not make her choice devoid of serious wrongdoing—a decision must be made, but that does not make it just. The virtuous military physician will approach the situation with courage, responsibility, and insight. She will think about the decision carefully, wisely, and conscientiously; she will weigh the goods and harms of the choices before her, in conjunction with a proper conception of the good life, human worth, and understanding of her obligations to others—including chain of command, fellow soldiers, and the medical community. She is attuned to the value of human life and has a reasonable idea of the various ways her decisions will affect others. She recognizes that she is in this non-ideal situation through no fault of her own: she is not the one fighting in battles; she is serving her country as a physician, whose job it is to save lives, treat everyone justly, and promote military objectives. She regrets the decision she is forced to make in battlefield triage, acting “with immense regret and pain,” Hursthouse explains, “instead of indifferently or gladly.” [23] This is because, no matter what decision is made, the virtuous military physician “does something terrible or horrible,” something she otherwise would not do and is contrary to her values. [24]
V. A Resolvable Moral Tragedy
Instead of asking whether there is a morally right decision, in which a decision is morally blameless and above reproach, the virtue ethicist asks whether there is a decision with a convincing rationale, knowing that a decision can have a clear rationale but still be morally tragic. It is perfectly reasonable to think that different virtuous persons will arrive at different courses of action: “two virtuous agents, in the same situation,” Hursthouse writes, “may act differently” in irresolvable moral tragedies, in cases in which there is no clear course of action. [25]
Because a person must act in a moral tragedy, one goal is to identify reasons for choosing the chosen action. Some decisions are clearly indefensible—treating neither the compatriot soldier nor the enemy combatant in Battlefield Triage would be wrong—and some decisions are more problematic than others. If the military physician selects to treat the soldier because she does not like the enemy combatant’s skin color, such a reason would be deeply problematic. But much of the debate over how to act in a moral tragedy is not over clearly indefensible or problematic criteria.
Instead, the literature is largely about different standards or implementations of justice. Some scholars defend nation-impartial triage as right, while others defend nation-aware triage as right, and each argues that the other side is promoting an unjust or otherwise wrong solution to Battlefield Triage.
We suggest that Battlefield Triage is a resolvable moral tragedy and that virtue ethics offers convincing reasons to prefer the treatment of the compatriot soldier rather than the enemy combatant on the grounds of national identity. Virtues are integral to living a good life, a flourishing life, but as Aristotle observed long ago, human beings are inherently social, interdependent and interconnected in profound ways. [26] This goes beyond the obvious fact that we need each other to survive day to day (one person makes clothes, another farms, and another makes tools); the claim is that a good or flourishing life depends in large part on one’s social network or community. This is why many of Aristotle’s moral virtues are other facing: justice, friendship, generosity, and magnanimity, to name a few. Courage, a typically self-facing virtue, is understood by Aristotle to be the virtue that regards one’s fear of death in battle, a battle fought on behalf of one’s city. [27] All of this remains true today. Namely, there is an important sense in which our community matters to our lives: it is easier to live a good, flourishing life if one is part of a good, flourishing community.
Our community is made up of smaller groups, and it is more accurate to say that we are simultaneous members of different groups within a broader community. A person may be part of a family, friend group, research team, large state university, city, state, and nation. Groups can function well or not, as we all have experienced, and this suggests that there are virtues or excellences that groups can instantiate. Good groups are unified in purpose, with each member doing their duty alongside others for the attainment of that purpose. Good groups manifest solidarity among their members. Although Aristotle does not list solidarity as a virtue, a number of modern-day virtue ethicists have begun examining how group solidarity can be a virtue that contributes to a good or flourishing life. [28] Solidarity is not conceptualized as an individual virtue, a virtue possessed by a person in isolation of others; instead, it is a collective virtue, a virtue that is shared among members of a defined group with particular ends. [29]
“A group has solidarity to the extent that its members are disposed to: (1) share values, aims, or goals; (2) care about those values, aims, or goals; (3) act in accordance with those values, aims, or goals; (4) trust the testimony of other group members with respect to those values, aims, and goals; and (5) feel a sense of belonging to the group.” [30]
The virtue of collective or group solidarity involves individuals having special concern for each other, shared aims and values, trust, loyalty, and a sense of belonging with these specific others. There is a oneness to the group in the pursuit of a definite goal or purpose, involving mutual support and affirmation of each member. As such, the group has ends and goods above and beyond the good of each individual person. Sometimes solidarity requires personal sacrifice for the collective (for example, a father sacrificing food so his child can eat).
The virtue of collective or group solidarity is important to the military and medical community at every level, and for clear reasons. In the military, there is a clear hierarchy of command, unity of purpose and end, mutual trust and support in complex settings, and so on. Soldiers need to know they can count on one another, and solidarity grounds a soldier’s ability to trust others and be assured of mutual aid. In medicine, solidarity maintains self-regulation of the profession, shared values and goals, as well as public support, not to mention that day-to-day operations require physician trust, engagement, and effort toward the ends of clinical care. Physicians need to work together, along with others, in pursuit of health, and disunity is sowed when there is mistrust, selfishness, or disengagement among the healthcare team and organization. Importantly, just as we are all members of various groups and hence may manifest group solidarity in different settings, the virtuous military physician instantiates collective solidarity with both the medical profession and the military. Her dual loyalty contributes to the moral difficulty of acting in Battlefield Triage.
The military physician has competing obligations to distinct groups and cannot satisfy all obligations in Battlefield Triage. Solidarity with the military supports the consideration of favoring the soldier for reasons of national identity, whereas solidarity with the medical community does not. Something has to give, which is why it is a moral tragedy. The virtuous military physician, therefore, must weigh the costs of each course of action. To fulfill her obligations to the medical community would require that she does not use nationality and other non-medical considerations in Battlefield Triage. Since the soldier and enemy combatant are equally injured, justice would demand a random process, perhaps a flip of the coin. Although this may satisfy obligations the military physician has to the medical community, this would be costly to the physician’s military group. If word gets out that the physician decides who to treat based on a coin toss, soldiers, families, and citizens may become frustrated and angry. Soldier morale may go down if it becomes known that a coin flip led to the preventable death of a soldier and the saving of an enemy combatant who had killed (or attempted to kill) other soldiers. As Gross highlights, military solidarity involves a mutual aid promise that military personnel promise to help one another. [31] A military physician is part of the military and, as such, is part of the mutual aid promise, which would appear to be violated if the physician flips a coin. Treating a member of one’s own team may be psychologically more beneficial than treating an enemy combatant and may lead to less moral distress. [32] Finally, treating soldiers rather than enemy combatants promotes broader military and social aims, including returning soldiers to health, maintaining unity of purpose, and minimizing community suffering from a soldier’s death.
Favoring members of one’s group, that is, triage based on nationality in Battlefield Triage, would fulfill obligations of military group loyalty, which is contrary to the values and duties of medicine. It does not seem as though showing favoritism in this particular situation is very costly to the medical community or general public, but this is because there is recognition that the physician is in the military. Medicine is impartial to non-medical indications partly because of fairness and to promote public trust in medicine. However, Battlefield Triage is unique, as medicine is being practiced in a non-public, wartime setting. In ordinary circumstances, a patient’s identity is irrelevant, and physicians ought not play favorites. Since Battlefield Triage is not an ordinary circumstance, decisions based on patient identity may not undermine public trust in medicine.
In addition, it is contestable that fairness in Battlefield Triage requires that no consideration be paid to one’s nationality. Fairness is about giving each person their due, what is owed to them, and the case can be made that soldiers who place themselves in danger for the sake of the common good or a just cause are owed special attention when they suffer harm in the line of duty. In other words, soldiers voluntarily undergo risk to themselves for the greater good, and society owes them for this sacrifice. This plausibly includes preferential treatment in a situation such as Battlefield Triage. So, while the medical community affirms justice demands non-preferential treatment, the military community can affirm the opposite. The demands of fairness are unclear at best or in conflict in this situation: demands of physician justice decry favoritism, while demands of military justice support favoritism. Triage not based on nationality is arguably unfair and triage based on nationality may not undermine public trust, after all.
All things considered, there is a clear rationale for favoring nationality-based preferential treatment in Battlefield Triage. Adopting a nationality-based preference in this situation is more defensible than not. This does not make such a decision ethically right or just. Preference based on nationality is the least bad decision, but it is not morally blameless. It involves one in a serious moral wrong, a wrong otherwise avoided and contrary to one’s character. The virtuous military physician is in a situation in which obligations conflict, and we disagree with Gross, who posits that care of fellow soldiers “is important to the near exclusion of all else.” [33] Gross fails to appreciate the collective virtue of solidarity as applied to those in medicine. The military physician has duties to fellow soldiers but also to fellow physicians, to the medical community, and humanity. To favor a soldier on grounds of nationality violates her duties and responsibilities to this latter group. She is involved in a moral tragedy and can only seek the most just action given the circumstances, yet, at least in virtue ethics, the action remains far from blameless.
We argue that Battlefield Triage is a moral tragedy, meaning that it is a situation in which there is no morally blameless decision and that the demands of justice cannot be satisfied. As such, the virtuous military physician incurs a moral cost to acting as she does—there is a moral residue. However, despite being a moral tragedy, there are clear reasons to act in favor of treating one’s own, considering group solidarity. As such, these kinds of tragedies are resolvable: virtuous military physicians should favor treatment of their own, although they would do so with sorrow.
[1] Militaries set forth medical rules of eligibility or guidelines used to determine whether a person qualifies for specific medical interventions or treatments in certain circumstances, and these guidelines are binding for a military physician. For example, despite opposition from medical organizations, militaries have adopted reverse triage guidelines for military physicians to follow. For ethical discussion, see Falzone, Elisabeth, P. Pasquier, C. Hoffmann, O. Barbier, M. Boutonnet, A. Salvadori, A. Jarrassier, J. Renner, B. Malgras, and S. Mérat. "Triage in military settings." Anaesthesia Critical Care & Pain Medicine 36, no. 1 (2017): 43-51. https://doi.org/10.1016/j.accpm.2016.05.004
[2] There are issues that are related to this, including the triage of civilians and allied soldiers. We set related issues aside for purposes of this paper
[3] American Medical Association, Code of Medical Ethics: Current Opinions with Annotations, 2004–2005 ed. (Chicago, IL: AMA, 2004), 300.
[4] American Medical Association, Code of Medical Ethics: Current Opinions with Annotations, 2004–2005 ed. (Chicago, IL: AMA, 2004), 300.
[5] This is termed the “dual loyalty” dilemma in military medicine and has been described at length elsewhere: Institute of Medicine (US) Board on Health Sciences Policy. Military Medical Ethics: Issues regarding Dual Loyalties: Workshop Summary. Washington (DC): National Academies Press (US); 2008. Toward a Framework for Resolving Dual Loyalties. Available from: https://www.ncbi.nlm.nih.gov/books/NBK214853/
[6] See Kenneth G. Swan and K.G. Swan, Jr., “Triage: The Past Revisited,” Military Medicine 161:8 (1996): 448–452. https://doi.org/10.1093/milmed/161.8.448; Jerome A. Singh, “American Physicians and dual loyalty obligations in the ‘war on terror,’” BMC Medical Ethics 4.4 (2003): 1–10. https://doi.org/10.1186/1472-6939-4-4; Beam, Thomas E. "Medical Ethics on the Battlefield." Military Medical Ethics: Sect. IV. Medical ethics in the military. Medical ethics on the battlefield: the crucible of military medical ethics 2 (2003): 369-402; Hereth, Blake. "Health justice for unjust combatants." Journal of Military Ethics 20, no. 1 (2021): 67-81. https://doi.org/10.1080/15027570.2021.1949782.
[7] See Adams, Marcus P. "Triage priorities and military physicians." In Physicians at war: The dual-loyalties challenge, pp. 215-236. Dordrecht: Springer Netherlands, 2008. Gross, Michael L. "Comradery, community, and care in military medical ethics." Theoretical medicine and bioethics 32 (2011): 337-350. https://doi.org/10.1007/s11017-011-9189-6. Gross, Michael L. "The limits of impartial medical treatment during armed conflict." In Military medical ethics for the 21st century, pp. 71-84. Routledge, 2016.
[8] World Medical Association, WMA Declaration of Lisbon on the Rights of the Patient. 5 December 2022, https://www.wma.net/policies-post/wma-declaration-of-lisbon-on-the-rights-of-the-patient/
[9] Geneva Convention for the Amelioration of the Condition of Wounded, Sick in Armed Forces in the Field. 12 August 1949. https://www.un.org/en/genocideprevention/documents/atrocity-crimes/Doc.30_GC-I-EN.pdf.
[10] List, Justin M. "Medical neutrality and political activism: physicians' roles in conflict situations." In Physicians at war: The dual-loyalties challenge, pp. 237-253. Dordrecht: Springer Netherlands, 2008. 240
[11] Beauchamp, T., and J. Childress. 2013. Principles of Biomedical Ethics, 7th ed. Oxford, United Kingdom: Oxford University Press.
[12] Adams, Marcus P. "Triage priorities and military physicians." In Physicians at war: The dual-loyalties challenge, pp. 215-236. Dordrecht: Springer Netherlands, 2008.
[13] Gross, "Comradery, community, and care in military medical ethics," 347.
[14] Gross, “Comradery, community, and care in military medical ethics,” 349.
[15] Gross, Michael L. "When medical ethics and military ethics collide." Narrative inquiry in bioethics 13, no. 3 (2023): 199-204. 202 https://dx.doi.org/10.1353/nib.2023.a924191
[16] Our argument draws on virtue ethics, from which care ethics derives, and it is worth clarifying how our argument relates to Gross’s. We do not think that the virtue of friendship grounds triage decisions, for we think it is unlikely that the physician and wounded soldier are friends. Instead, as explained below, we think the collective virtue of group solidarity better captures the moral significance of group loyalty and that Gross would agree with us. But since military physicians are part of distinct groups, with competing obligations, the military physician will be forced to sacrifice a value in battlefield triage cases. In other words, we think Gross downplays the dual group membership of a military physician.
[17] List,”Medical neutrality and political activism,” 250.
[18] Adams,”Triage priorities and military physicians,” 235.
[19] London, Leslie, Leonard S. Rubenstein, Laurel Baldwin-Ragaven, and Adriaan Van Es. "Dual loyalty among military health professionals: human rights and ethics in times of armed conflict." Cambridge Quarterly of Healthcare Ethics 15, no. 4 (2006): 381-391. 383.
[20] Hursthouse, R. On Virtue Ethics. OUP 1999. 74
[21] Nussbaum, Martha C. "The costs of tragedy: Some moral limits of cost-benefit analysis." The Journal of Legal Studies 29, no. S2 (2000): 1005-1036, 1007.
[22] De Wijze, S. (2005). Tragic-remorse–the anguish of dirty hands. Ethical theory and moral practice, 7(5), 453-471, 457. https://doi.org/10.1007/s10677-005-6836-x
[23] Hursthouse, 73
[24] Hursthouse, 81
[25] Hursthouse, 72
[26] Aristotle, Politics 1253a8. Reeve, C. D. C., Indianapolis: Hackett Publishing Co., 2017
[27] Aristotle, Nicomachean Ethics. III.6.114a, 34-35. 2002, Nicomachean Ethics, Christopher Rowe (trans.), Oxford: Oxford University Press
[28] Byerly, T. Ryan, and Meghan Byerly. "Collective virtue." The Journal of Value Inquiry 50, no. 1 (2016): 33-50. https://doi.org/10.1007/s10790-015-9484-y; Federico, Veronica. "Conclusion: solidarity as a public virtue." Solidarity as a Public Virtue (2018): 495-542. https://doi.org/10.5771/9783845290058 . Rehg, William. "Solidarity and the common good: An analytic framework." Journal of Social Philosophy 38, no. 1 (2007): 7-21. https://doi.org/10.1111/j.1467-9833.2007.00363.x
[29] Byerly and Byerly. "Collective virtue." 43
[30] Battaly, Heather. "Solidarity: Virtue or vice?." In Social virtue epistemology, pp. 303-324. Routledge, 2022. 304
[31] Ibid., 2011: 341
[32] It might be thought that displaying altruism by helping an enemy combatant at the expense of one’s fellow soldier may be psychologically satisfiying. For evidence that military physicians find it difficult to treat enemy combatants, see Lundberg, Kristina, Sofia Kjellström, Anders Jonsson, and Lars Sandman. "Experiences of Swedish military medical personnel in combat zones: adapting to competing loyalties." Military medicine 179, no. 8 (2014): 821-826. https://doi.org/10.7205/MILMED-D-14-00038. Lamblin, Antoine, Clément Derkenne, Marion Trousselard, and Marie-Ange Einaudi. "Ethical challenges faced by French military doctors deployed in the Sahel (Operation Barkhane): a qualitative study." BMC Medical Ethics 22 (2021): 1-13. https://doi.org/10.1186/s12910-021-00723-2
[33] Ibid., 2011: 344
Christopher Bobier
Associate Professor of Bioethics and Health Policy Central Michigan University's College of Medicine, MA and PhD Philosophy University of California, Irvine
Daniel Hurst
Associate Professor and Director of Professionalism, Ethics & Humanities Rowan-Virtua School of Osteopathic Medicine, PhD Healthcare Ethics Duquesne University, MS Global Health and Infectious Disease University of Edinburgh
Article Details

This work is licensed under a Creative Commons Attribution 4.0 International License .
- Fact sheets
- Facts in pictures
- Publications
- Questions and answers
- Tools and toolkits
- Endometriosis
- Excessive heat
- Mental disorders
- Polycystic ovary syndrome
- All countries
- Eastern Mediterranean
- South-East Asia
- Western Pacific
- Data by country
- Country presence
- Country strengthening
- Country cooperation strategies
- News releases
- Feature stories
- Press conferences
- Commentaries
- Photo library
- Afghanistan
- Cholera
- Coronavirus disease (COVID-19)
- Greater Horn of Africa
- Israel and occupied Palestinian territory
- Disease Outbreak News
- Situation reports
- Weekly Epidemiological Record
- Surveillance
- Health emergency appeal
- International Health Regulations
- Independent Oversight and Advisory Committee
- Classifications
- Data collections
- Global Health Observatory
- Global Health Estimates
- Mortality Database
- Sustainable Development Goals
- Health Inequality Monitor
- Global Progress
- World Health Statistics
- Partnerships
- Committees and advisory groups
- Collaborating centres
- Technical teams
- Organizational structure
- Initiatives
- General Programme of Work
- WHO Academy
- Investment in WHO
- WHO Foundation
- External audit
- Financial statements
- Internal audit and investigations
- Programme Budget
- Results reports
- Governing bodies
- World Health Assembly
- Executive Board
- Member States Portal
Technical Advisory Group on Clinical and Policy Considerations for New Tuberculosis (TB) Vaccines
Call for experts, issued on: 18 september 2024, deadline: 26 september 2024.
The World Health Organization (WHO) is seeking regulators and regulatory experts to serve as members on Technical Advisory Group on clinical and policy considerations for new Tuberculosis (TB) vaccines. This “Call for experts” provides information about the advisory group in question, the expert profiles being sought, the process to express interest, and the process of selection.
Please note: This call was previously posted in July 2024; this is a second call to recruit additional regulatory experts and regulators, specifically.
Tuberculosis (TB) is a leading cause of death from an infectious agent, and a major contributor to antimicrobial resistance. About a quarter of the world’s population has been infected with Mycobacterium tuberculosis, most living in low-and-middle income countries. This population is at risk of developing TB disease. An estimated 10.6 million people fell ill with TB in 2022, an estimated 1.3 million people died.
W HO seeks to advance the development and deployment of new TB vaccines to prevent TB disease, with a focus on adolescents and adults in whom 90% of TB disease occurs. Prevention of TB disease in these populations, responsible for most of the transmission, will significantly reduce disease and incidence in all those at risk, including unvaccinated infants, children, older adults and other key populations, such as people living with HIV. There are several vaccine candidates in the pipeline, many in late-stage development, and effort is needed now to co-ordinate and where feasible align on regulatory expectations, provide guidance on clinical aspects such as optimal clinical endpoints and on anticipated evidence needs for policy at the global, regional and national levels.
WHO recently established the TB Vaccine Accelerator Council to facilitate the development, testing, authorization, & use of new TB vaccines. This TAG would form part of the working groups associated with the TB Vaccine Accelerator.
Functions of the Technical Advisory Group on Clinical and Policy Considerations for New Tuberculosis (TB) Vaccines
- To provide independent evaluation of the scientific and strategic clinical, regulatory and policy aspects related to new TB vaccine candidates, including but not limited to safety, immunogenicity, efficacy, anticipated impact and effectiveness, resulting in recommendations on data requirements, study designs, clinical trial protocols and regulatory strategies.
- To advise WHO on evidence to support policy formulation, optimal programmatic delivery strategies and where appropriate implementation science to accelerate the pathway to recommendation, introduction and use of new TB vaccines at the country and global levels.
- To assist the secretariat in developing novel guidance / communication on WHO positions with respect to aspects such as clinical endpoints, case definitions, expected data and evidence needs, trade-offs, to inform investment and introduction decision-making.
Operations of the Technical Advisory Group on Clinical and Policy Considerations for New Tuberculosis (TB) Vaccines
The TAG shall normally meet face-to-face at least once each year, and virtually up to 8 times per year. Interim teleconferences and review of draft documents may be required of the members. The working language of the group will be English.
Who can express interest?
The Technical Advisory Group (TAG) on clinical and policy considerations for new Tuberculosis (TB) vaccines will be multidisciplinary, with members who have a range of technical knowledge, skills and experience relevant to novel TB vaccines, specifically their clinical development, regulatory approval, policy and implementation considerations to support WHO prequalification. Approximately 25 individuals may be selected.
For this call, WHO welcomes expressions of interest from regulators, or experts with regulatory experience, particularly from high TB burden countries. Please note that we cannot accept applications from the private sector.
Submitting your expression of interest
To register your interest in being considered for the TAG on clinical and policy considerations for new Tuberculosis (TB) vaccines, please submit the following documents by 26 September 2024 to [email protected] using the subject line “Expression of interest for the ‘Clinical and policy TAG on new TB vaccines’:
- A cover letter, indicating your motivation to apply and how you satisfy the selection criteria. Please note that, if selected, membership will be in a personal capacity. Therefore do not use the letterhead or other identification of your employer;
- Your curriculum vitae (including your nationality/ies) and
- A signed and completed Declaration of Interests (DOI) form for WHO Experts, available at https://www.who.int/about/ethics/declarations-of-interest .
Important information about the selection processes and conditions of appointment
Members of WHO advisory groups (AGs) must be free of any real, potential or apparent conflicts of interest. To this end, applicants are required to complete the WHO Declaration of Interests for WHO Experts, and the selection as a member of a AG is, amongst other things, dependent on WHO determining that there is no conflict of interest or that any identified conflicts could be appropriately managed (in addition to WHO’s evaluation of an applicant’s experience, expertise and motivation and other criteria).
All AG members will serve in their individual expert capacity and shall not represent any governments, any commercial industries or entities, any research, academic or civil society organizations, or any other bodies, entities, institutions or organizations. They are expected to fully comply with the Code of Conduct for WHO Experts ( https://www.who.int/about/ethics/declarations-of-interest ). AG members will be expected to sign and return a completed confidentiality undertaking prior to the beginning of the first meeting.
At any point during the selection process, telephone interviews may be scheduled between an applicant and the WHO Secretariat to enable WHO to ask questions relating to the applicant’s experience and expertise and/or to assess whether the applicant meets the criteria for membership in the relevant AG.
The selection of members of the AGs will be made by WHO in its sole discretion, taking into account the following (non-exclusive) criteria: relevant technical expertise; experience in international and country policy work; communication skills; and ability to work constructively with people from different cultural backgrounds and orientations .The selection of AG members will also take account of the need for diverse perspectives from different regions, especially from low and middle-income countries, and for gender balance.
If selected by WHO, proposed members will be sent an invitation letter and a Memorandum of Agreement. Appointment as a member of a AG will be subject to the proposed member returning to WHO the countersigned copy of these two documents.
WHO reserves the right to accept or reject any expression of interest , to annul the open call process and reject all expressions of interest at any time without incurring any liability to the affected applicant or applicants and without any obligation to inform the affected applicant or applicants of the grounds for WHO's action. WHO may also decide, at any time, not to proceed with the establishment of the AG, disband an existing TAG or modify the work of the AG.
WHO shall not in any way be obliged to reveal, or discuss with any applicant, how an expression of interest was assessed, or to provide any other information relating to the evaluation/selection process or to state the reasons for not choosing a member.
WHO may publish the names and a short biography of the selected individuals on the WHO internet.
AG members will not be remunerated for their services in relation to the AG or otherwise. Travel and accommodation expenses of AG members to participate in AG meetings will be covered by WHO in accordance with its applicable policies, rules and procedures.
The appointment will be limited in time as indicated in the letter of appointment.
If you have any questions about this “Call for experts”, please write to [email protected] well before the applicable deadline.

IMAGES
VIDEO
COMMENTS
Step 1: Choose your topic of interest. Step 2: Define your research scope and hypotheses. Step 3: Determine your focus group questions. Step 4: Select a moderator or co-moderator. Step 5: Recruit your participants. Step 6: Set up your focus group. Step 7: Host your focus group.
A focus group is a qualitative fact-finding method involving a small group of five to 10 people discussing a specific topic or issue. A moderator leads the group, poses open-ended questions, and encourages participant discussion and interaction. A focus group aims to gain insights into participants' opinions, attitudes, beliefs, and behaviors about the discussed topic.
Definition: A focus group is a qualitative research method used to gather in-depth insights and opinions from a group of individuals about a particular product, service, concept, or idea. The focus group typically consists of 6-10 participants who are selected based on shared characteristics such as demographics, interests, or experiences.
A focus group is a moderated group discussion on a pre-defined topic, for research purposes. 28,29 While not aligned to a particular qualitative methodology (for example, grounded theory or ...
A Case Study One case study will be used as an example of focus-group research throughout this article. Participants in the case study were undergraduate students who were asked to take part in some institutional research that was intended to inform university policy on the provision of its IT resources. The case study was published in Studies ...
A focus group is a research method or technique that is used to collect opinions and ideas regarding a concept, service, or product. Follow the below steps to conduct it: A researcher must be careful while recruiting participants. Members need adequate knowledge of the topic so that they can add to the conversation.
Based on your research goal or goals, this guide should include a list of focus group questions or topics you want to cover during the session, and strike a good balance between structured and flexible - so you can gather the data you need while not discouraging spontaneous conversation. 6. Conduct the focus group.
Focus groups use a group setting to generate data different to that obtained in a one-to-one interview. The group context may allow for better examination of beliefs, attitudes, values, perspectives, knowledge and ideas. Focus groups can be useful in action research methodology and other study designs which seek to empower research participants.
ISBN: 9781446248645. Publication Date: 2015-10-01. This sharp, stimulating title provides a structure for thinking about, analysing and designing case study. It explores the historical, theoretical and practical bones of modern case study research, offering to social scientists a framework for understanding and working with this form of inquiry.
A focus group is a qualitative research method that involves facilitating a small group discussion with participants who share common characteristics or experiences that are relevant to the research topic. The goal is to gain insights through group conversation and observation of dynamics. In a focus group: A moderator asks questions and leads a group of typically 6 to 12 pre-screened ...
What Is a Focus Group? Definition: A focus group is a qualitative, attitudinal research method in which a facilitator conducts a meeting or workshop (typically about 1-2 hours long) with a group of 6-9 people to discuss issues and concerns about their experiences with a product or service. The term "focus" relates to the role of the facilitator, who maintains the group's focus on ...
Qualitative Research: Introducing focus groups. This paper introduces focus group methodology, gives advice on group composition, running the groups, and analysing the results. Focus groups have advantages for researchers in the field of health and medicine: they do not discriminate against people who cannot read or write and they can encourage ...
Focus groups have been widely used in health research in recent years to explore the perspectives of patients and other groups in the health care system (e.g., Carr et al., 2003; Côté-Arsenault & Morrison-Beedy, 2005; Kitzinger, 2006). They are often included in mixed-methods studies to gain more information on how to construct questionnaires ...
Social science researchers can derive multiple benefits from using focus groups. One is that focus groups are an economical, fast, and efficient method for obtaining data from multiple participants (Krueger & Casey, 2000), thereby potentially increasing the overall number of participants in a given qualitative study (Krueger, 2000).Another advantage to focus groups is the environment, which is ...
A focus group, a cornerstone of qualitative research employed in market research and social sciences, gathers a select group of 6 to 10 participants. This method facilitates a guided discussion led by a skilled moderator, aiming to delve into participants' opinions, perceptions, and attitudes regarding a specific topic.
Despite the well-documented advantages of focus group data collection, modern challenges for qualitative health researchers exist. Health research funding is increasingly competitive, recruiting health-care professionals to participate in qualitative health research is challenging due to increasing busyness in clinical environments, vast geographical distances between research sites hinder ...
Focus Group Discussion as a Tool to Assess Patient-Based Outcomes, Practical Tips for Conducting Focus Group Discussion for Medical Students—Learning With an Example ... Strategies for improving patient recruitment to focus groups in primary care: a case study reflective paper using an analytical framework. BMC Med Res Methodol. 2009; 9:65 ...
A Case Study. One case study will be used as an example of focus-group research throughout this article. Participants in the case study were undergraduate students who were asked to take part in some institutional research that was intended to inform university policy on the provision of its IT resources.
Practitioners and researchers are conducting more focus groups online as a qualitative data collection method, yet rigorous methodological studies investigating the diversity of findings versus traditional in-person focus groups are limited. Previous studies primarily focused on health topics, varied on topic scope (broad to sensitive), format ...
Our study sample consisted of 350 African-American men living in Durham, North Carolina. Participants were randomized into either a focus group arm or individual interview arm, and were asked the same open-ended questions about their health-care seeking behavior.
This group is ideal for restaurant focus groups focusing on franchises. The more successful these locations become, the more consumers will demand. But what makes the ideal location for a franchise? Thankfully, management teams will be able to answer these questions based on data from evaluation groups. Restaurant Focus Group Case Study
A CASE STUDY ON THE USE OF FOCUS GROUPS AS PARTICIPATORY RESEARCH Tim Biello Dr. James (Sandy) Rikoon, Thesis Advisor ABSTRACT Participatory approaches to research involve the commitment of a researcher, as well as those supporting the researcher (i.e., academic institutions, funding
Other studies have used focus group discussion to clarify and extend findings, such as motivations for different resource use regimes (Harrison, Baker, Twinamatsiko, ... This is usually the case when working with non-sedentary households especially in the rangelands (e.g. 200). Where such communities or research subjects are involved ...
A strength of our study was the use of individual and focus groups interviews, which enabled a comprehensive exploration of individual and group views on emotional labour of NH professionals. Including professionals involved in direct care and leaders, i.e. nurse and medical coordinators, enabled to capture a diverse set of experiences and ...
This case study describes how the Department of Chemical Engineering at Bath has foregrounded student voice when developing climate and sustainability teaching. It emphasises the link between sustainability and social justice in this context. ... Case study: Student focus groups in Chemical Engineering map path to enhanced climate and ...
case study Relentless focus on participant experience and outcomes We worked closely with the plan sponsor and lifted participant engagement and promoted financial wellness, while looking beyond just the enrollment numbers to deferral rates, investment selections and Qualified Default Investment Alternative utilization rates.
A group has solidarity to the extent that its members are disposed to: (1) share values, aims, or goals; (2) care about those values, aims, or goals; (3) act in accordance with those values, aims, or goals; (4) trust the testimony of other group members with respect to those values, aims, and goals; and (5) feel a sense of belonging to the ...
Issued on: 18 September 2024Deadline: 26 September 2024The World Health Organization (WHO) is seeking regulators and regulatory experts to serve as members on Technical Advisory Group on clinical and policy considerations for new Tuberculosis (TB) vaccines. This "Call for experts" provides information about the advisory group in question, the expert profiles being sought, the process to ...